Author: bryancobb
Trigger points and headaches
Trigger points are contracted knots of muscle tissue that form in any muscle as a result of overload stress. Trigger points cause pain, referred pain, stiffness and weakness. Trigger points that form in the muscles of the neck and head often refer pain into the head and face. This is one of the most common causes of headache pain. Trigger point massage is an effective way to treat trigger points.


Myofascial Trigger Point characteristics

Myofascial pain syndrome.
Myofascial pain syndrome is a chronic pain disorder. In this condition, pressure on sensitive points in your muscles (trigger points) causes pain in the muscle and sometimes can cause pain spread to other parts of your body. This is called referred pain. Trigger points can also cause stiffness and weakness. This syndrome typically occurs after a muscle has been contracted repetitively. This can be caused by repetitive motions used in jobs or hobbies or by stress-related muscle tension. While nearly everyone has experienced muscle tension pain, the discomfort associated with myofascial pain syndrome persists or worsens. Treatment options include massage therapy, dry needling, and physical therapy. relaxation techniques such as meditation also can help.

Strength training is as important as cardio – and you can do it from home during COVID-19
Got a stiff neck??
One of the most common causes of a stiff neck are trigger points in the levator scapulae muscle. This muscle runs up the side of the neck from the top of the shoulder blade. It helps to shrug the shoulders and move and stabilize the neck. When trigger points form in this muscle they will produce pain and stiffness in the neck. Deep tissue trigger point massage applied to these knots is an effective treatment method.

Trigger points in the abdominal muscles.
Myofascial trigger points in the abdominal muscles are very common. These muscles are responsible for trunk movement and stability, and are engaged in some way during most activities. As a result trigger points will easily form. These knots will often refer pain into the lower or mid back in a horizontal strip. Trigger points in the abdominal muscles are often overlooked as a source of back pain. Once developed, a trigger point won’t release on its own. A therapeutic modality such as trigger point massage is needed to release the tissue.

Trigger point pain
Myofascial trigger points are contracted knots that form in muscle tissue. They form from overload stress placed on the muscle. Both chronic stress such as poor posture and acute stress such as an injury will cause trigger points to form. Once there a trigger point will produce pain, referred pain, weakness and stiffness. Trigger points don’t go away with rest or with time, some form of intervention such as trigger point massage is needed to treat the injured muscles. Trigger points can form in any muscle in the body and are one of the most common causes of pain.
Trigger points in the hamstrings.

With all the sitting going on these days, tight hamstrings are becoming increasingly common. When your hamstrings are tight they almost certainly have trigger points. These contracted knots in the muscle are a common cause of pain felt in the back of the leg, knee and lower buttocks. Trigger points don’t go away with rest or stretching, they need a therapeutic intervention such as massage to be released.
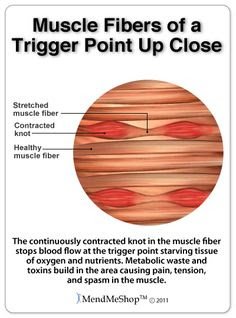
Anatomy of a trigger point.

