Fitness
Snow Shoveling Tips!

2 Critical Questions
Evidence-based chiropractors must routinely answer two questions:
- Does this patient have inflamed tissue or degenerated tissue?
- Has this injury resulted in a compensatory movement pattern?
Chiropractors treat the cause of dysfunction and not the just the pain—right? This becomes more challenging when patients present with an assortment of orthopedic diagnoses. Let’s be honest, we see the worst of the worst on a daily basis, and we are often the last option.
Identifying IF inflammation is a source of pain may be one of the biggest differentiators in your initial exam.
Chiropractors see patients in pain resulting from acute injuries. Newly injured tissue often contains an inflammatory component for healing. However, emerging clinical research tells us that reoccurring painful conditions often lack an inflammatory component. Effective treatment of pain is dependent on a clear understanding of whether inflammation is present or not.
Learn how to identify chemical vs. mechanical pain
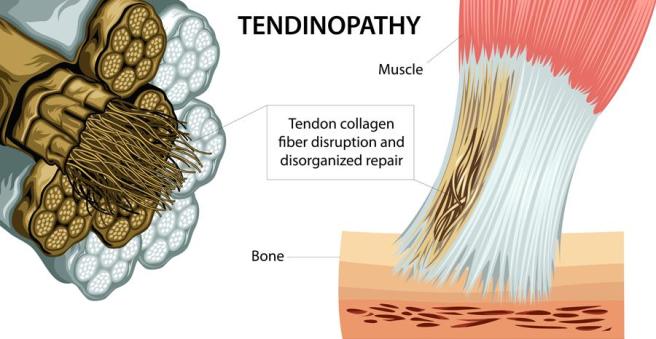
Many chronic tendon problems are not the result of ongoing inflammation, rather failed inflammation. Chronic failed inflammation results in tissue degeneration that diminishes long-term tissue capacity, size, and function. Tendons, when degenerated, exhibit lower stiffness. A failed healing response results in proliferation of tissue with decreased load transfer and elastic capability. We sometimes refer to this as scar tissue. This deficit must be accounted for during locomotion. Diminished tendon load transfer will lead to widespread biomechanical dysfunction. The patient must be willing to change their movement pattern or habits to stop this process.
Chronic problems often lead to widespread biomechanical dysfunction.
We have all seen the patient with chronic, but intermittent, plantar fasciitis who develops subsequent knee, hip, or back pain. Human movement is coordinated by a hierarchal system. The CNS initiates, controls and executes movement patterns. The human body knows movements—not muscles. If one tissue in the loop loses its integrity the patient may develop a new movement pattern. This new movement pattern may not be efficient to all the tissue components and result in new injuries. Our tissue only has a certain capacity. Muscles and tendons will strain, ligaments will sprain, and bones will break at different rates and/or amounts of load. Rehab should focus on optimal movement patterns instead of strengthening isolated muscles.
Let’s examine a patient with Achilles tendinosis?
Patients with Achilles pain will often favor the outside of their foot. Pain will result in an adaptive behavior altering the activity of agonist, synergist and antagonist muscles. A recent study in the Journal of Physiology highlighted this compensatory behavior:
“This was seen during single-legged hopping, where the contribution from the triceps surae muscle to the plantar flexors was decreased and the co-contraction from the tibialis anterior muscle was also decreased on the involved side in individuals with Achilles tendinosis. This may be attributed to the protective mechanism shielding the already injured tendon from further injury or even rupture.” (1)
If the agonist and antagonists have decreased activity, then how do these patients transfer load while walking?
“The EMG activity of the synergist muscle, the peroneal longus muscle in the present study, increased to compensate for the mechanical deficit resulting from the compliant Achilles tendon and to achieve the task goal.”
These patients have now condemned their gait cycle to walk on a supinated foot that transfers compensatory repercussions to the knee and hip. The increased load on the peroneal muscles may also result in injury in time. This is not an isolated problem, rather the typical continuum of an “…itis” to an “…opathy” over time. These are not isolated lesions; rather the start of widespread biomechanical dysfunction that may result in any number of orthopedic diagnosis. The authors conclude:
“Pain is a signal of tissue damage, although damaged tissues are not always painful.”
Excellent chiropractic clinical outcomes require that providers look upstream and downstream for biomechanical co-conspirators. ChiroUp helps your patients recognize how specific orthopedic conditions change movement patterns. Preselected exercise protocols incorporate ideal movement patterns during the rehab process. In the case of tendinopathy, ChiroUp protocols incorporate eccentric exercise to facilitate and strengthen the damaged tissue and prevent recurrence of pain.
Reference
- Chang Y-J, Kulig K. The neuromechanical adaptations to Achilles tendinosis. The Journal of Physiology. 2015;593(Pt 15):3373-3387. doi:10.1113/JP270220.
Canada’s Pain Crisis
In a nation of only 36 million people, over 5 million people turned to opioid use for their pain despite the availability of better options. Opioids should never be the first step in pain management; preventing overuse takes education of both the public who are using and the professionals prescribing these drugs.
At Aberdeen Chiropractic we are proud to be part of the solution to Canada’s opioid crisis by providing safe, effective care for back pain, neck pain and headaches. Our goal is to assess, correct and prevent your pain with a variety of interventions including Chiropractic, Acupuncture, Laser, Exercise Rehabilitation and Trigger Point Therapy.

