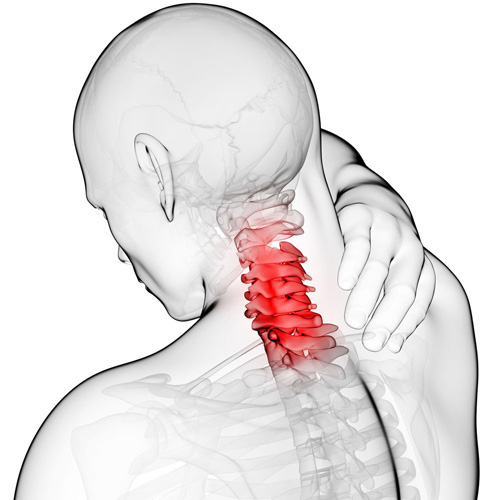
A large number of factors have been identified as causes of trigger point activation. These include acute or chronic overload of muscle tissue, disease, psychological distress, systemic inflammation, homeostatic imbalances, direct trauma, radiculopathy, infections, and lifestyle choices such as smoking. Trigger points form as a local contraction of muscle fibres in a muscle or bundle of muscle fibres. These can pull on ligaments and tendons associated with the muscle which can cause pain to be felt deep inside a joint. It is theorized that trigger points form from excessive release of acetylcholine causing sustained depolarization of muscle fibres. Trigger points present an abnormal biochemical composition with elevated levels of acetylcholine, noradrenaline and serotonin and a lower ph. The contracted fibres in a trigger point constricts blood supply to the area creating an energy crisis in the tissue that results in the production of sensitizing substances that interact with pain receptors producing pain. When trigger points are present in a muscle there is often pain and weakness in the associated structures. These pain patterns follow specific nerve pathways that have been well mapped to allow for accurate diagnosis or the causative pain factor.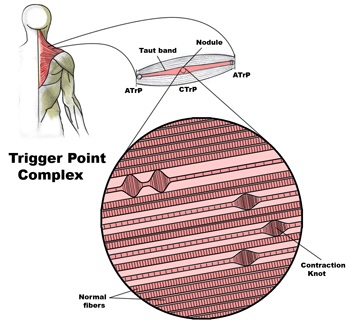
Posture
Upper Crossed Syndrome/Desk Neck

Your posture plays an important role in your overall health. Poor posture leads to chronic strain and discomfort. “Upper crossed syndrome” describes poor posture that results from excessive tightness in your shoulders and chest with weakness in your neck and mid-back. This combination forces your shoulders to roll inward and your head to project forward.
To help understand how upper crossed syndrome causes trouble, think of your spine as a telephone pole and your head as a bowling ball that sits on top. When the bowling ball is positioned directly over the top of the upright post, very little effort is required to keep it in place. If you tip the post forward and the ball begins to roll over the edge of the post, significantly more effort would be required from the muscles trying to hold it there. This effort results in chronic strain of the muscles of your neck and upper back.
The chronic strain is uncomfortable and may also lead to neck pain, upper back pain, headaches, TMJ pain, and ultimately- arthritis. This postural problem is exceptionally common in computer workstation users.
Correction of this problem is accomplished by stretching the tight muscles, strengthening weak muscles, and modifying your workstation. Treatment is aimed at reducing and eliminating symptoms through the use of Chiropractic adjustments, soft tissue release, acupuncture and trigger point therapy.
Diagnosis of trigger points.
Diagnosis of trigger points typically takes into account symptoms, pain patterns, and manual palpation. When palpating the therapist will feel for a taut band of muscle with a hard nodule within it. Often a local twitch response will be elicited by running a finger perpendicular to the muscle fibres direction. Pressure applied to the trigger point will often reproduce the pain complaint of the patient and the referral pattern of the trigger point. Often there is a heat differential in the local area of the trigger point. 
Trigger points in the biceps Brachii muscle.
The Bicep Brachii is perhaps the most recognizable muscle in the body. It’s the muscle that is most often flexed when someone says ” show me your muscles”. It is composed of two heads, the long head and the short head. The short head originates on the coracoid process of the scapula, and the long head on the supraglenoid tubercle. Both heads merge to insert on the radial tuberosity and bicipital aponeurosis into the deep fascia on the medial part of the forearm. The main actions of this muscle are elbow flexion and forearm supination(rotation with the palm of the hand going upward). This muscle also assists shoulder flexion. Trigger points in this muscle mainly refer pain into the shoulder, with spillover into the posterior aspect above the scapula. A less common referral is into the anterior elbow and forearm. 
