Athletes and the general public alike often develop compensation patterns when mild, non-debilitating injuries go untreated. These compensatory patterns can significantly impact performance, whether in sports or daily activities, often resulting in pain and difficulty in movement. Recognizing and addressing these issues is crucial for maintaining optimal functionality and quality of life.
Our office is dedicated to identifying, correcting, and preventing these dysfunctional patterns as part of our comprehensive care approach, especially for patients dealing with long-term pain. When it comes to acute injuries—those that are new or recent—our focus on preventing these patterns is paramount. Addressing them early can lead to a quicker and smoother return to sports, work, and daily life.
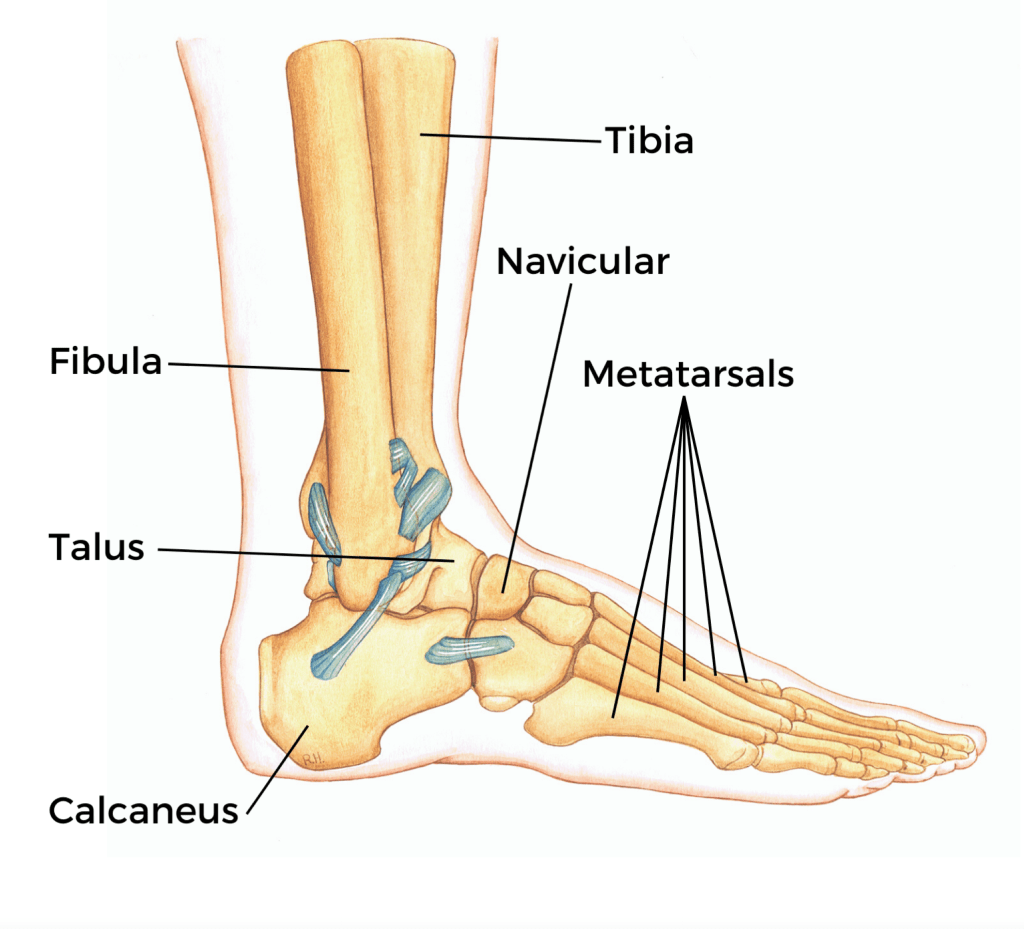
Untreated mild injuries can subtly alter the way we move, causing the body to adapt in ways that are not always beneficial. For example, an untreated sprained ankle might cause an individual to favor the uninjured foot, leading to imbalances and strain in other parts of the body. Over time, these imbalances can cause additional problems, such as knee, hip, or back pain. In athletes, even minor changes in movement patterns can lead to significant decreases in performance and an increased risk of further injury.
Our approach to care involves a thorough assessment of each patient’s movement patterns and injury history. This allows us to pinpoint areas where compensations may be occurring. By addressing these issues early, we can help prevent the development of chronic pain and dysfunction. For those already experiencing long-term pain, our goal is to correct these patterns to restore normal function and alleviate discomfort.
In acute injury cases, early intervention is key. When an injury is fresh, the body is in a heightened state of healing and adaptation. This is the ideal time to ensure that healing occurs correctly and that no maladaptive compensation patterns are established. Our treatment plans for acute injuries are designed to support the body’s natural healing processes while providing the guidance and interventions needed to maintain proper movement and function.
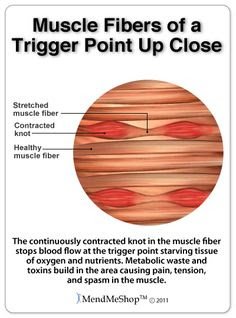
Preventing compensation patterns involves a combination of techniques tailored to each individual’s needs. This may include manual therapies to address soft tissue restrictions, joint mobilizations to restore proper alignment and movement, and corrective exercises to strengthen and retrain affected muscles. Education is also a critical component, as understanding how and why compensations occur can empower patients to make adjustments in their daily lives that support their recovery and long-term health.
For athletes, this approach not only helps in recovering from injuries but also enhances overall performance. By ensuring that movement patterns are efficient and free of compensations, athletes can move more effectively, reducing the risk of future injuries and optimizing their physical capabilities.
In conclusion, the development of compensation patterns following untreated mild injuries can lead to decreased performance and increased pain. Our office is committed to addressing these issues through a comprehensive approach that includes identifying, correcting, and preventing dysfunctional movement patterns. Whether dealing with chronic pain or recovering from a recent injury, our goal is to support our patients in achieving a quick and seamless return to their desired activities, free from pain and with improved functionality. Through early intervention and personalized care, we aim to enhance the quality of life and performance for all our patients.