The Levator scapula is a muscle in your neck that originates on the transverse processes of C1-C4 and inserts on the superior part of the medial border of the scapula. The primary actions of this muscle are to elevate the scapula and rotate the glenoid fossa downward. It also rotates the neck to the same side and assists in extension. When this muscle is tight it restricts neck rotation resulting in the classic “stiff neck”. With a forward head position the Levator is often stretched and over worked. To help combat this you must get the head back by releasing the anterior chest and neck muscles. Trigger points in this muscle refer pain into the angle of the neck and down the shoulder blade.
How can a low speed crash cause injury?
There is certainly a lot of interest in concussion these days between big screen movies, football, and other sports-related injuries. Concussion, traumatic brain injury (TBI), and mild traumatic brain injury (mTBI) are often used interchangeably. Though mTBI is NOT the first thing we think about in a low-speed motor vehicle collision (MVC), it does happen. So how often do MVC-related TBIs occur, how does one know they have it, and is it usually permanent or long lasting?
Here are some interesting statistics: 1) The incidence rate of fatal and hospitalized TBI in 1994 was estimated to be 91/100,000 (~1%); 2) Each year in the United States, for every person who dies from a brain injury, five are admitted to hospitals and an additional 26 seek treatment for TBI; 3) About 80% of TBIs are considered mild (mTBI); 4) Many mTBIs result from MVCs, but little is known or reported about the crash characteristics. 5) The majority (about 80%) of mTBI improve within three months, while 20% have symptoms for more than six months that can include memory issues, depression, and cognitive difficulty (formulating thought and staying on task). Long-term, unresolved TBI is often referred to as “post-concussive syndrome.”
In one study, researchers followed car crash victims who were admitted into the hospital and found 37.7% were diagnosed with TBI, of which the majority (79%) were defined as minor by a tool called Maximum Abbreviated Injury Scale (MAIS) with a score of one or two (out of a possible six) for head injuries. In contrast to more severe TBIs, mild TBIs occur more often in women, younger drivers, and those who were wearing seatbelts at the time of the crash. Mild TBI is also more prevalent in frontal vs. lateral (“T-bone”) crashes.
