Since 2005, Bryan has been dedicated to helping all people with chronic and acute pain caused by soft-tissue damage.
His training and experience make him uniquely qualified to treat a wide variety of pain and dysfunction and to give instruction on prevention and self-care.
Bryan is the only Massage Therapist in Manitoba — and one of the few in Canada — to be certified by the Certification Board for Myofascial Trigger Point Therapists (CBMTPT).
Bryan holds a degree as an Advanced Remedial Massage Therapist (ARMT) from the Massage Therapy College of Manitoba. Course work at MTCM includes
• over 2,000 hours of practice, as well as
• intensive course work,
• a supervised clinical practicum, and
• community outreach placements.MTCM has a credit transfer affiliation with the University of Winnipeg, ensuring that its courses are held to the highest level. When Bryan studied at MTCM, the college was the only massage therapy college in western Canada accredited by the Commission on Massage Therapy Accreditation. Today, the college is a member of the Canadian Council of Massage Therapy Schools.
Bryan is a member in good standing of the Natural Health Practitioners of Canada.
Bryan also has a background in Anatomy, Exercise Physiology, and Sport Sciences from the University of Manitoba, and he has worked as a personal trainer and fitness leader.
He is an avid natural bodybuilder and fitness enthusiast, and has a blue belt in Brazilian jiu-jitsu.
stress
Trigger points in the Quadratus Lumborum muscle.
The quadratus lumborum muscle is a commonly overlooked source of low back pain and is often responsible for “pseudo disc syndrome”. This muscle originates on the inferior border of the 12th rib and lumbar transverse processes. It inserts on the iliac crest and iliolumbar ligament. The q.l.’s main actions are extension and lateral flexion of the spine. It also acts as a stabilizer of the lumbar spine. Trigger points in this muscle refer pain into the sacroiliac joint and the lower buttock. Pain can also spread anteriorly along the crest of the ilium into the lower abdomen and groin and to the greater trochanter. 
Trigger points in the temporalis muscle
The temporalis muscle is located in the temple area of the skull. It originates on the temporal lines on the parietal bone of the skull, and inserts on the coronoid process of the mandible. It’s main action is to close the jaw. The posterior and middle fibres bilaterally retrude the mandible. Acting individually, this muscle will deviate the mandible to the same side. Trigger points in this muscle refer into the teeth causing hypersensitivity, and into and above the eye and temple, causing headaches.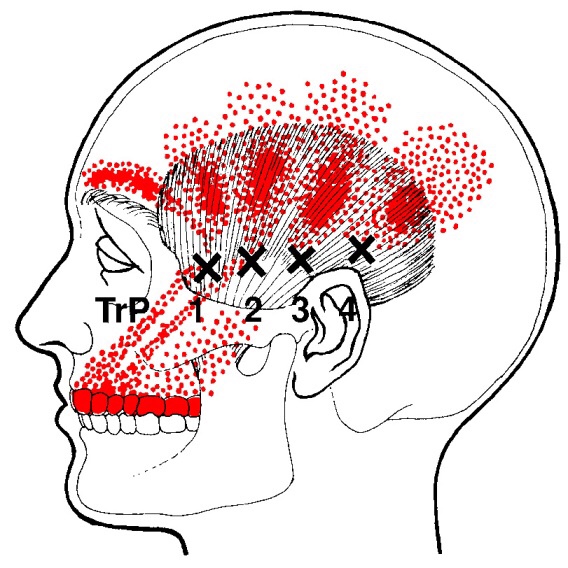
What is Tarsal Tunnel Syndrome?
The tarsal tunnel is the space behind the bump on the inside of your ankle. The tibial nerve lives in this tunnel along with some tendons. Tarsal tunnel syndrome means that the tibial nerve is being irritated within the tunnel. This results in pain, numbness or tingling into your heel and the arch of your foot.
The tibial nerve may be irritated by compression (from trauma , arthritic spurs, or swelling of other tissues within the tunnel), or more commonly by constant stretch (from flat feet). Research has shown that tarsal tunnel pressure increases almost 30 fold in people with flat feet.
 Tarsal tunnel is slightly more common in women, and high heels are suspect. The condition often affects both feet. Conditions like diabetes and thyroid disorders may aggravate nerve problems like tarsal tunnel. Plantar fasciitis commonly accompanies tarsal tunnel syndrome.