The Hip Cycle
Meet the Hip Cycle. A great way to activate those pesky hip stabilizers and get your lower limb ready for squatting, running, sports or even just walking.
You can thank me later.
1. Side lying with back and shoulders against a wall so you can’t roll back.
2. Bend your bottom leg and put the sole of your foot against the wall to be more stable.
3. Start position is with your foot directly in line with your hip. Do not let it get any lower than that. The highest point of your foot needs to be the bump on the outside of your ankle.
Do 5-10 reps of each of the following without rest between exercises twice a day. The goal is 20 reps each.
a. 6″ leg raises in abduction
b. Knee up to chest (90* knee and hip)
c. 12″ leg raises into abduction
d. Bicycling (knee up to chest, extend knee and sweep back to start with leg straight)
e. Clockwise circles
f. Counterclockwise circles
Good luck.
How does my neck cause headaches?

Headaches can arise from many different causes. A partial list includes stress, lack of sleep, allergies, neck trauma (particularly sports injuries and car accidents), and more. In some cases, the cause may be unknown.
A unique common denominator of headaches has to do with cervical spine anatomy, in particular the upper part of the neck. There are seven cervical vertebrae, and the top three (C1-3) give rise to three nerves that travel into the head. These nerves also share a pain nucleus with the trigeminal nerve (cranial nerve V), which can route pain signals to the brain.
Depending on which nerve is most irritated, the location of the headache can vary. For example, C2—the greater occipital nerve—travels up the back of the head to the top. From there, it can communicate with another nerve (cranial nerve V or the trigeminal nerve), which can refer pain to the forehead and/or behind the eye.
When C1—the lesser occipital nerve—is irritated, pain travels to the back of the head, while irritation to C3—the greater auricular nerve—results in pain to an area just above the ear. When a nerve is pinched, the altered sensation can include pain, numbness, tingling, burning, itching, aching, or a combination of these sensations.
These are classified as cervicogenic headaches (CGH), and as the name implies, the origin of pain/altered sensation arises from the neck.
A 2013 study reviewing the literature on CGH found that manipulation and mobilization improved pain, disability, and function. The most effective approach included manipulation combined with neck-upper back strengthening exercises.
But what about migraine headaches? Migraines are vascular headaches, and some (but not all) are preceded by an aura or a pre-headache warning that may include blurry vision, tingling, strange olfactory sensations, etc. One study of 127 migraine sufferers reported fewer attacks and less medication required by those who received chiropractic care.
The good news is that spinal manipulation is very safe, and a trial is often very rewarding for many types of headaches.
Can We Prevent Carpel Tunnel?
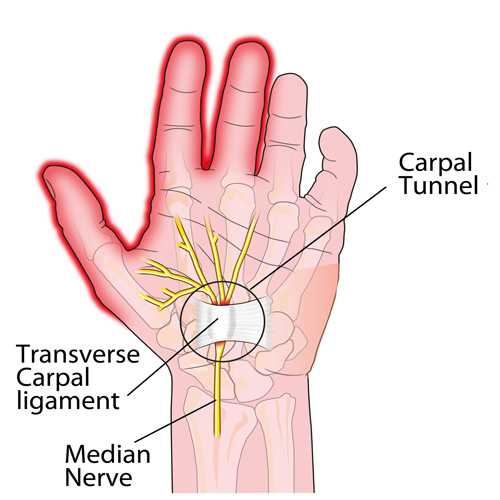
Carpal tunnel syndrome (CTS) is the most common of the many “entrapment neuropathies”— nerve pinches in the arms or legs—likely because we use our hands and fingers repetitively for long time frames at work and during many of our hobbies. In addition, the wrist is a very complicated joint because it’s not a simple ball-and-socket or hinge, like the hip, elbow, or knee.
The wrist is made up of eight small “carpal” bones that are all shaped very differently and fit together a bit like a puzzle. These eight bones are lined up in two rows of four bones that form the “roof“ of the tunnel.
The shape of the tunnel changes with different activities, and the contents within the tunnel have to accommodate for this. Nine of the tendons that allow the hand to move the fingers also travel through the tunnel. Look at the palm-side of your wrist as you wiggle your fingers. See all the activity going on there? The median nerve travels through the tunnel as well, just under the “floor”, which is a very strong ligament that stretches from the pinky to the thumb-side of the tunnel.
Virtually ANY condition that increases the pressure inside the already tightly packed tunnel can create CTS symptoms like numbness, tingling, burning, etc. Over time, grip strength may weaken, causing one to accidentally drop objects.
To add to the causation list of CTS, conditions like obesity, pregnancy, diabetes, hypothyroid, rheumatoid arthritis (and other “arthropathies”), taking birth control pills (BCPs), and more can cause CTS without any increase in hand/wrist activities!
So HOW can we prevent CTS?
First, consider your job and your “workstation.” There are ergonomic keyboard and mouse options that can help you maintain a “neutral” wrist posture. If you have to bend your wrist a lot to do your work tasks—like placing items in a package, assembly work, etc.—see if you can change the angle of the package or assembly set up that allows your wrist to be straight, NOT BENT! Also, sit/stand up straight, chin tucked back, and DON’T SLOUCH!
A “night splint” forces the wrist to stay straight and can REALLY help! Managing your weight and health (manage your diabetes, thyroid, and medications that increase swelling like BCPs) is VERY important! There are also natural anti-inflammatory vitamins and herbs like ginger, turmeric, and bioflavonoid you may want to consider—your doctor of chiropractic can help you with this!
Chiropractors can manage CTS very well and can frequently help patients avoid the need for a surgical release. The “KEY” is to not wait—get treated early on!
Posture Matters!