As stated previously, we don’t think about our brains being injured in a car crash as much as we do other areas of our body that may be injured—like the neck. In fact, MOST patients only talk about their pain, and their doctor of chiropractic has to specifically ask them about their brain-related symptoms.
How do you know if you have mTBI? An instrument called the Traumatic Brain Injury Questionnaire can be helpful as a screen and can be repeated to monitor improvement. Why does mTBI persist in the “unlucky” 20%? Advanced imaging has come a long way in helping show nerve damage associated with TBI such as DTI (diffuse tensor imaging), but it’s not quite yet readily available. Functional MRI (fMRI) and a type of PET scanning (FDG-PET) help as well, but brain profusion SPECT, which measures the blood flow within the brain and activity patterns at this time, seems the most sensitive.
We realize you have a choice in whom you consider for your health care provision and we sincerely appreciate your trust in choosing our service for those needs. If you, a friend, or family member requires care for Whiplash, we would be honored to render our services.
Hip Abductor Weakness
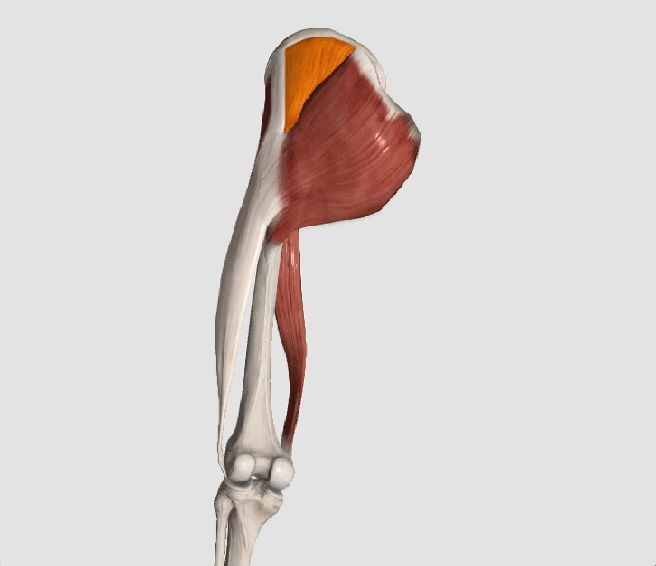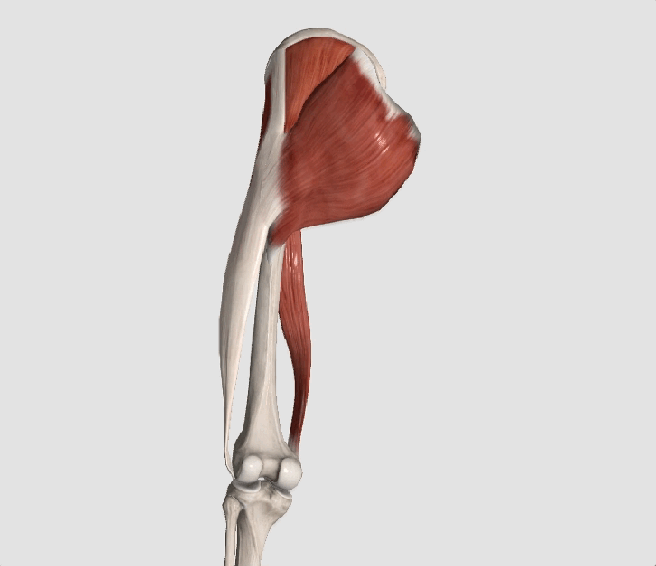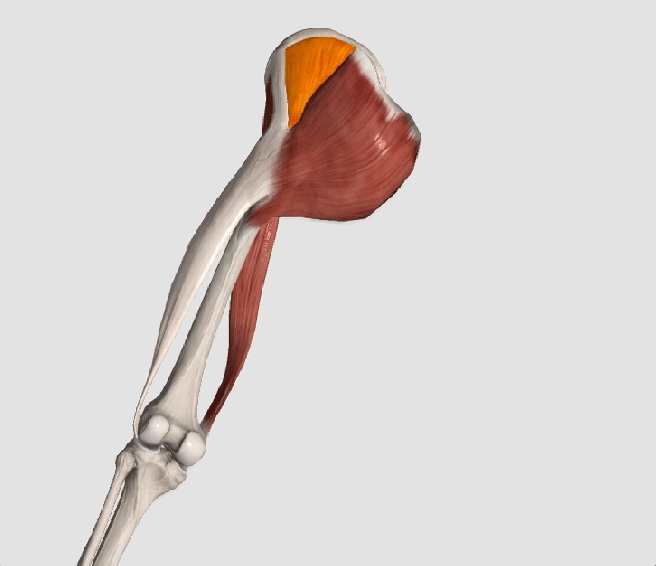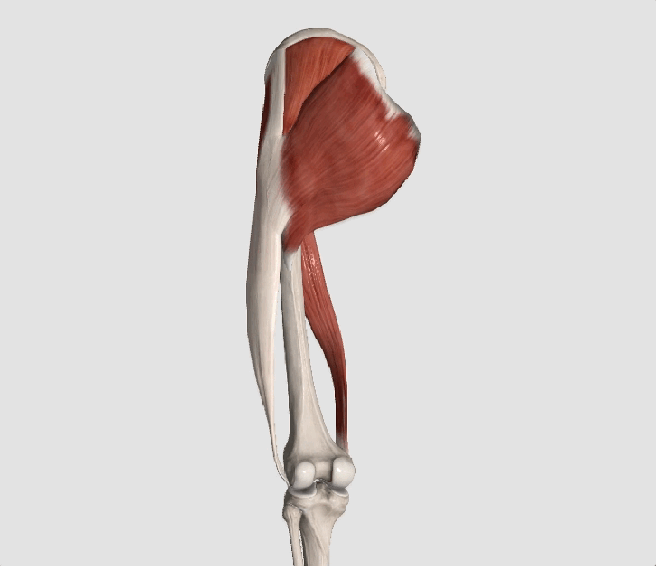
* The gluteus medius contributes approximately 70% of the abduction force required to maintain pelvic leveling during single leg stance.
* Hip abductor strength is the single greatest contributor to lower extremity frontal plain alignment during activity.
* There is no “typical” presentation for hip abductor weakness, but the problem must be considered in any patient with lower chain symptomatology, particularly those with hip tendinopathy, greater trochanteric pain syndrome, iliotibial band syndrome, patellofemoral pain syndrome, ACL injury, medial knee pain, and lower back pain.
*Hip abductor weakness is often accompanied by lower crossed syndrome – a larger pattern of biomechanical dysfunction involving weakness of the abdominal wall and hypertonicity in the hip flexors and paraspinal musculature. Evaluation should include a relatively global assessment of lumbopelvic muscle and joint function. Additionally, clinicians should assess for the presence of foot hyperpronation in patients with hip abductor weakness.
Referenced from:
ChiroUp.com “Hip Abductor Weakness Clinical Pearls

