When dealing with Upper Crossed Syndrome the ergonomics of your workstation should be at the from of mind. Some workstation ergonomics advice is as follows:
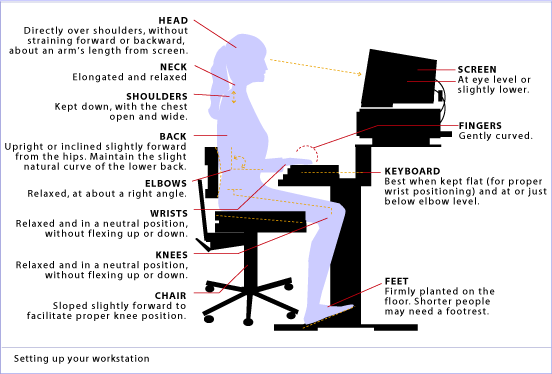
When dealing with Upper Crossed Syndrome the ergonomics of your workstation should be at the from of mind. Some workstation ergonomics advice is as follows:

Your low back consists of 5 individual vertebrae stacked on top of each other. Flexible cushions called “discs” live between each set of vertebrae. A disc is made up of two basic components. The inner disc, called the “nucleus”, is like a ball of jelly about the size of a marble. This jelly is held in place by the outer part of the disc called the “annulus”, which is a tough ligament that wraps around the inner nucleus much like a ribbon wrapping around your finger.

Your low back relies on discs and other ligaments for support. “Discogenic Low Back Pain” develops when these tissues are placed under excessive stress, much like a rope that frays when it is stretched beyond its normal capacity. Most commonly, disc pain is not the result of any single event, but rather from repeated overloading. Your lumbar discs generally manage small isolated stressors quite well, but repetitive challenges lead to injury in much the same way that constantly bending a piece of copper wire will cause it to break. Examples of these stressors include: bad postures, sedentary lifestyles, poor fitting workstations, repetitive movements, improper lifting, or being overweight.
Approximately one third of adults will experience pain from a lumbar disc at some point in their lifetime. The condition is more common in men. Most lumbar disc problems occur at one of the two lowest discs- L5 or L4. Smokers and people who are generally inactive have a higher risk of lumbar disc problems. Certain occupations may place you at a greater risk, especially if you spend extended periods of time sitting or driving. People who are tall or overweight have increased risk of disc problems.
Symptoms from disc pain may begin abruptly but more commonly develop gradually. Symptoms may range from dull discomfort to surprisingly debilitating pain that becomes sharper when you move. Rest may relieve your symptoms but often leads to stiffness. The pain is generally centered in your lower back but can spread towards your hips or thighs. Be sure to tell your doctor if your pain extends beyond your knee, or if you have weakness in your lower extremities or a fever.
Repeated injuries cause your normal healthy elastic tissue to be replaced with less elastic “scar tissue.” Over time, discs may dehydrate and thin. This process can lead to ongoing pain and even arthritis. Patients who elect to forego treatment and “just deal with it” develop chronic low back pain more than 60% of the time. Seeking early and appropriate treatment like the type provided in our office is critical.
Depending on the severity of your injury, you may need to limit your activity for a while, especially bending, twisting, and lifting, or movements that cause pain. Bed rest is not in your best interest. You should remain active and return to normal activities as your symptoms allow. Light aerobic exercise (i.e. walking, swimming, etc) has been shown to help back pain sufferers. The short-term use of a lumbar support belt may be helpful. Sitting makes your back temporarily more vulnerable to sprains and strains from sudden or unexpected movements. Be sure to take “micro breaks” from workstations for 10 seconds every 20 minutes.
