Your low back consists of 5 individual vertebrae stacked on top of each other. Flexible cushions called “discs” live between each set of vertebrae. A disc is made up of two basic components. The inner disc, called the “nucleus”, is like a ball of jelly about the size of a marble. This jelly is held in place by the outer part of the disc called the “annulus”, which is a tough ligament that wraps around the inner nucleus much like a ribbon wrapping around your finger.
 Your low back relies on discs and other ligaments for support. “Discogenic Low Back Pain” develops when these tissues are placed under excessive stress, much like a rope that frays when it is stretched beyond its normal capacity. Most commonly, disc pain is not the result of any single event, but rather from repeated overloading. Your lumbar discs generally manage small isolated stressors quite well, but repetitive challenges lead to injury in much the same way that constantly bending a piece of copper wire will cause it to break. Examples of these stressors include: bad postures, sedentary lifestyles, poor fitting workstations, repetitive movements, improper lifting, or being overweight.
Your low back relies on discs and other ligaments for support. “Discogenic Low Back Pain” develops when these tissues are placed under excessive stress, much like a rope that frays when it is stretched beyond its normal capacity. Most commonly, disc pain is not the result of any single event, but rather from repeated overloading. Your lumbar discs generally manage small isolated stressors quite well, but repetitive challenges lead to injury in much the same way that constantly bending a piece of copper wire will cause it to break. Examples of these stressors include: bad postures, sedentary lifestyles, poor fitting workstations, repetitive movements, improper lifting, or being overweight.
Approximately one third of adults will experience pain from a lumbar disc at some point in their lifetime. The condition is more common in men. Most lumbar disc problems occur at one of the two lowest discs- L5 or L4. Smokers and people who are generally inactive have a higher risk of lumbar disc problems. Certain occupations may place you at a greater risk, especially if you spend extended periods of time sitting or driving. People who are tall or overweight have increased risk of disc problems.
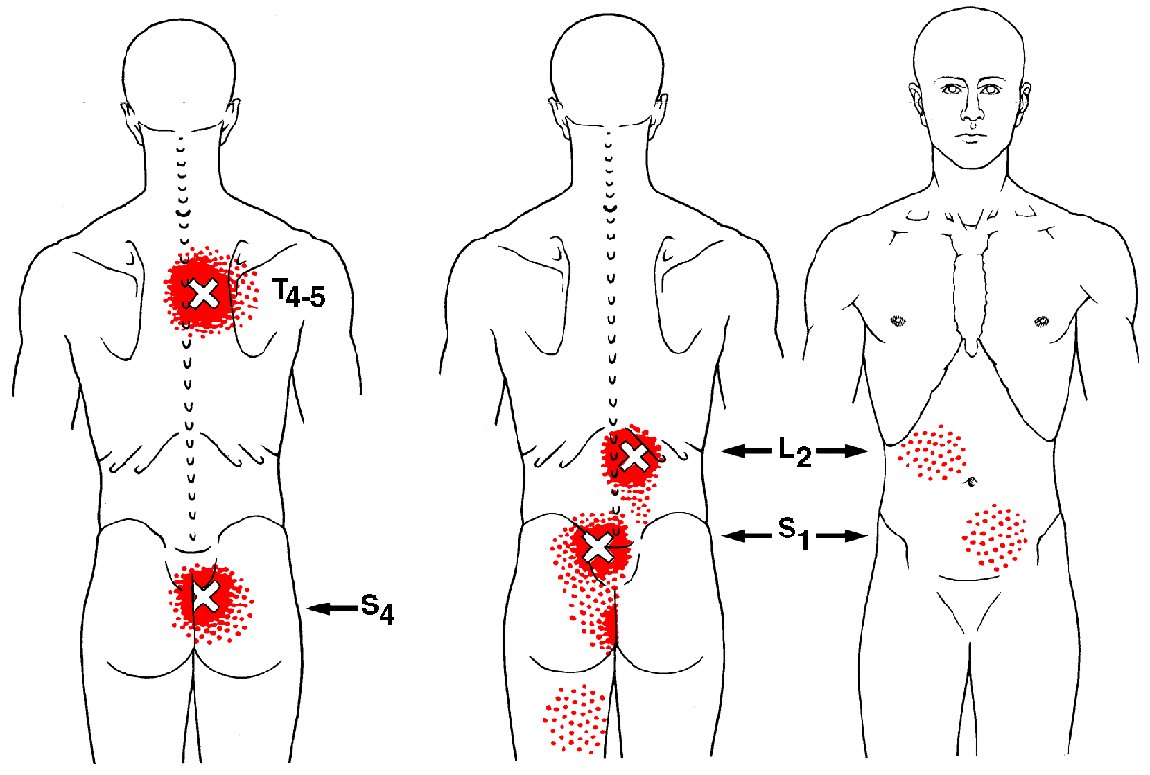
Symptoms from disc pain may begin abruptly but more commonly develop gradually. Symptoms may range from dull discomfort to surprisingly debilitating pain that becomes sharper when you move. Rest may relieve your symptoms but often leads to stiffness. The pain is generally centered in your lower back but can spread towards your hips or thighs. Be sure to tell your doctor if your pain extends beyond your knee, or if you have weakness in your lower extremities or a fever.
Repeated injuries cause your normal healthy elastic tissue to be replaced with less elastic “scar tissue.” Over time, discs may dehydrate and thin. This process can lead to ongoing pain and even arthritis. Patients who elect to forego treatment and “just deal with it” develop chronic low back pain more than 60% of the time. Seeking early and appropriate treatment like the type provided in our office is critical.
Depending on the severity of your injury, you may need to limit your activity for a while, especially bending, twisting, and lifting, or movements that cause pain. Bed rest is not in your best interest. You should remain active and return to normal activities as your symptoms allow. Light aerobic exercise (i.e. walking, swimming, etc) has been shown to help back pain sufferers. The short-term use of a lumbar support belt may be helpful. Sitting makes your back temporarily more vulnerable to sprains and strains from sudden or unexpected movements. Be sure to take “micro breaks” from workstations for 10 seconds every 20 minutes.