What is a trigger point
Dr Janet travel coined the term trigger point in 1942 to describe clinical findings with characteristics of pain related a discrete irritable point in muscle or fascia that was not caused by acute trauma, inflammation, degeneration, neoplasm or infection. The painful point can be palpated as a nodule or tight band in the muscle that can produce a local twitch response when stimulated. Palpation of the trigger point reproduces the pain and symptoms of the patient and the pain radiates in a predictable referral pattern specific to the muscle harbouring the trigger point.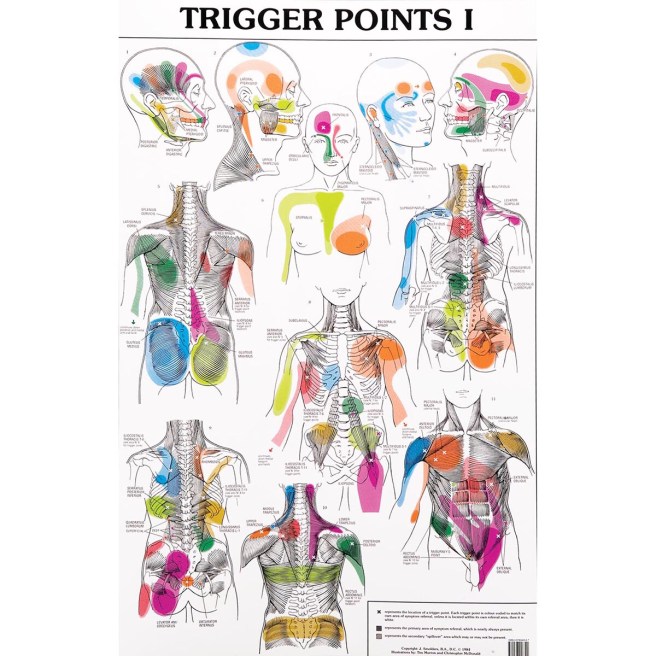
What to expect with a trigger point massage.
A treatment with Bryan is very user friendly. And, no, you don’t have to remove any clothing. However, bringing a t-shirt and a pair of shorts or sweats is recommended.
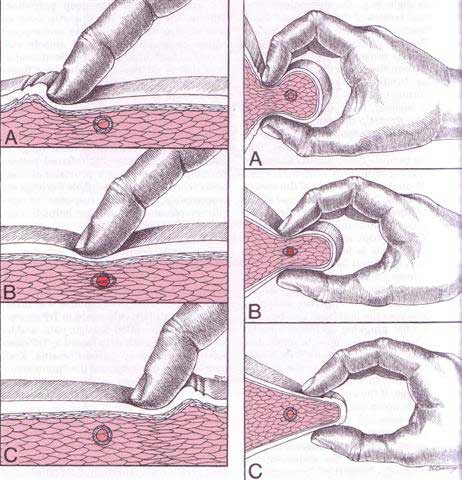
The first time you come for a treatment you will be asked to fill out a Client History form. Bryan will go over the information you provide, asking for more detail and discussing the type of pain you are having and its location.
The treatment itself involves locating the Trigger Points in the muscle or soft tissue and applying a deep focused pressure to the Point. This will reproduce the pain and the referral pattern that is characteristic of that pain.
The treatment will be uncomfortable at first, but as the Trigger Points release, the pain will decrease. The pressure will always be adjusted to your tolerance level. If, at any time, you feel too uncomfortable you can ask Bryan to ease off a bit.
Depending on your specific problem, Bryan may also use some stretching and / or range-of-motion techniques, as needed.
After treatment, it is usually recommended that the client apply moist heat to the area treated.
Trigger points in the pectoralis minor muscle.
The pectoralis minor is a small strap like muscle that is underneath (deep) to the pectoralis major. It originates on the third to fifth rib, near the costal cartilages. It’s insertion is on the coracoid process of the scapula. It acts to draw the scapula forward, downward, and inward at nearly equal angles ( think of rounding or shrugging your shoulders forward). This muscle is very often shortened and tight in people due to the high prevalence of desk jobs. This muscle pulls the shoulder blade forward resulting in the muscles in the back(rhomboid and mid traps) being chronically strained. Trigger points that form in the pec minor primarily refer pain over the anterior chest and shoulder, with spillover down the medial arm. Trigger points in the left side can mimic angina. 
What evidence do we have of whiplash?
Whiplash, or WAD (Whiplash Associated Disorders), refers to a neck injury where the normal range of motion is exceeded, resulting in injury to the soft-tissues (hopefully with no fractures) in the cervical region. There are a LOT of factors involved that enter into the degree of injury and length of healing time. Let’s take a closer look!
Picture the classic rear-end collision. The incident itself may be over within 300 milliseconds (msec), which is why it’s virtually impossible to brace yourself effectively for the crash as a typical voluntary muscle contraction takes two to three times longer (800-1000 msec) to accomplish.