A large number of factors have been identified as causes of trigger point activation. These include acute or chronic overload of muscle tissue, disease, psychological distress, systemic inflammation, homeostatic imbalances, direct trauma, radiculopathy, infections, and lifestyle choices such as smoking. Trigger points form as a local contraction of muscle fibres in a muscle or bundle of muscle fibres. These can pull on ligaments and tendons associated with the muscle which can cause pain to be felt deep inside a joint. It is theorized that trigger points form from excessive release of acetylcholine causing sustained depolarization of muscle fibres. Trigger points present an abnormal biochemical composition with elevated levels of acetylcholine, noradrenaline and serotonin and a lower ph. The contracted fibres in a trigger point constricts blood supply to the area creating an energy crisis in the tissue that results in the production of sensitizing substances that interact with pain receptors producing pain. When trigger points are present in a muscle there is often pain and weakness in the associated structures. These pain patterns follow specific nerve pathways that have been well mapped to allow for accurate diagnosis or the causative pain factor.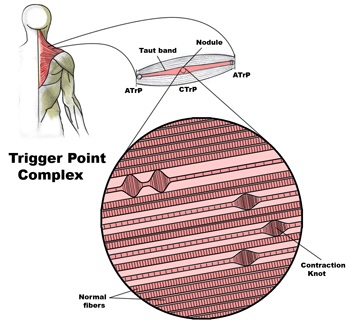
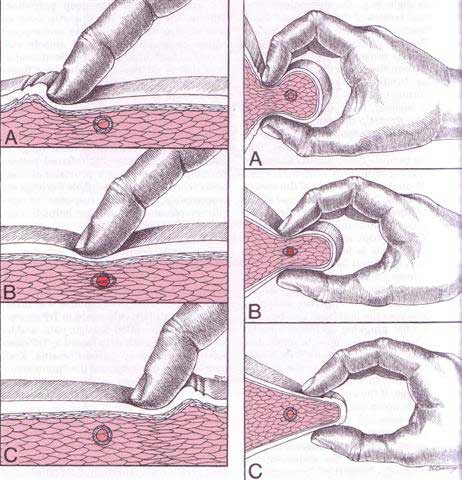
Diagnosis of trigger points typically takes into account symptoms, pain patterns, and manual palpation. When palpating the therapist will feel for a taut band of muscle with a hard nodule within it. Often a local twitch response will be elicited by running a finger perpendicular to the muscle fibres direction. Pressure applied to the trigger point will often reproduce the pain complaint of the patient and the referral pattern of the trigger point. Often there is a heat differential in the local area of the trigger point. 
The Bicep Brachii is perhaps the most recognizable muscle in the body. It’s the muscle that is most often flexed when someone says ” show me your muscles”. It is composed of two heads, the long head and the short head. The short head originates on the coracoid process of the scapula, and the long head on the supraglenoid tubercle. Both heads merge to insert on the radial tuberosity and bicipital aponeurosis into the deep fascia on the medial part of the forearm. The main actions of this muscle are elbow flexion and forearm supination(rotation with the palm of the hand going upward). This muscle also assists shoulder flexion. Trigger points in this muscle mainly refer pain into the shoulder, with spillover into the posterior aspect above the scapula. A less common referral is into the anterior elbow and forearm. 
Dr Janet travel coined the term trigger point in 1942 to describe clinical findings with characteristics of pain related a discrete irritable point in muscle or fascia that was not caused by acute trauma, inflammation, degeneration, neoplasm or infection. The painful point can be palpated as a nodule or tight band in the muscle that can produce a local twitch response when stimulated. Palpation of the trigger point reproduces the pain and symptoms of the patient and the pain radiates in a predictable referral pattern specific to the muscle harbouring the trigger point.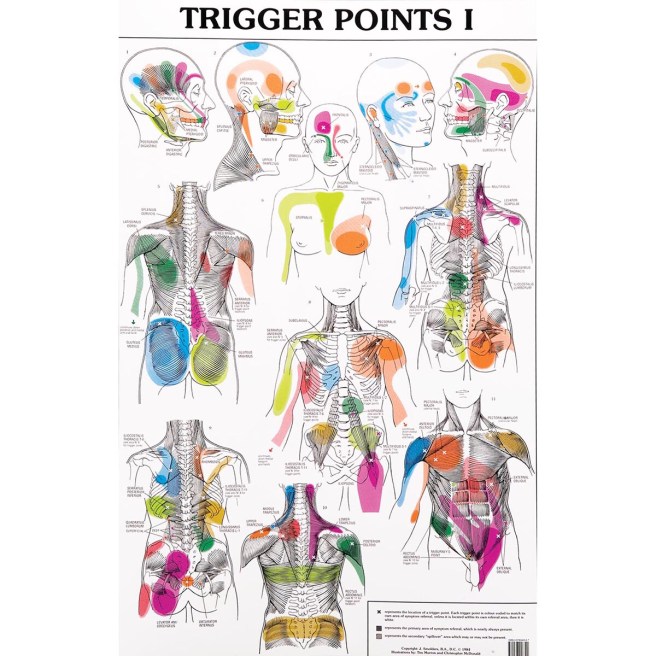
A treatment with Bryan is very user friendly. And, no, you don’t have to remove any clothing. However, bringing a t-shirt and a pair of shorts or sweats is recommended.
