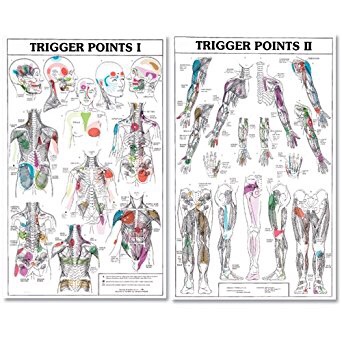
Your thoracic spine is made up of 12 individual vertebrae stacked on top of each other. To allow for flexibility and movement, there is a cushion or “disc” in between each level. As we age, these discs can wear and become thinner over time. This leads to additional changes, including bone spurs and narrowing of the opening where your nerves exit your spine. This process is called “thoracic spondylosis”, or simply, “arthritis”.
How quickly you develop back arthritis is largely a trait you inherited from your parents. Other factors may play a role, including a history of trauma, smoking, operating motorized vehicles, being overweight and/ or performing repetitive movements (i.e. lifting, twisting, bending or sitting). Men seem to be affected slightly more often than women.
Symptoms often begin as back pain that gradually worsens over time. Stiffness may be present upon arising in the morning. Pain is relieved by rest or light activity and aggravated by strenuous work. Sometimes your nerves can become “pinched” in narrowed openings where they exit your spine. This can cause pain, numbness, or tingling radiating around your trunk along the path of the irritated nerve. Be sure to tell your doctor if you notice any weakness or if you have a rash (running along your rib), fever, abdominal pain, change in bowel or bladder function, or pain in your groin crease.
Arthritic changes can be seen on x-rays, but interestingly, the amount of wearing does not seem to correlate directly with the severity of your symptoms. People with the same degree of arthritis may have symptoms ranging from none to severe. Most researchers believe that the symptoms of osteoarthritis are not the direct result of the disease, but rather, from the conditions that preceded the disease and those that develop after it, like joint restrictions and muscle tightness. Fortunately, those conditions are treatable and our office has a variety of tools to help relieve your pain.
In general, you should avoid repeated lifting and twisting and take frequent breaks from prolonged sitting, especially in motorized vehicles. Avoid any position that causes an increase in radiating pain. Light exercise, like walking, stationary cycling, water aerobics, and yoga may be helpful. Smokers should find a program to help them quit and overweight patients will benefit from a diet and exercise program.

 This process is called “lumbar spondylosis”, or simply, “arthritis”. This problem most commonly involves the vertebra at the very base of your spine, which bear the highest loads.
This process is called “lumbar spondylosis”, or simply, “arthritis”. This problem most commonly involves the vertebra at the very base of your spine, which bear the highest loads.
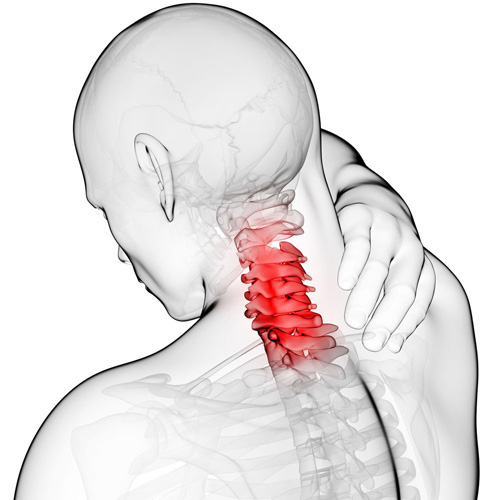


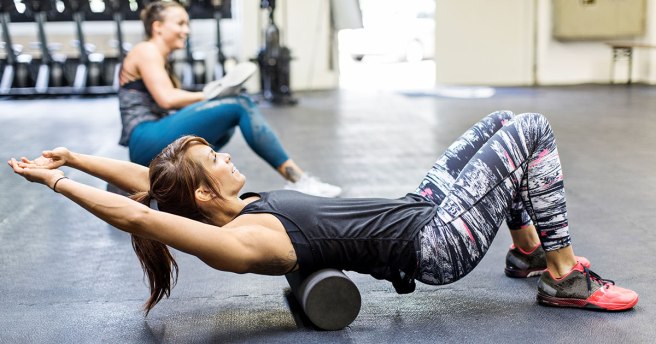

 Your low back relies on discs and other ligaments for support. “Discogenic Low Back Pain” develops when these tissues are placed under excessive stress, much like a rope that frays when it is stretched beyond its normal capacity. Most commonly, disc pain is not the result of any single event, but rather from repeated overloading. Your lumbar discs generally manage small isolated stressors quite well, but repetitive challenges lead to injury in much the same way that constantly bending a piece of copper wire will cause it to break. Examples of these stressors include: bad postures, sedentary lifestyles, poor fitting workstations, repetitive movements, improper lifting, or being overweight.
Your low back relies on discs and other ligaments for support. “Discogenic Low Back Pain” develops when these tissues are placed under excessive stress, much like a rope that frays when it is stretched beyond its normal capacity. Most commonly, disc pain is not the result of any single event, but rather from repeated overloading. Your lumbar discs generally manage small isolated stressors quite well, but repetitive challenges lead to injury in much the same way that constantly bending a piece of copper wire will cause it to break. Examples of these stressors include: bad postures, sedentary lifestyles, poor fitting workstations, repetitive movements, improper lifting, or being overweight.