A large number of factors have been identified as causes of trigger point activation. These include acute or chronic overload of muscle tissue, disease, psychological distress, systemic inflammation, homeostatic imbalances, direct trauma, radiculopathy, infections, and lifestyle choices such as smoking. Trigger points form as a local contraction of muscle fibres in a muscle or bundle of muscle fibres. These can pull on ligaments and tendons associated with the muscle which can cause pain to be felt deep inside a joint. It is theorized that trigger points form from excessive release of acetylcholine causing sustained depolarization of muscle fibres. Trigger points present an abnormal biochemical composition with elevated levels of acetylcholine, noradrenaline and serotonin and a lower ph. The contracted fibres in a trigger point constricts blood supply to the area creating an energy crisis in the tissue that results in the production of sensitizing substances that interact with pain receptors producing pain. When trigger points are present in a muscle there is often pain and weakness in the associated structures. These pain patterns follow specific nerve pathways that have been well mapped to allow for accurate diagnosis or the causative pain factor.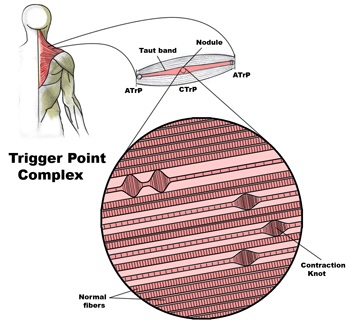
Laser Therapy
Diagnosis of trigger points.
Diagnosis of trigger points typically takes into account symptoms, pain patterns, and manual palpation. When palpating the therapist will feel for a taut band of muscle with a hard nodule within it. Often a local twitch response will be elicited by running a finger perpendicular to the muscle fibres direction. Pressure applied to the trigger point will often reproduce the pain complaint of the patient and the referral pattern of the trigger point. Often there is a heat differential in the local area of the trigger point. 
Snapping Hip. Not as horrific as it sounds.
The muscle responsible for flexing your hip toward your trunk, is called the Psoas. This muscle begins on your lower spine and passes through your pelvis to attach onto the top of your femur (thigh bone). Along this course, the muscle travels across the front of your hip socket and over several bony prominences. If the muscle is too tight, its tendon may rub over these “bumps”. This occasionally produces an audible snapping sound, hence the moniker, “snapping hip”, aka “psoas tendinopathy”.
 The tendon can be irritated by an acute injury, but more commonly from overuse- particularly repeatedly flexing your hip toward your trunk. The condition is also known as “dancer’s hip” or “jumper’s hip”, as movements associated with these activities are known culprits. Likewise, the condition is frequently seen in athletes who participate in rowing, track and field, hurdling, running (especially uphill), soccer, and gymnastics.
The tendon can be irritated by an acute injury, but more commonly from overuse- particularly repeatedly flexing your hip toward your trunk. The condition is also known as “dancer’s hip” or “jumper’s hip”, as movements associated with these activities are known culprits. Likewise, the condition is frequently seen in athletes who participate in rowing, track and field, hurdling, running (especially uphill), soccer, and gymnastics.
Your symptoms may include a “snapping” sound or sensation when you flex and extend your hip- although many cases are silent. Repeated rubbing causes inflammation and subsequent deep groin pain that can radiate to the front of your hip or thigh. Long-standing problems can trigger weakness or even limping.
The diagnosis of snapping hip is frequently overlooked. In fact, some studies show that identification is often delayed more than two years, while other potential causes are pursued. Fortunately, your problem has been recognized, and our office has several treatments to help you recover.
Psoas problems often start when one group of muscles is too tight, while another is too loose. Your home exercises will help to correct this problem. Depending upon the severity of your condition, you may need to avoid certain activities for a while. You should especially avoid repetitive hip flexion. Prolonged seated positions can encourage shortening of your hip flexors so be sure to take frequent breaks. Patients with fallen arches may benefit from arch supports.
Biceps Tendon Injury. The “suns out, guns out” injury.

