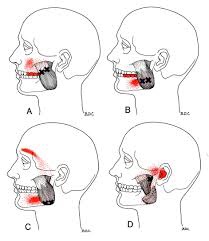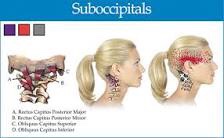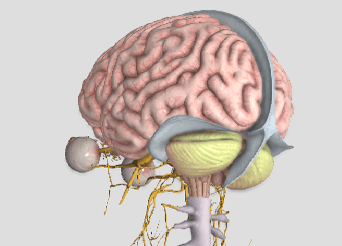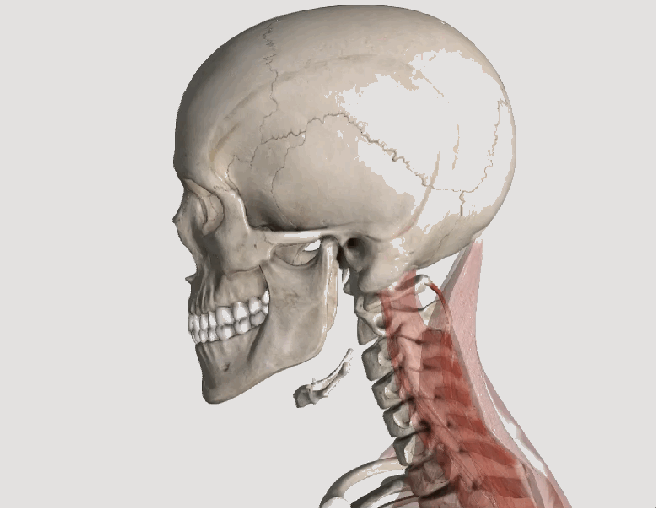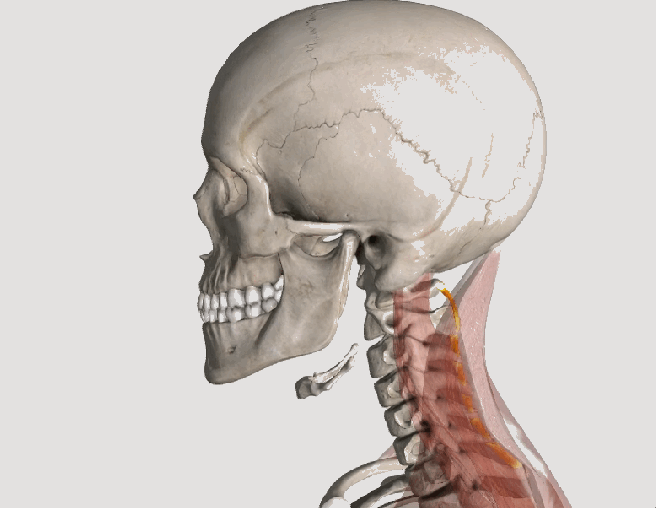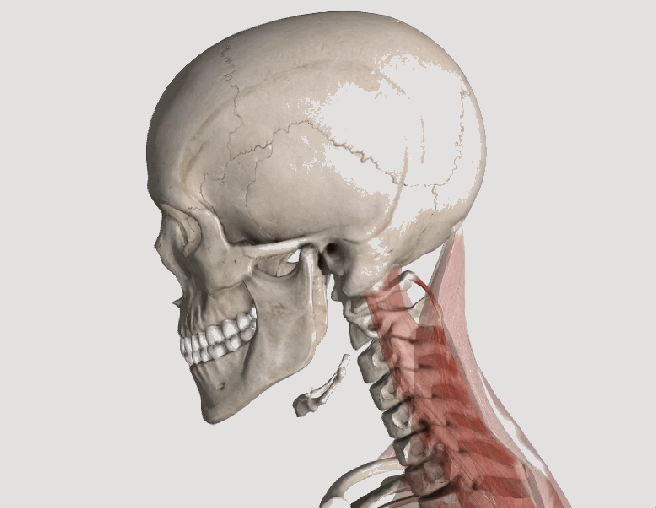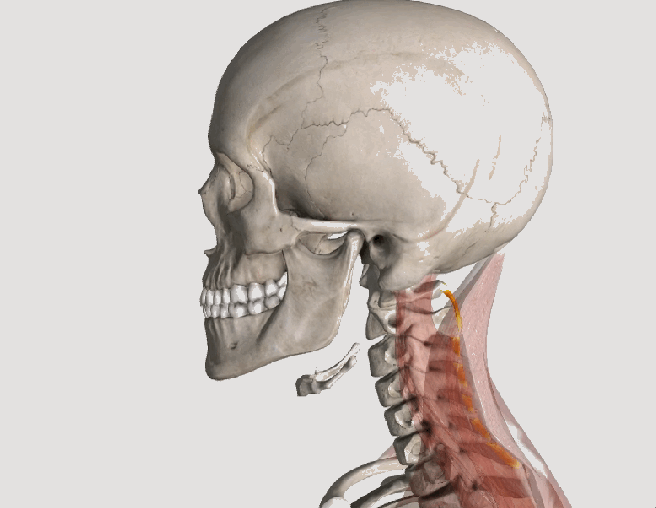
Whiplash, or “Whiplash Associated Disorders” or WAD, is the result of a sudden “crack the whip” of the head on the neck due to a slip and fall, sports injury, a violent act, or most commonly, a motor vehicle collision (MVC), particularly a rear-end collision. In describing “what can I expect” after a whiplash injury, one thing is for certain, there are many faces of whiplash, meaning the degree of injury can range from none to catastrophic depending on many factors, some of which are difficult or impossible to identify or calculate. Let’s take a closer look!
Even though the good news is that most people injured in a car crash get better, 10% do not and go on to have chronic pain, of which about half have significant difficulty working and/or doing desired everyday activities. There is a “great debate” as to the way experts describe “chronic whiplash syndrome” (CWS) as well as how these cases should be managed. Some feel there is something PHYSICALLY wrong in the CWS patient, especially if severe neck or head pain persists for more than one year. There is some proof of this as Dr. Nikolai Bogduk from the University of Newcastle in Australia and colleagues have used selective nerve blocks to anesthetize specific joints in the neck to determine exactly where the pain is generated. The patient then has the option to have that nerve cauterized or burned and pain relief can be significant in many cases. Dr. Bogduk and his group admit that these CWS patients have more psychological symptoms, but they feel this is the result of pain, not the CAUSE.
