
Did you know that sleeping on your back puts approximately 50 pounds of pressure on your spine?
Other positions, such as a side position, may be better.

Did you know that sleeping on your back puts approximately 50 pounds of pressure on your spine?
Other positions, such as a side position, may be better.

Migraines can be life-altering! They can stop us from being able to enjoy a child’s piano recital, participate in family events, go to work, or simply do household chores! Wouldn’t it be nice to have ways to self-manage these miserable, often disabling headaches? Here are some options!
1. RELAXATION THERAPY: Search for a calm environment, turn off the lights (photophobia, or light sensitivity, is a common migraine complaint), minimize sound/noise (due to “hyperacusis”), and sleep if possible. Monitor the room temperature and/or use hot/cold compresses to the head and/or neck regions to relax tight muscles (heat) and reduce pain and swelling (cold). Similarly, a warm shower or bath can have similar beneficial effects.
2. SLEEP WELL: Migraines can interfere with falling asleep, they can wake you up during the night, and they are often triggered by NOT getting a good night’s sleep. To improve your sleep quality: a) Establish regular sleeping hours. Wake up and go to bed at consistent times every day, including weekends. b) Keep daytime naps short (20-30 min. max). c) “Unwind” at the end of the day – try soothing music, a warm bath, or reading a favorite book (avoid suspenseful movies). d) Don’t eat/drink too much before bedtime as heavy meals, caffeine, nicotine, and alcohol can interfere with sleep. e) Don’t exercise intensely before bedtime (stretching is fine). f) Eliminate distractions in the bedroom, including TV and bringing work to bed. Close the bedroom door and use a fan to muffle out distracting noises. g) If you take any medications, check for known side effects, as many contain caffeine or other stimulants that can interfere with sleep – including some meds that treat migraines! Talk to your doctor and pharmacist!
3. EAT WELL: Be consistent about when you eat and don’t skip meals (fasting increases the risk for migraine). Keep a food journal to figure out your migraine triggers and avoid foods that commonly trigger migraines like chocolate, aged cheeses, caffeine, and alcohol. Try eliminating these and see how you feel!
4. EXERCISE REGULARLY: This is MOST IMPORTANT for migraine management as it facilitates sleep cycles and stimulates the release of endorphins and enkephlins that help block pain. It also helps fight obesity, which is another risk factor for headaches.
Is there a connection between fibromyalgia (FM) and sleep disturbance? Let’s take a look!
FM is a condition that causes widespread pain and stiffness in muscles and joints. Patients with FM often experience chronic daytime fatigue and some type of sleep problems like getting to sleep, staying asleep, and/or feeling restored in the morning upon waking. The National Institutes of Health estimates between 80-90% of those diagnosed with FM are middle-aged women, although it can affect men and happen at any age. As little as 10-20 years ago, it was hard to find a doctor who “believed” in FM, and it was common for the patient to be told that their pain “was all in their head.” FM has now been studied to the point that we know it is a real condition, and it affects between 2-6% of the general population around the world.
It is well established that sleep disturbance frequently occurs after surgery, which usually normalizes as time passes. One study used a group of healthy women who were deprived of sleep (particularly slow wave sleep) for three days to see if there was a link between sleep disturbance and pain. Results confirmed that the women experienced a decrease in pain tolerance and increased levels of discomfort and fatigue after three days—the same symptoms found among FM sufferers!
Fibromyalgia may have NO known cause, or it can be triggered by other conditions such as repetitive stress injuries, car crash injuries, and other forms of trauma. FM also appears to run in families though it’s still NOT clear if this is a true genetic link or caused by shared environmental factors. Some feel FM is a rheumatoid condition, and though FM is NOT a true form of arthritis, it has been found that people with arthritis are more likely to have FM.
FM sufferers frequently suffer from conditions such as irritable bowel syndrome, chronic fatigue syndrome, migraine headaches, arthritis, lupus, and major depressive disorders. Approximately 20% of FM patients have depression and/or anxiety disorders, and a link between chronic pain and depression exists and seems to play a role in people’s perception of pain.
Because conditions such as sleep apnea can result in symptoms similar to FM, it’s recommended that patients suspected of FM keep a sleep/sleepiness diary in order to rule out sleep apnea as a cause for their condition.
There are many “tips” for improving sleep quality, which we will dive into next month, as these may prove VERY HELPFUL in the management of FM!
If you, a friend or family member requires care for Fibromyalgia, we sincerely appreciate the trust and confidence shown by choosing our services!

There is a lot to be learnt from this video. Dr. Mike Evans does a great job of explaining why we need to KEEP MOVING during and after an episode of low back pain. Check it out!
One of our favourites in the office; Thoracic Rotation.
An easy exercise for your upper and mid-back. No equipment required! – (Post link to article and video on your blog or post video directly on your social media account.)”