Your biceps muscle attaches to your shoulder through two strong fibrous bands called “tendons.” The term “biceps tendinitis” means that one of these bands has become painfully irritated from strain or degeneration. Sometimes the tendon may be strained by an accident or lifting injury. Biceps tendinitis more often results from repeated pinching of the tendon beneath the bony part of your shoulder

from a condition called “impingement.” Repeated overhead activity, like throwing, swimming, gymnastics, and racquet sports are known culprits. Biceps tendinitis is often accompanied by other conditions, like rotator cuff tears or injuries to the cartilage around the rim of your shoulder joint. Factors that make you more likely to develop biceps tendinitis include: improper lifting techniques, inflexibility, poor posture, or repetitive overloading.
Your symptoms likely include a deep, throbbing ache over the front of your shoulder. The pain often refers toward the outside of your arm. The main job of your biceps muscle is to flex your elbow and turn your palm up, so overhead movements or activities that require flexion of your elbow may cause pain. Patients often report increased discomfort when initiating activity. Night time symptoms are common, especially if you lie on your affected shoulder. Be sure to tell your doctor if you notice popping, catching, or locking during movements, as this may suggest an additional problem. A painful, loud “pop” followed by relief with a visible bulge in your biceps (Popeye deformity) suggests that your tendon has ruptured.
Surgery is rarely required for biceps tendon problems unless you are a young athlete or worker who performs exceptionally heavy physical activity and have completely ruptured your tendon. The most effective treatment for the majority of biceps tendinitis patients is conservative care, like the type provided in our office. Initially, you may need to avoid heavy or repetitive activity, (especially overhead activity and elbow flexion) as returning to activity too soon may prolog your recovery. You should specifically avoid military presses, upright rows, and wide grip bench presses until cleared by your doctor. You may use ice over your shoulder for 10-15 minutes at a time each hour. The exercises described below will be a very important part of your recovery and should be performed consistently.
Another tunnel injury? Seriously?
Your radial nerve begins in your neck and travels past your elbow en route to its final destination in your hand. Just beyond your elbow, this nerve passes through a 2-inch area on the back of your forearm called the “Radial tunnel”. “Radial tunnel syndrome” means that your radial nerve has been compressed or irritated within this space-leading to forearm pain or hand weakness.

Radial tunnel syndrome is thought to result from muscular overuse, especially prolonged or excessive wrist extension or rotation. The most common cause of compression comes from excessive tightness in a muscle called the “Supinator”. Workers whose jobs require heavy or repetitive wrist movements are at an increased risk for this disorder. Occasionally, the radial nerve can become irritated from direct compression by a tight band or brace. The condition may be more common in those who have diabetes or thyroid problems.
Symptoms from irritation of the radial nerve depend upon which specific nerve fibers are irritated. The most common symptoms include pain, numbness, tingling or decreased sensitivity along the top of your forearm radiating toward your hand and thumb. The symptoms often mimic those of “tennis elbow.” When the nerve fibers that control muscle function become compressed, you may experience weakness when trying to extend your fingers, hand or wrist. Seventy percent of radial tunnel patients also have problems in their neck or upper back.
Conservative treatment of radial tunnel syndrome is generally successful. Fixing the problem means limiting excessive or repetitive wrist movements, especially extension and rotation. In severe cases, a splint may be necessary to limit your motion. Try to avoid compression of your forearm, particularly from tight bands or braces. Use of a tennis elbow brace will likely aggravate your symptoms. You may find relief by applying ice or ice massage to the area for 10-15 minutes at a time.
Cubital Tunnel Syndrome…. Ever heard of it?
Your cubital tunnel is the groove on the inside of your elbow, also called the “funny bone.” The funny part about the funny bone is that it is not actually a bone but rather a nerve, called the ulnar nerve. Your ulnar nerve begins in your neck and passes through the cubital tunnel on its way to your hand.