Food Myth #3
Avoid eggs because of their cholesterol content.
Eggs got a bad rep years ago because we thought they contributed to a rise in levels of LDL (Bad) cholesterol. The most recent research shows that eggs don’t actually contribute to high cholesterol at all and are a great source of iron, zinc, lutein, vitamin D and choline, not to mention a cheap, easy source of protein.
So go ahead with your eggs tomorrow morning! You’ll be healthier for it.

https://www.heartfoundation.org.au/healthy-eating/food-and-nutrition/protein-foods/eggs
https://www.eatrightontario.ca/en/Articles/Heart-Health/Understanding-Eggs-and-Cholesterol-How-many-eggs.aspx
https://www.health.harvard.edu/heart-health/are-eggs-risky-for-heart-health
A Few Sleep Tips From Us To You

Your mattress and the position you sleep in may affect your spine.
✓ Choose a mattress that provides medium or firm support, such as a traditional coil spring or adjustable airbed. Avoid waterbeds, thick pillow tops and soft, sagging mattresses.
✓ Always sleep on your back with a pillow either underneath your knees or on your side with a pillow between your knees. Avoid sleeping on your stomach.
✓ Keep your neck and back covered while sleeping to avoid drafts that could cause potential muscle spasms.
Here are a couple of tips to help you get in and out of bed more comfortably:
✓ To lie down: Sit on the edge of the bed, pull your arms to your sides and tilt your body into the bed, maintaining the bend of your knees at 45 degrees. Finally, bring your feet into in a lying position or roll onto your back.
✓ To get up: From a side-lying position with your knees bent, push your body upright into a sitting position, swinging your legs over the edge of the bed as you rise.
If you find that you wake up sore then you may be suffering from any number of conditions that get worse overnight.
What is health?

