Pain
Fibromyalgia and Sleep
Is there a connection between fibromyalgia (FM) and sleep disturbance? Let’s take a look!
FM is a condition that causes widespread pain and stiffness in muscles and joints. Patients with FM often experience chronic daytime fatigue and some type of sleep problems like getting to sleep, staying asleep, and/or feeling restored in the morning upon waking. The National Institutes of Health estimates between 80-90% of those diagnosed with FM are middle-aged women, although it can affect men and happen at any age. As little as 10-20 years ago, it was hard to find a doctor who “believed” in FM, and it was common for the patient to be told that their pain “was all in their head.” FM has now been studied to the point that we know it is a real condition, and it affects between 2-6% of the general population around the world.
It is well established that sleep disturbance frequently occurs after surgery, which usually normalizes as time passes. One study used a group of healthy women who were deprived of sleep (particularly slow wave sleep) for three days to see if there was a link between sleep disturbance and pain. Results confirmed that the women experienced a decrease in pain tolerance and increased levels of discomfort and fatigue after three days—the same symptoms found among FM sufferers!
Fibromyalgia may have NO known cause, or it can be triggered by other conditions such as repetitive stress injuries, car crash injuries, and other forms of trauma. FM also appears to run in families though it’s still NOT clear if this is a true genetic link or caused by shared environmental factors. Some feel FM is a rheumatoid condition, and though FM is NOT a true form of arthritis, it has been found that people with arthritis are more likely to have FM.
FM sufferers frequently suffer from conditions such as irritable bowel syndrome, chronic fatigue syndrome, migraine headaches, arthritis, lupus, and major depressive disorders. Approximately 20% of FM patients have depression and/or anxiety disorders, and a link between chronic pain and depression exists and seems to play a role in people’s perception of pain.
Because conditions such as sleep apnea can result in symptoms similar to FM, it’s recommended that patients suspected of FM keep a sleep/sleepiness diary in order to rule out sleep apnea as a cause for their condition.
There are many “tips” for improving sleep quality, which we will dive into next month, as these may prove VERY HELPFUL in the management of FM!
If you, a friend or family member requires care for Fibromyalgia, we sincerely appreciate the trust and confidence shown by choosing our services!
Teens & Headaches? What?

In 2016, researchers at Curtin University in Perth examined the seated posture and health data of 1,108 17-year olds in an effort to determine if any particular posture increased the risk of headaches/neck pain among late adolescents.
Among four posture subgroups—upright, intermediate, slumped thorax, and forward head—the researchers observed the following: participants who were slumped in their thoracic spine (mid-back region) and had their head forward when they sat were at higher odds of having mild, moderate, or severe depression; participants classified as having a more upright posture exercised more frequently, females were more likely to sit more upright than males; those who were overweight were more likely to sit with a forward neck posture; and taller people were more likely to sit upright.
While they found biopsychosocial factors like exercise frequency, depression, and body mass index (BMI) ARE associated with headaches and neck pain, their data did not suggest any one particular posture increased the risk of neck pain or headaches more than any other posture among the teenagers involved in the study.
This is noteworthy as studies with adults do indicate the risk for neck pain and headaches is greater in individuals with poor neck posture. In particular, postures such as forward head carriage, pinching a phone between the ear and shoulder, and prolonged neck/head rotation outside of neutral can all increase the risk of cervical disorders. This suggests that in younger bodies, the cause of neck pain and headaches may be multifactoral and not limited to just poor posture and that treatment must address all issues that may increase one’s risk for neck pain/headaches in order to reach a desired outcome.
The good news is that chiropractic has long embraced the biopsychosocial model of healthcare, looking at ALL factors that affect back and neck pain and quality of life. Through patient education, spinal manipulation, mobilization, exercise training, the use of modalities, and more, chiropractors can greatly help those struggling with neck pain and headaches!
Non-surgical Options
Diet & Exercise Tip Of The Month

Research has shown that working out first thing in the morning will rev up your metabolism for the rest of the day. If you’re short on time in the mornings, opt for a quick, but high-intensity workout of the basics, such as jumping jacks, push-ups, and squats.
CBC with some exercise tips!

http://www.cbc.ca/beta/news/canada/calgary/fall-fitness-calgary-tips-1.4306014
The CBC actually earning our tax dollars with a solid article on fitness!
Fibromyalgia Diet?
Folks suffering with fibromyalgia (FM) commonly complain that certain foods can make their symptoms worse. How common is this? One study reported 42% of FM patients found that certain foods worsened their symptoms!
Because FM affects each person differently, there is no ONE FM diet or, “…one size fits all” when it comes to eating “right” for FM. Patients with FM usually find out by trial and error which foods work vs. those that consistently don’t. However, remembering which foods do what can be a challenge so FIRST, make a three column FOOD LOG with the following headings: BETTER, NO CHANGE, WORSE. This will allow you to QUICKLY review the list as a memory refresher.
