In 2016, researchers at Curtin University in Perth examined the seated posture and health data of 1,108 17-year olds in an effort to determine if any particular posture increased the risk of headaches/neck pain among late adolescents.
Among four posture subgroups—upright, intermediate, slumped thorax, and forward head—the researchers observed the following: participants who were slumped in their thoracic spine (mid-back region) and had their head forward when they sat were at higher odds of having mild, moderate, or severe depression; participants classified as having a more upright posture exercised more frequently, females were more likely to sit more upright than males; those who were overweight were more likely to sit with a forward neck posture; and taller people were more likely to sit upright.
While they found biopsychosocial factors like exercise frequency, depression, and body mass index (BMI) ARE associated with headaches and neck pain, their data did not suggest any one particular posture increased the risk of neck pain or headaches more than any other posture among the teenagers involved in the study.
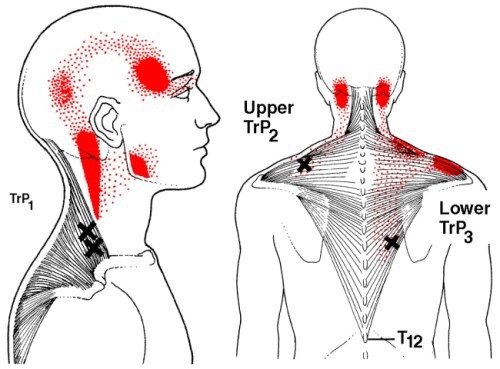
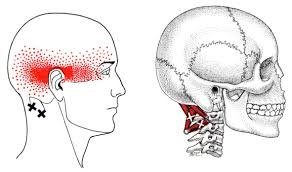
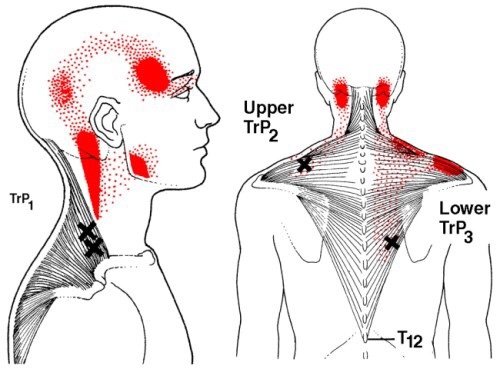
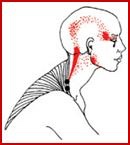
This is noteworthy as studies with adults do indicate the risk for neck pain and headaches is greater in individuals with poor neck posture. In particular, postures such as forward head carriage, pinching a phone between the ear and shoulder, and prolonged neck/head rotation outside of neutral can all increase the risk of cervical disorders. This suggests that in younger bodies, the cause of neck pain and headaches may be multifactoral and not limited to just poor posture and that treatment must address all issues that may increase one’s risk for neck pain/headaches in order to reach a desired outcome.
The good news is that chiropractic has long embraced the biopsychosocial model of healthcare, looking at ALL factors that affect back and neck pain and quality of life. Through patient education, spinal manipulation, mobilization, exercise training, the use of modalities, and more, chiropractors can greatly help those struggling with neck pain and headaches!