The first time you come for a treatment you will be asked to fill out a Client History form. Bryan will go over the information you provide, asking for more detail and discussing the type of pain you are having and its location.
The treatment itself involves locating the Trigger Points in the muscle or soft tissue and applying a deep focused pressure to the Point. This will reproduce the pain and the referral pattern that is characteristic of that pain.
The treatment will be uncomfortable at first, but as the Trigger Points release, the pain will decrease. The pressure will always be adjusted to your tolerance level. If, at any time, you feel too uncomfortable you can ask Bryan to ease off a bit.
Depending on your specific problem, Bryan may also use some stretching and / or range-of-motion techniques, as needed.
After treatment, it is usually recommended that the client apply moist heat to the area treated.
Headaches are REALLY common! In fact, two out of three children will have a headache by the time they are fifteen years old, and more than 90% of adults will experience a headache at some point in their life. It appears safe to say that almost ALL of us will have firsthand knowledge of what a headache is like sooner or later!
Certain types of headaches run in families (due to genetics), and headaches can occur during different stages of life. Some have a consistent pattern, while others do not. To make this even more complicated, it’s not uncommon to have more than one type of headache at the same time!
Headaches can vary in frequency and intensity, as some people can have several headaches in one day that come and go, while others have multiple headaches per month or maybe only one or two a year. Headaches may be continuous and last for days or weeks and may or may not fluctuate in intensity.
For some, lying down in a dark, quiet room is a must. For others, life can continue on like normal. Headaches are a major reason for missed work or school days as well as for doctor visits. The “cost” of headaches is enormous—running into the billions of dollars per year in the United States (US) in both direct costs and productivity losses. Indirect costs such as the potential future costs in children with headaches who miss school and the associated interference with their academic progress are much more difficult to calculate.
There are MANY types of headaches, which are classified into types. With each type, there is a different cause or group of causes. For example, migraine headaches, which affect about 12% of the US population (both children and adults), are vascular in nature—where the blood vessels dilate or enlarge and irritate nerve-sensitive tissues inside the head. This usually results in throbbing, pulsating pain often on one side of the head and can include nausea and/or vomiting. Some migraine sufferers have an “aura” such as a flashing or bright light that occurs within 10-15 minutes prior to the onset while other migraine sufferers do not have an aura.
The tension-type headache is the most common type and as the name implies, is triggered by stress or some type of tension. The intensity ranges between mild and severe, usually on both sides of the head and often begin during adolescence and peak around age 30, affecting women slightly more than men. These can be episodic (come and go, ten to fifteen times a month, lasting 30 min. to several days) or chronic (more than fifteen times a month over a three-month period).
There are many other types of headaches that may be primary or secondary—when caused by an underlying illness or condition. The GOOD news is chiropractic care is often extremely helpful in managing headaches of all varieties and should be included in the healthcare team when management requires a multidisciplinary treatment approach.