Tarsal tunnel is slightly more common in women, and high heels are suspect. The condition often affects both feet. Conditions like diabetes and thyroid disorders may aggravate nerve problems like tarsal tunnel. Plantar fasciitis commonly accompanies tarsal tunnel syndrome.
The discomfort is often described as “burning”. Symptoms may increase with long periods of standing, running or exercise. Almost half of patients report increased symptoms at night.
Your doctor will make the diagnosis of tarsal tunnel syndrome based on your history and an exam. Your doctor may take an x-ray to rule out other problems like arthritic spurs or a stress fracture. In severe cases, more sophisticated nerve testing may be necessary.
The first goal of treatment is to allow you to return to pain-free activity as soon as possible. The second goal is to correct the mechanical problem that allowed this condition to begin with.
Trigger points in the lateral pterygoid
The lateral pterygoid muscle plays an important role in prober jaw function. It originates on the greater wing of the sphenoid bone and the lateral pterygoid plate, and inserts on the condyloid process of the mandible. It’s action is to pull the head of the mandibular condyle out of the mandibular fossa while opening the jaw. When trigger points develop they refer pain into the temporal mandibular joint and maxillary sinus. This referral is commonly mistaken for TM arthritis. In addition to the referral pain, trigger points in this muscle can also effect proper movement of the jaw.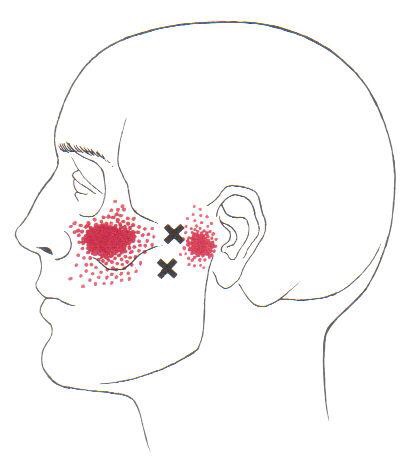

What is Fibromyalgia?
Fibromyalgia, although often misdiagnosed and misunderstood, is the second most common musculoskeletal disorder behind osteoarthritis. The condition affects nearly 12 million Americans and is ten times more common in women.
The diagnosis of fibromyalgia is made when a certain set of symptoms has been present for at least three months. The most common symptoms include wide-spread muscle and joint pain, achiness or soreness- especially in the neck, shoulders, back, and hips. Your muscles may constantly feel overworked and tired. Fibromyalgia patients often exhibit a set of predictable “tender points” spread throughout the body. Some patients have trouble sleeping and feel as though they are in a “brain fog” most of the day. This can lead to fatigue or mood changes, like anxiety and depression.

Stress is a known contributor to fibromyalgia, and patients should seek ways to de-stress, including yoga or meditation. Fibromyalgia patients should minimize their caffeine intake, as this is a known stimulant for nervousness, anxiety, and insomnia. Breathing exercises are sometimes helpful.
Although your sleep may be restless, you should try to establish a bedtime routine that gives your body the best chance for recovery. Try to avoid late night electronics, like the television or computer. Keep your bedroom dark, quiet, cool, and distraction-free. Be sure to take time for yourself each day for relaxation or to do something you enjoy. Combat “brain fog” by carrying a notebook or a phone to make notes for important things. Some patients report decreased muscle tightness by applying moist heat or a taking warm bath. The American Pain Society recommends conservative treatment, including chiropractic, along with moderate aerobic exercise.
What Is Upper Crossed Syndrome?
Your posture plays an important role in your overall health. Poor posture leads to chronic strain and discomfort. “Upper crossed syndrome” describes poor posture that results from excessive tightness in your shoulders and chest with weakness in your neck and mid-back. This combination forces your shoulders to roll inward and your head to project forward.

To help understand how upper crossed syndrome causes trouble, think of your spine as a telephone pole and your head as a bowling ball that sits on top. When the bowling ball is positioned directly over the top of the upright post, very little effort is required to keep it in place. If you tip the post forward and the ball begins to roll over the edge of the post, significantly more effort would be required from the muscles trying to hold it there. This effort results in chronic strain of the muscles of your neck and upper back.
