
Just a friendly reminder….


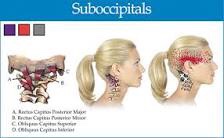
The suboccipitals are a group or four muscles that attach to the transverse and spinous process of C1 and C2 and the occipital bone.
These muscles provide extension side bending and rotation movements between the occiput and C1 and C2. These muscles are often overloaded due to postural strain. A classic example being sitting in front of a computer all day.
When these muscles are overloaded trigger points can develop. Pain and symptoms of trigger points in the suboccipitals include head pain that penetrates into the skull but is difficult to localize.
Patients are likely to describe the pain as “all over” including the occiput, eye and forehead, but without any clarity. Trigger points in these muscles are often associated with tension head aches
.


Fibromyalgia (FM) is a very common condition affecting approximately ten million Americans (2-4% of the population)—with a ratio of about four women to each man with the disease. Part of the diagnosis and treatment challenge is that many of the complaints associated with FM occur in ALL of us at some point, such as fatigue, generalized whole body aches/pains, non-restorative sleep, depression, anxiety, etc. So what is the difference between the FM sufferer and those without it? Let’s take a look!
The primary distinction between patients with FM and the “rest of us” has to do with the word “chronic.” This term means “…persisting for a long time or constantly recurring; long-standing, long-term.” In fact, the term “fibromyalgia” is described as a complex chronic pain disorder that causes widespread pain and tenderness that may present body wide or migrate around the body. It is also known to “wax and wane over time,” meaning it flares up and down, off and on.
The diagnosis of FM is typically made by eliminating every other possible cause. Hence, after blood tests and x-ray or other imaging, the ABSENCE of other problems helps nail down the diagnosis of “primary fibromyalgia.” Then there is “secondary fibromyalgia,” which is DUE TO a known disorder or condition such as after trauma (like a car accident), rheumatoid arthritis, migraine headache, irritable bowel syndrome, “GERD” (which is heart burn due to reflux), pelvic pain, overactive bladder, tempromandibular joint dysfunction (jaw pain, with or without ringing in the ears), or stress. It’s also often accompanied by anxiety, depression, and/or some other mental health condition.
It should be clearly understood that there is no “cure” for FM. It has also been widely reported in many studies that the BEST management approach for FM is through a TEAM of healthcare providers. This team is frequently made up of primary care doctors, doctors of chiropractic, massage therapists, mental / behavioral specialists, physical therapists, and perhaps others (acupuncturist, nutritionist, stress management specialists, and more).
The “general” treatment approach is typically done with medications, cognitive behavioral therapies (CBT), gentle exercise, and manual therapies. Additionally, patients are encouraged to participate in the healing process via self-management strategies that focus on reducing stress and fatigue, optimizing diet, and developing a consistent sleep habit.
Think of the role of the chiropractor as a strong member of the team. A doctor of chiropractic can offer many of the known methods of managing FM described above, as their training includes diet and nutrition, stress management, exercise training, and ability to provide “whole person care.” Treatments delivered in the chiropractic setting like spinal manipulation, mobilization, and massage offer GREAT relief to FM patients! Again, coordinating care between various providers is the best approach, but you need someone willing and able to do that. A doctor of chiropractic is a great choice!
It is very difficult to manage FM on your own. Let a doctor of chiropractic tailor a treatment plan that is appealing to you and your specific interests. Managing FM is definitely NOT a “…one size fits all” approach like an inhaler is for asthma. Each individual’s situation is too highly unique!

We all know what it’s like to have neck pain—whether it’s after a long drive, pinching the phone between the head and shoulder, star-gazing, or from talking to someone who is seated off to the side. There are many causes of neck pain, but the question of the month is, how do chiropractic adjustments help neck pain? Let’s take a look!
Chiropractic, when broken down into its fundamental Greek derivatives, means “hand” (cheir) and “action” (praxis). The technique most often associated with chiropractic is spinal manipulation where a “high velocity, low amplitude” thrust is applied to specific vertebrae in the spine, which does several things: 1) It restores mobility in an area with restricted movement; 2) It stimulates the sensory “neuroreceptors” in joint capsules, which has a muscle relaxing reflex effect; 3) It can affect surrounding neurological structures in certain parts of the spine such as the parasympathetic (cranial & sacral regions) and sympathetic (mid-back) nervous systems, which can have beneficial effects on the digestive system, cardiovascular system, and other body systems not typically thought about when seeking chiropractic care.
Joint manipulation is not new, as it can be traced back to as early as 400 BCE. The profession of chiropractic began in the later 1800s and has grown in popularity ever since. There is now an overwhelming body of evidence that supports spinal manipulation as both a safe and highly effective treatment for neck and back pain, headaches, and many other maladies.
It’s important to note that there are many different types of manual therapies that chiropractors utilize when caring for neck pain patients. There are “low-velocity, low amplitude” or non-thrust techniques that do NOT produce the “crack” that is frequently associated with chiropractic adjustments. The term “mobilization” is often used when referencing these non-thrust methods, and this often incorporates a combination of manual traction (pulling of the neck), left to right and front to back “gliding” movements usually starting lightly and gradually increasing the pressure as tolerated. In many cases, a doctor of chiropractic may utilize a combination of manipulation and mobilization as well as “trigger point therapy” (applying sustained pressure over tight “knots” in muscles), depending on a patient’s needs.


One of our favourites in the office; Thoracic Rotation.
An easy exercise for your upper and mid-back. No equipment required! – (Post link to article and video on your blog or post video directly on your social media account.)”