In the first 50 msec, the force of the rear-end collision pushes the vehicle (and the torso of the body) forwards leaving the head behind so the cervical spine straightens out from its normal “C-shape” (or lordosis). By 75-100 msec, the lower part of the neck extends or becomes more C-shaped while the upper half flexes or moves in an opposite direction creating an “S” shape to the neck. Between 150-200msec, the whole neck hyper extends and the head may hit the head rest IF the headrest is positioned properly. In the last 200-300 msec, the head is propelled forwards into flexion in a “crack the whip” type of motion.
Injury to the neck may occur at various stages of this very fast process, and many factors determine the degree of injury such as a smaller car being hit by a larger car, the impact direction, the position of the head upon impact (worse if turned), if the neck is tall and slender vs. short and muscular, the angle and “springiness” of the seat back and relative position of the headrest, dry vs. wet/slippery pavement, and airbag deployment, just to name a few.
Some other factors that can predict recovery include: limited neck motion, the presence of neurological loss (nerve specific muscle weakness and/or numbness/tingling), high initial pain levels (>5/10 on a 0-10 scale), high disability scores on questionnaires, overly fearful of harming oneself with usual activity and/or work, depressive symptoms, post-traumatic stress, poor coping skills, headaches, back pain, widespread or whole body pain, dizziness, negative expectation of recovery, pending litigation, catastrophizing, age (older is worse), and poor pre-collision health (both mental and physical).
Research shows the best outcomes occur when patients are assured that most people fully recover and when patients stay active and working as much as possible. Studies have shown it’s best to avoid prolonged inactivity and cervical collars unless under a doctor’s orders. It’s also a good idea to gradually introduce exercises aimed at improving range of motion, postural endurance, and motor control provided doing so keeps the patient within reasonable pain boundaries. Chiropractic manipulation restores movement in fixed or stuck joints in the back and neck and has been found to help significantly with neck pain and headaches, particularly for patients involved in motor vehicle collisions. A doctor of chiropractic may also recommend using a cervical pillow, home traction, massage, and other therapies as part of the recovery process.
It is important to be aware that fear of normal activity and not engaging in usual activities and work can delay healing and promote chronic problems and long-term disability. It’s suggested patients avoid opioid medication use due to the addictive problems with such drugs. Ice and anti-inflammatory herbs or nutrients (like ginger, turmeric, and bioflavonoids) are safer options. Your doctor of chiropractic can guide you in this process!
Have you Been Told You Have TMJ Disorder?
Temporomandibular Disorder (TMD) is a term used to describe a group problems that cause pain in the temporomandibular joint, also called the TMJ. These problems can arise from the muscles around the joint, the disc within the joint or the bony portion of the joint itself. Imbalances between the muscles that open and close your jaw are the most common culprit.

Up to 25% of the population will suffer with TMD symptoms. Most patients are 20-50 years old and the condition is 2-3 times more common in females. Typical symptoms include: jaw clicking, limited mouth opening, possible jaw locking and pain. Chewing and eating usually make your symptoms more noticeable. TMD pain is generally described as an “ache” located in front of your ear canal but may also refer to other areas of your face, head, neck and shoulders. TMD patients often suffer from headaches.
TMD is more common in people who clench their jaw or grind their teeth, especially at night. Bad posture and emotional stress are contributors to this problem. You are three times more likely to suffer with TMD if you have been involved in a “whiplash” accident.
Conservative treatments, like those provided by our office, have been shown to be as effective as any surgery for most patients with TMD. Treatment is simple, focusing on “massaging” tightness out of the jaw muscles, restoring movement to any restricted joints (including your neck and upper back), and prescribing exercises to improve flexibility.
You should avoid aggravating activities like chewing gum or eating “rubbery” foods. Limit excessive talking. A custom fitted mouth guard may be prescribed to help minimize grinding & clenching and promote relaxation of your jaw muscles at night. Patients with night-time symptoms should avoid stressful activity before bedtime and try to sleep in a “neutral” position. In some cases, stress management techniques, like biofeedback, can assist you in learning how to relax your jaw muscles.
The Bird Dog

Today we are going to look at one of the most effective exercises to protect your lumbar spine from discogenic injury, the bird dog. A great way to work on both posterior chain and rotational stability, the bird dog is safe, effective and simple.
- Get on your hands and knees (four point position) with your knees and hands, hip and shoulders width apart.
- Your back is in neutral position (slightly arched) and your chin must be tucked in.
- Activate your lower abdominals (transversus abdomini) by bringing your belly button inward and by activating your pelvic floor muscles 20 to 30% of maximal contraction.
- Maintain a steady abdominal breathing while you simultaneously lift one leg backwards and the opposite arm overhead keeping your back in neutral position.
- Return to the initial position and repeat with the other leg and arm.
2 sets of 10 reps as part of your regular core/stability routine will have you well on your way to a life-proof low back!