According to Dr. Ginevra Liptan, medical director of the Frida Center for Fibromyalgia (Portland, OR) and author of Figuring Out Fibromyalgia: Current Science and the Most Effective Treatments, there are some common trends she’s observed through treating FM patients. Here are some of her recommendations:
PAY ATTENTION TO HOW FOOD MAKES YOU FEEL: It is quite common to have “sensitivities” to certain foods, but this is highly variable from person to person. Examples of problematic foods/ingredients include: MSG (commonly used in Chinese food), other preservatives, eggs, gluten, and dairy. Dr. Liptan HIGHLY recommends the food journal approach! She also recommends including a note about the type of symptoms noticed with each “WORSE” food, as symptoms can vary significantly.
ELIMINATE CERTAIN FOODS: If you suspect a certain food may be problematic, try an elimination challenge diet. That means STOP eating that food for six to eight weeks and then ADD it back into your diet and see how you feel. Remember, FM sufferers frequently have irritable bowel syndrome, also known as IBS, and this approach can be REALLY HELPFUL! Food allergies may be part of the problem, and your doctor may refer you for a consult with an allergist and/or a dietician. They will also discuss the “anti-inflammatory diet” with you.
EAT HEALTHY: In general, your diet should emphasize fruits and vegetables and lean protein. Pre-prepare food so you have something “healthy” to reach for rather than a less healthy snack when you’re hungry and tired. Consider “pre-washed” and pre-cut up vegetables; try quinoa rather than pasta. Consume anti-fatigue foods and eat multiple small meals daily vs. one to two large meals. Protein snacks (like a hardboiled egg or oatmeal – GLUTEN FREE) help a lot! Eat breakfast and include protein. Also, GET ENOUGH SLEEP (at least seven to eight hours and be consistent)!
SUPPLEMENTS: Consider a good general multi-vitamin, calcium and magnesium, omega-3 fatty acids, vitamin D3, and Co-Enzyme Q10. There are others, but this represents a great place to start. Remember to check any medication you may be taking with these/any suggestions before taking supplements!
If you, a friend or family member requires care for Fibromyalgia, we sincerely appreciate the trust and confidence shown by choosing our services!
I love this video
There is a lot to be learnt from this video. Dr. Mike Evans does a great job of explaining why we need to KEEP MOVING during and after an episode of low back pain. Check it out!
Exercise of the Month!
One of our favourites in the office; Thoracic Rotation.
An easy exercise for your upper and mid-back. No equipment required! – (Post link to article and video on your blog or post video directly on your social media account.)”
- Begin on your hands and knees and shift back so that your buttock is on your heels.
- Place one hand behind your neck with your elbow pointing downward.
- Rotate your trunk to move your elbow towards your opposite knee.
- Rotate back, raising your elbow toward the ceiling.
- Repeat three sets of 10 repetitions on each side twice per day or as directed.
What is Whiplash?
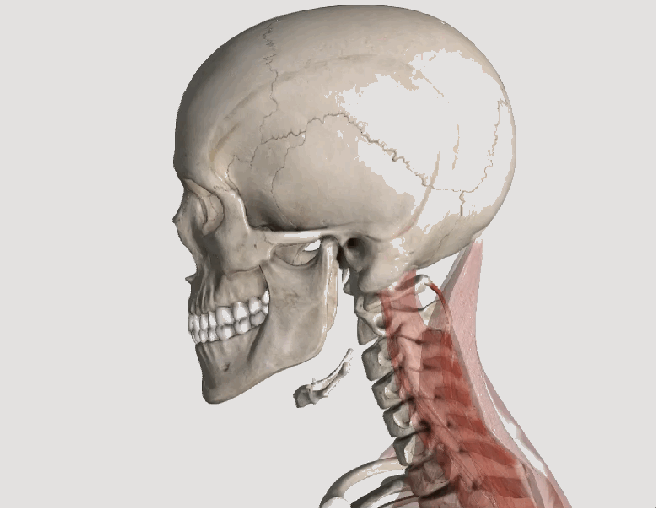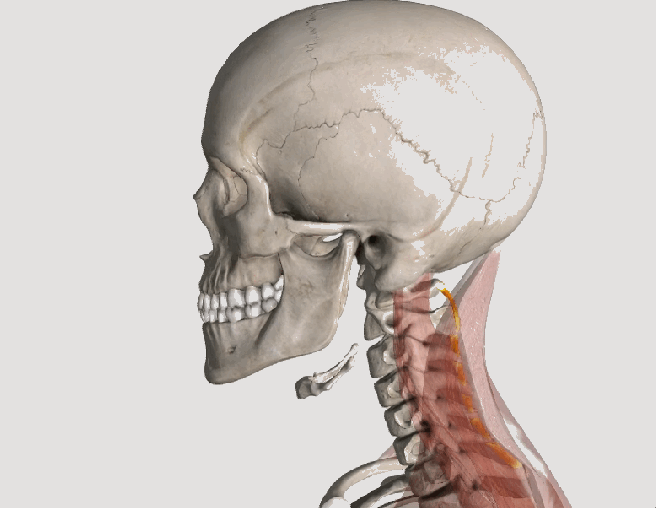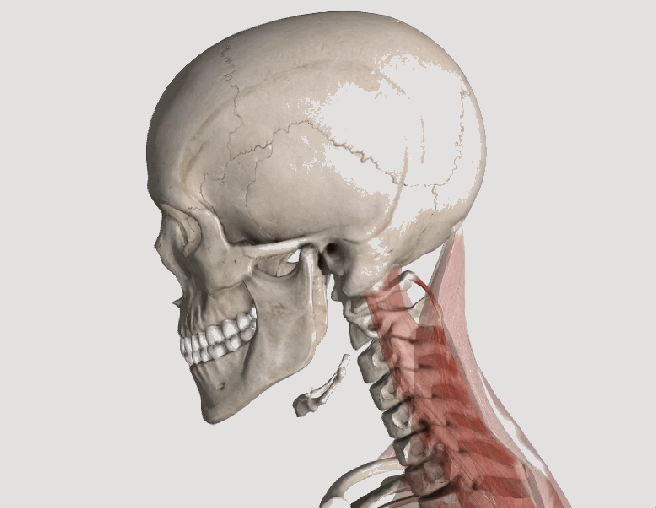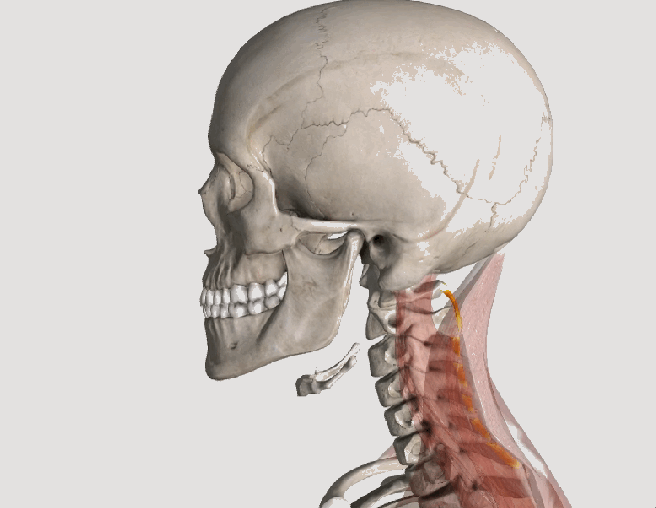
Whiplash is an injury to the soft-tissues of the neck often referred to as a sprain or strain. Because there are a unique set of symptoms associated with whiplash, doctors and researchers commonly use the term “whiplash associated disorders” or WAD to describe the condition.
