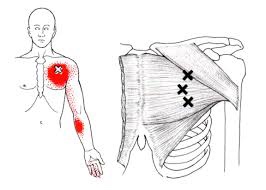
Most of the muscles that flex your wrist are attached to a bony bump on the inside of your elbow called the “medial epicondyle.” Sometimes, through injury or overuse, the site where these muscles originate can become irritated or inflamed. This condition is called “medial epicondylitis”, or “golfer’s elbow.”
Although the condition is named “golfer’s elbow,” over 90% of those affected
are not even athletes, much less golfers. Nonetheless, the condition is more common in certain sports, especially golf, throwing, bowling, football, archery, and weight lifting. Occupations that require heavy gripping or repeated hand movements, like carpentry or typing, can predispose you to this condition. Smokers and people who are obese are more likely to experience this condition.
Medial epicondylitis is the most frequent cause of pain on the “inside” of your elbow but is 3-10 times less likely that its “outside” counterpart- lateral epicondylitis (i.e. “tennis elbow”). Medial epicondylitis is most common between the ages of 40 and 60. The condition strikes the dominant arm in over ¾ of cases. Your symptoms will likely include a dull aching pain over the bump on the inside of your elbow that becomes more intense with use. As the condition progresses, you may notice grip weakness or limitations when shaking hands, grasping objects, and opening jars. Be sure to tell your doctor if you notice numbness or tingling traveling toward your hand.
If left untreated, medial epicondylitis can last indefinitely. Studies show that up to 40% of untreated patients suffer prolonged discomfort, some as long as three years. Fortunately, conservative treatment like the type provided in our office is effective for relieving this condition. Our office may prescribe an elbow “counterforce brace” to help dampen stress to the irritated area. This type of brace should not be used in patients who have numbness or tingling radiating into their fingers. Some patients may benefit from a “wrist splint” that is used at night to allow your tendon to heal in a lengthened position. Using ice or ice massage over your elbow can help limit pain. Your home exercises will play an important role in your recovery.
Initially, you may need to avoid activities that cause an increase in pain, like gripping, lifting, golfing, throwing balls, or swinging a racquet. Be sure to warm up properly and stretch prior to any heavy physical activity. Smokers would benefit from quitting. Overweight patients should consider increasing their aerobic activity to shed excess pounds.
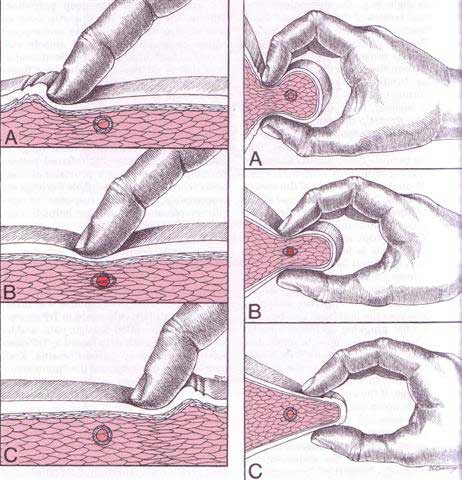

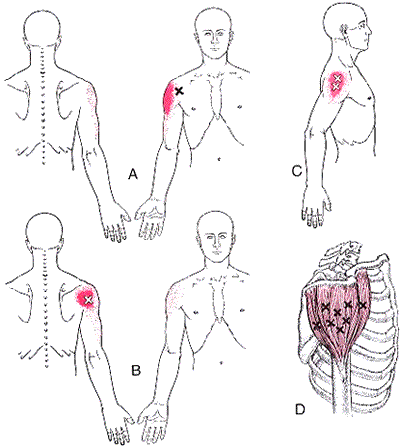


 When you flex your elbow, the ulnar nerve is required to both stretch and slide through your cubital tunnel. If your ulnar nerve is “stuck” in the tunnel and does not glide when you flex your elbow, this leads to traction and irritation of the nerve. This is called “cubital tunnel syndrome.” The nerve may also be irritated from direct compression, like leaning your elbow on the edge of a desk or from arthritic spurs. Cubital tunnel syndrome is the second most common nerve compression problem in the arm, behind carpal tunnel syndrome.
When you flex your elbow, the ulnar nerve is required to both stretch and slide through your cubital tunnel. If your ulnar nerve is “stuck” in the tunnel and does not glide when you flex your elbow, this leads to traction and irritation of the nerve. This is called “cubital tunnel syndrome.” The nerve may also be irritated from direct compression, like leaning your elbow on the edge of a desk or from arthritic spurs. Cubital tunnel syndrome is the second most common nerve compression problem in the arm, behind carpal tunnel syndrome.