Why Chiropractic?

What is wrong with my shoulder?


Shoulder pain is a REALLY common problem that can arise from many causes. There are actually several joints that make up the shoulder, so shoulder injuries can be quite complex!
Probably the most common source of shoulder pain arises from the muscle tendons and the bursa—the fluid-filled sacs that lubricate, cushion, and protect the sliding tendons near their attachment to bone. The rotator cuff is made up from a group of four muscles and their connecting tendons. Typically, when the tendons tear, the bursa swells and “impingement” occurs. When this happens, it’s very painful to raise the arm up from the side.
The term “strain” applies to injuries of the muscles and tendons and are classified as mild, moderate, or severe (some refer to this as first, second, and third degree tears), depending on the amount of tissue that has torn. Overexertion, overuse, sports injuries, dislocation, fracture, frozen shoulder, joint instability, and pinched nerves can all give rise to shoulder pain.
The diagnosis of what’s actually causing a patient’s shoulder pain is often determined by the history of how the injury occurred, or the “mechanism of injury.” This is followed up by measuring the range of motion and performing provocative tests to see which positions bother the shoulder the most. A doctor may use X-rays to assess for fracture/dislocation and an MRI to assess muscle tendon tears, labral tears (a rim of cartilage surrounding the glenoid fossa or cup of the ball & socket joint), and other soft tissue injuries.
People with jobs that require heavy lifting or repetitive pounding (carpenters and jack-hammer operators, for example), who play sports such as football and rugby, and those who smoke, have diabetes, and/or an overactive thyroid are at higher risk of injury. Because the shoulder joint is normally not very stable, MANY people tear their rotator cuff or injure their shoulder during their lifetime. One study found 17% of participants had full thickness rotator cuff tears (as opposed to partial tears). The researchers reported that age was an important determinant, as the incidence of full tears was only 6% in those less than 60 years old vs. 30% in those over 60! So obviously, this IS NOT an injury limited to the younger active person!
Outside of a medical emergency, patients should always try non-surgical treatment options first. Doctors of chiropractic offer the shoulder injury patient a non-surgical option that emphasizes exercise and self-management strategies in addition to manual manipulation, mobilization, and more. The most important message is BE PATIENT as these usually take time to manage, often up to a year.