On the other hand, experts such as Dr. Henry Berry from the University of Toronto report the EXACT OPPOSITE. He argues that it’s not JUST the physical injury that has to be dealt with but also the person’s “state of mind.” Dr. Berry states that when stepping back and looking at all the complaints or symptoms from a distance, “…you see these symptoms can be caused by life stress, the illness ‘role’ as a way of adjusting to life, psychiatric disorders, or even [made up by the patient].” Berry contends that it’s important to tell the patient their pain will go away soon, advises NO MORE THAN two weeks of physical therapy, and sends people back to work ASAP.
Oregon Health Sciences University School of Medicine’s Dr. Michael D. Freeman, whose expertise lay in epidemiology and forensic science, disagrees with Dr. Berry stating that the scientific literature clearly supports the physical injury concept and states, “…the idea that it is a psychological disturbance is a myth that has been perpetuated with absolutely no scientific basis at all.” Dr. Freeman states that 45% of people with chronic neck pain were injured in a motor vehicle crash (which includes three million of the six million of those injured in car crashes every year in the United States).
Here’s the “take home” to consider: 1) CWS occurs in about 10% of rear-end collisions; 2) Some doctors feel the pain is physically generated from specific nerves inside the neck joints; 3) Others argue it’s a combination of psychological factors and care should focus on preventing sufferers from becoming chronic patients.
Many studies report that chiropractic offers fast, cost-effective benefits for whiplash-injured patients with faster return to work times and higher levels of patient satisfaction.
We realize you have a choice in whom you consider for your health care provision and we sincerely appreciate your trust in choosing our service for those needs. If you, a friend, or family member requires care for Whiplash, we would be honored to render our services.