Workstation Ergonomics

Ergonomics is the science of adjusting your workstation to minimize strain in the following ways:
✓ Maintain proper body position and alignment while sitting at your desk – Hips, knees and elbows at 90 degrees, shoulders relaxed, feet flat on floor or footrest.
✓ Wrists should not be bent while at the keyboard. Forearms and wrists should not be leaning on a hard edge.
✓ Use audio equipment that keeps you from bending your neck (i.e., Bluetooth, speakerphones, headsets).
✓ Monitors should be visible without leaning or straining and the top line of type should be 15 degrees below eye level.
✓ Use a lumber roll for lower back support.
✓ Avoid sitting on anything that would create an imbalance or uneven pressure (like your wallet).
✓ Take a 10-second break every 20 minutes: Micro activities include: standing, walking, or moving your head in a “plus sign” fashion.
✓ Periodically, perform the “Brugger relief position” (See video below) -Position your body at the chair’s edge, feet pointed outward. Weight should be on your legs and your abdomen should be relaxed. Tilt your pelvis forward, lift your sternum, arch your back, drop your arms, and roll out your palms while squeezing your shoulders together. Take a few deep cleansing breaths.
Carpal Tunnel Facts #1
If tingling/numbness primarily affects your thumb, index, third, and ring fingers, it very well could be carpal tunnel syndrome, or CTS. Chances are you’ve probably had this condition for months or even longer but it’s been more of a nuisance than a “major problem” and therefore, you probably haven’t “bothered” having it checked out. Let’s take a look at some “facts” about CTS!
WHAT IS CTS? CTS is basically a pinched nerve (the median nerve) that occurs on the palm side of the wrist that innervates the three middle fingers and the thumb on the palm side. This nerve starts in the neck, runs through the shoulder to enter the arm, and travels down the palm side forearm through the carpal tunnel. The carpal tunnel is made up by eight small bones (called “carpal bones”) that form the roof and walls of the tunnel. The floor of the tunnel is a ligament called the transverse carpal ligament. The median nerve lies immediately on the floor, and deeper inside the tunnel are nine tendons that connect the muscles of our forearm to the fingers, which allow us to make a fist and grip. When swelling occurs inside the tunnel, the nerve is pinched against the floor (ligament) and symptoms occur.
SYMPTOMS OF CTS: Symptoms typically start gradually with tingling, numbness, burning, itching, or a “half-sleep” feeling in the palm of the hand, thumb, and middle three fingers. The fingers can feel swollen and weak, though “swelling” is usually NOT visible. CTS can occur in one or both hands, but it is usually worse in the dominant hand. Initially, you may only notice symptoms at night or in the morning. As CTS worsens, sleep interruptions, grip weakness, difficulty distinguishing hot from cold, increased pain, pain radiating up the arm, and more may occur.
CAUSES OF CTS: There are many causes of CTS that often occur in combination: 1) Heredity or genetics — being born with a smaller wrist than others; 2) Trauma — a fall on the arm/hand (sprain or fracture); 3) Overuse of the arms/hands (like repetitive line work, serving tables, or using a computer), 4) Hormonal causes — during menstruation, with pregnancy, during menopause, diabetes, hypothyroid, overactive pituitary gland; 5) Rheumatoid arthritis; 6) Fluid retention; 7) Cysts, tumors, or spurs inside the tunnel; 8) Vibrating tools, 9) Hobbies such as knitting, sewing, crocheting; 10) sports; or 11) an “Insidious” or unknown cause!
CTS RISK FACTORS: 1) Gender: Women are three times more likely to develop CTS, possibly because they generally have a smaller carpal tunnel than men, in addition to hormonal differences; 2) Diabetes or other metabolic disorders; 3) Adults, especially >50 years old; 4) Job demands.
CTS DIAGNOSIS: Your doctor of chiropractic will review your patient history and then evaluate the neck, shoulder, arm, and hand, as ALL can be involved in producing CTS-like symptoms. He/she may also order blood tests (to check for diabetes, thyroid levels, rheumatoid arthritis, etc.) and/or an EMG/NCV (electromyogram/nerve conduction studies) to test for nerve damage.
We will FINISH THIS interesting discussion next week covering: Treatment, prevention, and research.

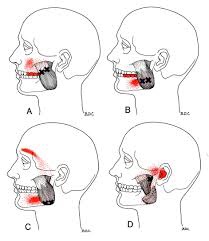
Trigger points in the masseter muscle

The masseter is the main muscle that moves your jaw. It originates on the zygomatic arch and maxilla, and inserts on the coronoid process and Ramus of the mandible. It’s actions are to elevate the mandible and close the jaw. The deep fibres of this muscle also retrude the mandible. This muscle commonly harbours trigger points as a result of teeth grinding. Trigger points in this muscle are often also associated with tmj dysfunction. Trigger points in the upper part of this muscle will refer pain to the upper molars and maxilla often felt as sinusitis. Trigger points in the lower portion of this muscle refer to the lower molars and temple. All trigger points can cause tooth sensitivity