WAD commonly occurs as a result of a car crash, but it can also result from a slip and fall, sports injury, a personal injury (such as an assault), and other traumatic causes. The tissues commonly involved include muscle tendons (“strain”), ligaments and joint capsules (“sprains”), disk injuries (tears, herniation), as well as brain injury or concussion—even without hitting the head!
Symptoms vary widely but often include neck pain, stiffness, tender muscles and connective tissue (myofascial pain), headache, dizziness, sensations such as burning, prickly, tingling, numbness, muscle weakness, and referred pain to the shoulder blade, mid-back, arm, head, or face. If concussion occurs, additional symptoms include cognitive problems, concentration loss, poor memory, anxiety/depression, nervousness/irritability, sleep disturbance, fatigue, and more!
Whiplash associated disorders can be broken down into three categories: WAD I includes symptoms without any significant examination findings; WAD II includes loss of cervical range of motion and evidence of soft-tissue damage; and WAD III includes WAD II elements with neurological loss—altered motor and/or sensory functions. There is a WAD IV which includes fracture, but this is less common and often excluded.
Treatment for WAD includes everything from doing nothing to intensive management from multiple disciplines—chiropractic, primary care, physical therapy, clinical psychology, pain management, and specialty services such as neurology, orthopedics, and more. The goal of treatment is to restore normal function and activity participation, as well as symptom management.
The prognosis of WAD is generally good as many will recover without residual problems within days to weeks, with most people recovering around three months after the injury. Unfortunately, some are not so lucky and have continued neck pain, stiffness, headache, and some develop post-concussive syndrome. The latter can affect cognition, memory, vision, and other brain functions. Generally speaking, the higher the WAD category, the worse the prognosis, although each case MUST be managed by its own unique characteristics. If the injury includes neurological loss (muscle strength and/or sensory dysfunction like numbness, tingling, burning, pressure), the prognosis is often worse.
Chiropractic care for the WAD patient can include manipulation, mobilization, and home-based exercises, as well as the use of anti-inflammatory herbs (ginger, turmeric, proteolysis enzymes (bromelain, papain), devil’s claw, boswellia extract, rutin, bioflavonoid, vitamin D, coenzyme Q10, etc.) and dietary modifications aimed at reducing inflammation and promoting healing.
* 83% of those patients involved in an MVA will suffer whiplash injury and 50% will be symptomatic at 1 year.
* 90% of patients with neurologic signs at onset may be symptomatic at 1 year.
* 25- 80% of patients who suffer a whiplash injury will experience late-onset dizziness
* Clinicians should be observant for radiographic signs of instability, including interspinous widening, vertebral subluxation, vertebral compression fracture, and loss of cervical lordosis.
* Horizontal displacement of greater than 3.5 mm or angular displacement of more than 11 degrees on flexion/extension views suggests instability.