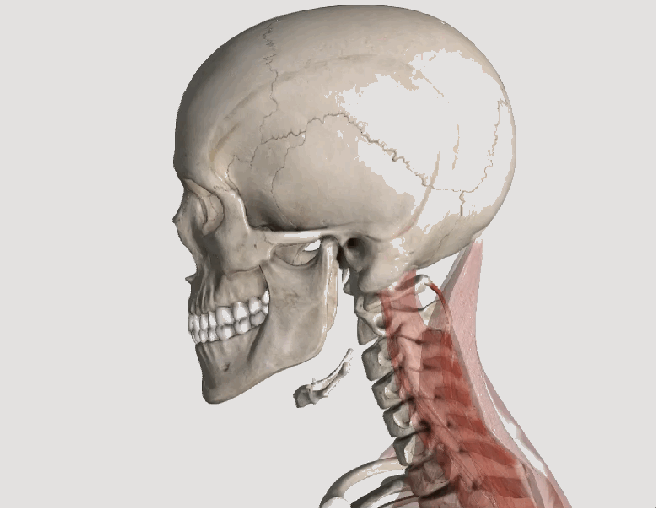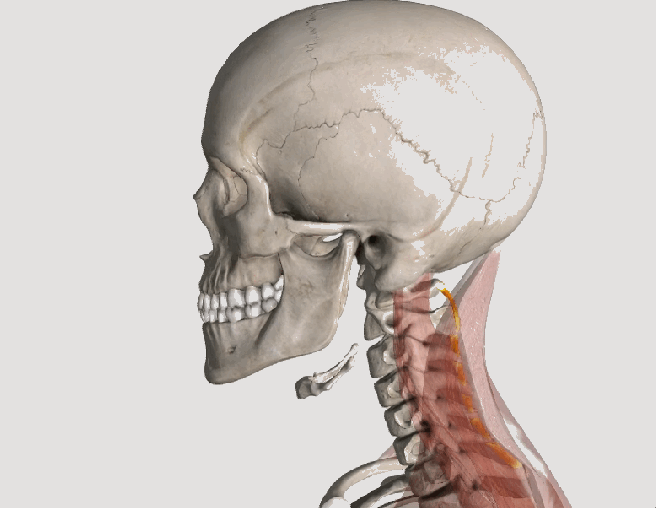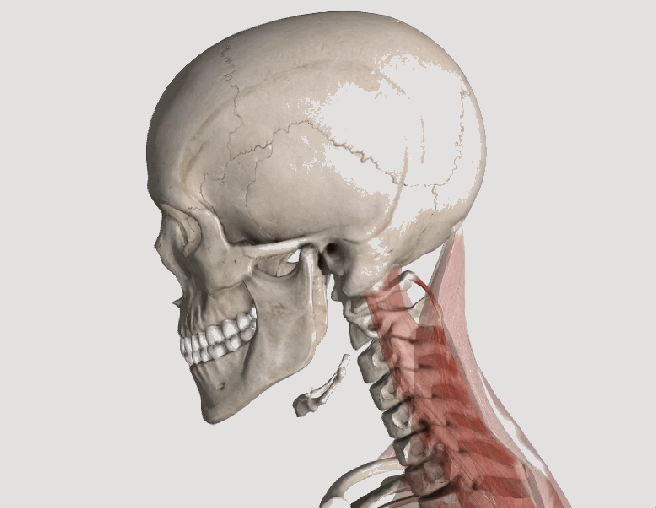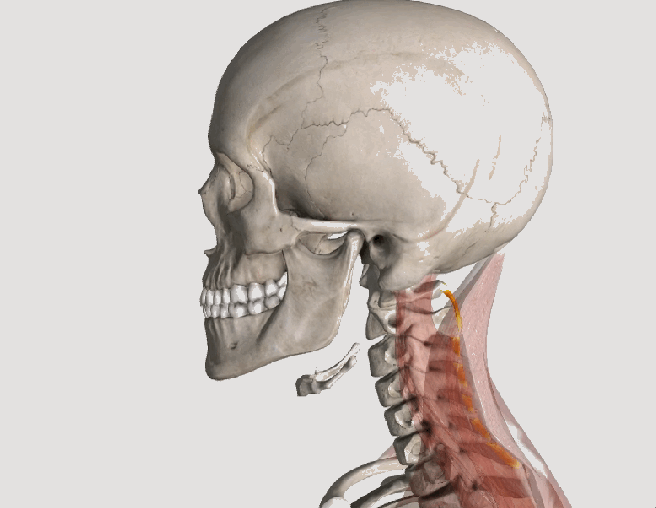
Whiplash is an injury to the soft-tissues of the neck often referred to as a sprain or strain. Because there are a unique set of symptoms associated with whiplash, doctors and researchers commonly use the term “whiplash associated disorders” or WAD to describe the condition.