The chronic strain is uncomfortable and may also lead to neck pain, upper back pain, headaches, TMJ pain, and ultimately- arthritis. This postural problem is exceptionally common in computer workstation users. Correction of this problem is accomplished by stretching the tight muscles, strengthening weak muscles, and modifying your workstation.
Is there an actual cure all?
No; but exercise seems to be as close as we will ever get!
Some of you may have heard about how a modified form of boxing is helping patients with Parkinson’s disease (PD). If you haven’t, it’s been observed that people with Parkinson’s disease (PD) who engage in this boxing-like exercise routine can enhance their quality of life and even build impressive gains in posture, strength, flexibility, and speed. Proponents of the program report that regardless the degree of severity of PD, participants have a happier, healthier, and higher quality of life.
But must it be boxing? Maybe not. A report presented at the International Congress of Parkinson’s Disease and Movement Disorders in San Diego in June 2015 found that patients with Parkinson’s disease who began regular exercise early into the PD process had a much slower decline in their quality of life when compared with those who started exercising later. The researchers found just 2.5 hours per week of exercise is needed to improve quality of life scores. According to the report, it didn’t matter what exercise the participants did — simply getting up and moving for a total of 2.5 hours/week was reportedly enough (that’s only 20-25 minutes / day)!
Looking beyond Parkinson’s, other chronic conditions also benefit from adding exercise into a person’s lifestyle. Studies show that regular exercise as simple as walking helps reduce one’s risk for memory loss, and it slows down functional decline in the elderly. Incorporating aerobic exercise into one’s lifestyle can also improve reaction time in people at ALL AGES. Exercise has also been shown to improve both physical and emotional well-being in those afflicted with Alzheimer’s disease with as little as 60 minutes/week of moderate exercise! Patients with multiple sclerosis (MS) have also reported less stiffness and less muscle wasting when using exercise machines, aquatic exercise, and/or walking.
Research has shown just 30 minutes of brisk exercise three times a week can help reduce depressive symptoms in patients with mild-to-moderate depression. In a study involving teenagers, those who engaged in sports reported a greater level of well-being than their sedentary peers, and the more vigorous the exercise, the better their emotion health! In kids 8-12 years old, physical inactivity is strongly linked to depression.
Even anxiety, stress, and depression associated with menopause are less severe in those who exercise! So LET’S ALL GET OUT THERE AND EXERCISE!!!
Work Station Ergonomics Advice
When dealing with Upper Crossed Syndrome the ergonomics of your workstation should be at the from of mind. Some workstation ergonomics advice is as follows:
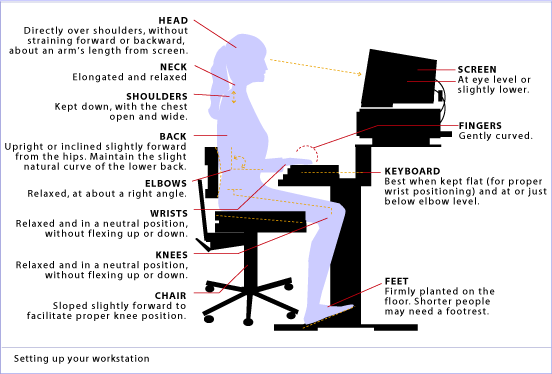
Upper Crossed Syndrome/Desk Neck

Your posture plays an important role in your overall health. Poor posture leads to chronic strain and discomfort. “Upper crossed syndrome” describes poor posture that results from excessive tightness in your shoulders and chest with weakness in your neck and mid-back. This combination forces your shoulders to roll inward and your head to project forward.
To help understand how upper crossed syndrome causes trouble, think of your spine as a telephone pole and your head as a bowling ball that sits on top. When the bowling ball is positioned directly over the top of the upright post, very little effort is required to keep it in place. If you tip the post forward and the ball begins to roll over the edge of the post, significantly more effort would be required from the muscles trying to hold it there. This effort results in chronic strain of the muscles of your neck and upper back.
The chronic strain is uncomfortable and may also lead to neck pain, upper back pain, headaches, TMJ pain, and ultimately- arthritis. This postural problem is exceptionally common in computer workstation users.
Correction of this problem is accomplished by stretching the tight muscles, strengthening weak muscles, and modifying your workstation. Treatment is aimed at reducing and eliminating symptoms through the use of Chiropractic adjustments, soft tissue release, acupuncture and trigger point therapy.

