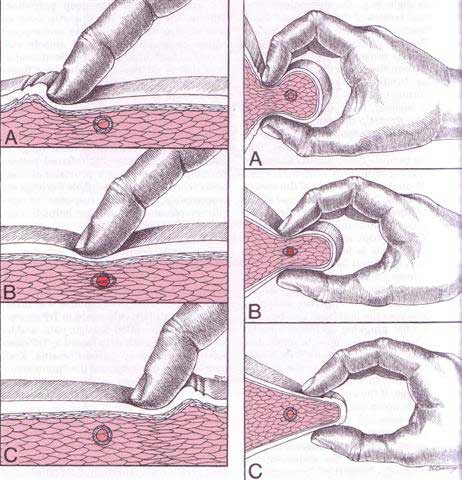
Carpal Tunnel Syndrome (CTS) is a VERY common condition where the median nerve is compressed or squeezed as it passes through the wrist. One reason that it’s so common is because MANY daily activities require fast, repetitive use of the fingers, hands, and arms, and the friction of the rapidly moving muscle tendons inside the tunnel results in swelling and compression of the nerve. So, can CTS really be prevented?
There are many factors associated with CTS, and some risks can be prevented. For example, some conditions like diabetes, rheumatoid arthritis, and IBS increase the risk of CTS. Therefore, it would be safe to assume those who better manage such conditions would have a lower risk for developing CTS.
Due to the many factors associated with CTS, there is no “one size fits all” when it comes to treatment and prevention of CTS. With that said, here are some VERY effective methods:
1) Ergonomic workstation modifications: Altering the work space (monitor height, keyboard/mouse style, different chair, chair/desk height, etc.) to reduce the number and speed of movements needed to perform commons work tasks.
2) Rest periods: Insert “micro-breaks” into a busy task. Combine breaks with stretching exercises of the wrist/hand/fingers and vary job tasks between fast and slow repetitive types.
3) Exercise: Shake the fingers and hands, lean back in a chair with the arms/shoulders stretched back (“Brugger’s Exercise”), move the neck (chin tucks, rotations, etc.), bend the hand/wrist backwards on a wall or the desk’s edge, self-massage and deep tissue release of the forearm and hand muscles. Do regular aerobic exercise (walking, swimming, biking, etc.) several times each week.
4) Posture: Sit up straight, elbows about 90° on height-adjustable arm rests or comfortably at the sides, forearms parallel to the floor; knees level or slightly lower than the hips, feet flat on the floor or on a footrest or box, if needed. Place typing materials at eye level / avoid prolonged head/neck rotation. Use a wrist rest for the keyboard and mouse, and use a headset when on the phone.
5) Reduce hand tool forces: Choose a tool that allows the wrist to remain neutral. Avoid side to side and flexion/extension wrist positions—especially if they’re prolonged! Tool handles should NOT dig into the palm of the hand or the wrist, and should not have sharp edges. A textured handle can improve grip. Minimize vibration from power tools. Wear shock absorbing gloves. Avoid cold work environments and cold tools.
6) Diet: Cut down on caffeine and smoking. Avoid obesity—a known risk factor of CTS! Consider an anti-inflammatory diet (Paleo, Mediterranean).
7) Splints: A wrist cock-up splint at night prevents prolonged faulty positions and REALLY helps!
This is a partial list of preventative measures that can REALLY help. Doctors of chiropractic treat the WHOLE person and can teach you the right exercises, ways to modify your diet, offer manual therapies and modalities, and help guide you in your self-management of CTS, as this can be a lifelong affliction. A multi-modal treatment approach generally works best!