WAD commonly occurs as a result of a car crash, but it can also result from a slip and fall, sports injury, a personal injury (such as an assault), and other traumatic causes. The tissues commonly involved include muscle tendons (“strain”), ligaments and joint capsules (“sprains”), disk injuries (tears, herniation), as well as brain injury or concussion—even without hitting the head!
Symptoms vary widely but often include neck pain, stiffness, tender muscles and connective tissue (myofascial pain), headache, dizziness, sensations such as burning, prickly, tingling, numbness, muscle weakness, and referred pain to the shoulder blade, mid-back, arm, head, or face. If concussion occurs, additional symptoms include cognitive problems, concentration loss, poor memory, anxiety/depression, nervousness/irritability, sleep disturbance, fatigue, and more!
Whiplash associated disorders can be broken down into three categories: WAD I includes symptoms without any significant examination findings; WAD II includes loss of cervical range of motion and evidence of soft-tissue damage; and WAD III includes WAD II elements with neurological loss—altered motor and/or sensory functions. There is a WAD IV which includes fracture, but this is less common and often excluded.
Treatment for WAD includes everything from doing nothing to intensive management from multiple disciplines—chiropractic, primary care, physical therapy, clinical psychology, pain management, and specialty services such as neurology, orthopedics, and more. The goal of treatment is to restore normal function and activity participation, as well as symptom management.
The prognosis of WAD is generally good as many will recover without residual problems within days to weeks, with most people recovering around three months after the injury. Unfortunately, some are not so lucky and have continued neck pain, stiffness, headache, and some develop post-concussive syndrome. The latter can affect cognition, memory, vision, and other brain functions. Generally speaking, the higher the WAD category, the worse the prognosis, although each case MUST be managed by its own unique characteristics. If the injury includes neurological loss (muscle strength and/or sensory dysfunction like numbness, tingling, burning, pressure), the prognosis is often worse.
Chiropractic care for the WAD patient can include manipulation, mobilization, and home-based exercises, as well as the use of anti-inflammatory herbs (ginger, turmeric, proteolysis enzymes (bromelain, papain), devil’s claw, boswellia extract, rutin, bioflavonoid, vitamin D, coenzyme Q10, etc.) and dietary modifications aimed at reducing inflammation and promoting healing.
* 83% of those patients involved in an MVA will suffer whiplash injury and 50% will be symptomatic at 1 year.
* 90% of patients with neurologic signs at onset may be symptomatic at 1 year.
* 25- 80% of patients who suffer a whiplash injury will experience late-onset dizziness
* Clinicians should be observant for radiographic signs of instability, including interspinous widening, vertebral subluxation, vertebral compression fracture, and loss of cervical lordosis.
* Horizontal displacement of greater than 3.5 mm or angular displacement of more than 11 degrees on flexion/extension views suggests instability.

As exciting as the holidays can be, the added stress that comes along can really affect how your body functions. Whether you’ll be doing a lot of shopping, cooking, wrapping presents, or attending holiday parties, chances are you’ll be putting your body through a lot more than it’s normally accustomed to and all of this can trigger back and neck pain. Here are 11 tips to help you prepare for a happy and healthy holiday season.
Shopping Tips
• Dress appropriately before heading out for a day of shopping. Wear comfortable low-heeled shoes with arch supports and leave your heavy purse at home. Opt for a light backpack or a fanny pack to carry your personal belongings.
• Drink plenty of water to stay hydrated.
• A long day of shopping, i.e. walking, should be treated like an athletic event. Make sure you stretch before and after.
• Make extra trips to the car to drop off your goods so you don’t have to carry those heavy bags around all day.
• Take advantage of online shopping. Skip the long lines and crowded malls completely and shop from the comfort of your own home.
• Simplify your to-do list by picking up gift cards at the grocery store. You’ll get two errands done in one stop.
Wrapping Tips
• Use a table or a counter to wrap gifts. The floor is a less than ideal spot to do your wrapping. Standing or sitting in a chair will promote better posture and help you avoid back and neck pain.
• Don’t wait until the last minute to wrap all of your gifts. Wrapping a few at a time is best.
Wellness Tips
• Don’t neglect your fitness routine. Although you’ll be busier than normal, it’s important to keep those workouts on your daily to-do list. Even a quick 20-minute
workout is better than skipping it all together and you’ll be helping to manage your stress.
• Get enough sleep. The holidays won’t be as enjoyable if you aren’t catching enough z’s. Make sure you’re getting the recommended 7-9 hours of sleep every night.
• Try to stay on track with your healthy eating. Gaining extra weight will only contribute to back pain and health problems. Before attending a party, make sure you eat something healthy and drink plenty of water to avoid overeating while you’re there. It’s ok to indulge a little with holiday treats, just be sure to be sensible about it.
With some simple preparation, you can manage holiday stressors and ward off debilitating back and neck pain. If you do experience pain this season, please give our office a call. We’re experts at finding the root cause of your pain and can help you get back to a better quality of life.