Most of the tissues in our body are in a constant state of rejuvenation, wherein old cells are removed to be replaced by new. In our skeleton, when the production of new bone cannot keep up with the rate of tear down, our bones become progressively thinner and weaker in a process called “osteoporosis”.

Bone fractures occur when stress to a bone exceeds the bone’s ability to support that load. In healthy vertebrae, significant stress is required to cause a fracture. But in osteoporotic bones, the threshold for injury is lowered to the point that “compression fractures” may occur with seemingly minimal stress like bending, coughing, or sneezing. A compression fracture causes a wedge-shaped collapse of the front of the vertebral “body”- resembling what would occur after stepping on one edge of an aluminum can.
Compression fractures are two to three times more common in women, and the risk of developing the problem increases over time. People who have had a prior compression fracture are at greater risk for developing a subsequent fracture. Additional risk factors for compression fracture include a family history of osteoporosis, low body weight, recent weight loss, smoking, a sedentary lifestyle, poor dietary choices, inadequate calcium or vitamin D intake, excessive alcohol or caffeine intake, and scoliosis. The American Academy of Orthopedic Surgery recommends bone density screening for osteoporosis in all women over age 65 or post-menopausal women who have suffered a compression fracture. If you have not already done so, you should schedule a bone density screening.
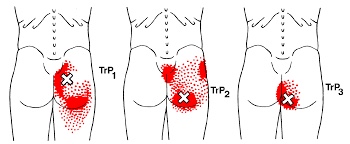
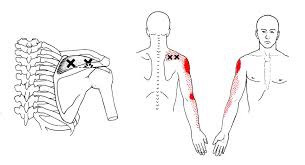
Symptoms of a compression fracture include an “aching” or “stabbing” pain in the back, near the site of fracture. Symptoms can range from minimal to disabling. Often times, pain is referred to the ribs, hip, groin, or buttocks. Be sure to tell your doctor if you have pain or numbness that radiates into your legs, weakness, clumsiness, loss of bowel or bladder control, impotence, fever, unexplained weight loss, night sweats, excessive fatigue, or a history of cancer.
Symptoms from a compression fracture typically lasts for six to 12 weeks. Occasionally, patients will require surgical treatment of a compression fracture, but fortunately, most respond to conservative care. In general, you should maintain a relatively active lifestyle and try to avoid bed rest. If your pain prevents movement, you may talk to your doctor about wearing a brace to limit stress.
Our office will prescribe exercises to help you recover and reduce the risk of subsequent fracture. As your symptoms improve, you can begin incorporating some aerobic exercise, like walking on a treadmill. Studies have shown that light resistance training (i.e. weights and elastic bands) may help you maintain bone density and reduce the risk of future fractures. Supplements to help manage osteoporosis include daily intake of 800-1000 IU of vitamin D and 1000-1200 mg of calcium.