The deltoid is the the muscle that is most often thought of as the “shoulder.” It is the diamond shaped muscle that caps the shoulder joint. It originates on the clavicle, the acromion, and the spine of the scapula. It inserts on the deltoid tuberosity of the humerus. As a whole unit the deltoid laterally abducts the humerus at the glenohumeral joint. The anterior portion of the delt forward flexes the arm, as well as horizontally flexing the arm across the chest. Since the deltoid is involved in almost all shoulder movements it is especially prone to trigger points. Points in the anterior deltoid refer into the anterior and lateral shoulder. Trigger points in the posterior deltoid refer pain into the posterior shoulder with spillover down the lateral arm. 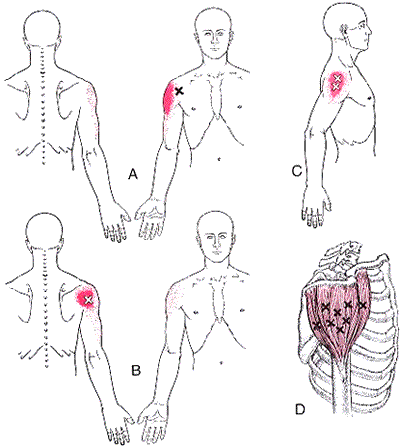
Carpal Tunnel Syndrome (CTS) is a VERY common condition where the median nerve is compressed or squeezed as it passes through the wrist. One reason that it’s so common is because MANY daily activities require fast, repetitive use of the fingers, hands, and arms, and the friction of the rapidly moving muscle tendons inside the tunnel results in swelling and compression of the nerve. So, can CTS really be prevented?
There are many factors associated with CTS, and some risks can be prevented. For example, some conditions like diabetes, rheumatoid arthritis, and IBS increase the risk of CTS. Therefore, it would be safe to assume those who better manage such conditions would have a lower risk for developing CTS.
Due to the many factors associated with CTS, there is no “one size fits all” when it comes to treatment and prevention of CTS. With that said, here are some VERY effective methods:
1) Ergonomic workstation modifications: Altering the work space (monitor height, keyboard/mouse style, different chair, chair/desk height, etc.) to reduce the number and speed of movements needed to perform commons work tasks.
2) Rest periods: Insert “micro-breaks” into a busy task. Combine breaks with stretching exercises of the wrist/hand/fingers and vary job tasks between fast and slow repetitive types.
3) Exercise: Shake the fingers and hands, lean back in a chair with the arms/shoulders stretched back (“Brugger’s Exercise”), move the neck (chin tucks, rotations, etc.), bend the hand/wrist backwards on a wall or the desk’s edge, self-massage and deep tissue release of the forearm and hand muscles. Do regular aerobic exercise (walking, swimming, biking, etc.) several times each week.
4) Posture: Sit up straight, elbows about 90° on height-adjustable arm rests or comfortably at the sides, forearms parallel to the floor; knees level or slightly lower than the hips, feet flat on the floor or on a footrest or box, if needed. Place typing materials at eye level / avoid prolonged head/neck rotation. Use a wrist rest for the keyboard and mouse, and use a headset when on the phone.
5) Reduce hand tool forces: Choose a tool that allows the wrist to remain neutral. Avoid side to side and flexion/extension wrist positions—especially if they’re prolonged! Tool handles should NOT dig into the palm of the hand or the wrist, and should not have sharp edges. A textured handle can improve grip. Minimize vibration from power tools. Wear shock absorbing gloves. Avoid cold work environments and cold tools.
6) Diet: Cut down on caffeine and smoking. Avoid obesity—a known risk factor of CTS! Consider an anti-inflammatory diet (Paleo, Mediterranean).
7) Splints: A wrist cock-up splint at night prevents prolonged faulty positions and REALLY helps!
This is a partial list of preventative measures that can REALLY help. Doctors of chiropractic treat the WHOLE person and can teach you the right exercises, ways to modify your diet, offer manual therapies and modalities, and help guide you in your self-management of CTS, as this can be a lifelong affliction. A multi-modal treatment approach generally works best!