 When you flex your elbow, the ulnar nerve is required to both stretch and slide through your cubital tunnel. If your ulnar nerve is “stuck” in the tunnel and does not glide when you flex your elbow, this leads to traction and irritation of the nerve. This is called “cubital tunnel syndrome.” The nerve may also be irritated from direct compression, like leaning your elbow on the edge of a desk or from arthritic spurs. Cubital tunnel syndrome is the second most common nerve compression problem in the arm, behind carpal tunnel syndrome.
When you flex your elbow, the ulnar nerve is required to both stretch and slide through your cubital tunnel. If your ulnar nerve is “stuck” in the tunnel and does not glide when you flex your elbow, this leads to traction and irritation of the nerve. This is called “cubital tunnel syndrome.” The nerve may also be irritated from direct compression, like leaning your elbow on the edge of a desk or from arthritic spurs. Cubital tunnel syndrome is the second most common nerve compression problem in the arm, behind carpal tunnel syndrome.
Irritation of the ulnar nerve in the cubital tunnel causes pain, numbness or tingling that radiates from your elbow into your fourth and fifth fingers. Your symptoms can vary from a vague increased sensitivity to pain. The symptoms are common at night and are often progressive over time. In severe cases, you may begin to lose grip strength and fine muscle control.
Cubital tunnel syndrome is commonly seen in baseball, tennis and racquetball players. Workers who keep their elbows flexed such as holding a tool or telephone, or those who press the ulnar nerve against a hard surface like a desk, are at an increased risk for this disorder. Cubital tunnel syndrome affects men three to eight times as often as women and is more common in those who have diabetes or are overweight.
You should try to avoid prolonged elbow flexion or direct pressure over your elbow. Our office may prescribe a nighttime elbow splint that limits flexion.
Feels just like Carpal Tunnel but isn’t Carpal Tunnel……
Your Median Nerve begins in your neck and travels down your arm on its way to your hand. This nerve is responsible for sensation on the palm side of your first 3 ½ fingers and also controls some of the muscles that flex your fingers. The median nerve can sometimes become entrapped near your elbow as it travels through a muscle called the “pronator teres”. Compression of the median nerve by the pronator muscle is called “Pronator Syndrome.”

Pronator syndrome is often brought on by prolonged or repeated wrist and finger movements, i.e., gripping with the palm down. Carpenters, mechanics, assembly line workers, tennis players, rowers, and weight lifters are predisposed to this problem. The condition is more common in people with excessively developed forearm muscles and is also more common in your dominant arm. Pronator syndrome most often affects adults age 45-60 and females are affected about four times more frequently than males. People who suffer from diabetes, thyroid disease, and alcoholism have an increased risk for developing pronator syndrome.
Pronator syndrome produces symptoms very similar to a more common cause of median nerve compression called “carpal tunnel syndrome”. Symptoms of pronator syndrome include numbness, tingling, or discomfort on the palm side of your thumb, index, middle finger, and half of your ring finger. The discomfort often begins near the elbow and radiates toward your hand. Your symptoms are likely aggravated by gripping activities, especially those that involve rotation of the forearm, like turning a doorknob or a screwdriver. Unlike carpal tunnel syndrome, pronator syndrome symptoms are not generally present at night. You may sometimes feel as though your hands are clumsy. In more severe cases, hand weakness can develop.
To help resolve your condition, you should avoid activities that involve repetitive hand and forearm movements. Perhaps the most important aspect of your treatment plan is to avoid repetitive forceful gripping. You may apply ice packs or ice massage directly over the pronator teres muscle for ten minutes at a time or as directed by our office. In some cases, an elbow splint may be used to limit forearm movements. If left untreated, pronator syndrome can result in permanent nerve damage. Fortunately, our office has several treatment options available to help resolve your symptoms.
Golfer’s Elbow? Thats a thing?
Most of the muscles that flex your wrist are attached to a bony bump on the inside of your elbow called the “medial epicondyle.” Sometimes, through injury or overuse, the site where these muscles originate can become irritated or inflamed. This condition is called “medial epicondylitis”, or “golfer’s elbow.”
Although the condition is named “golfer’s elbow,” over 90% of those affected
are not even athletes, much less golfers. Nonetheless, the condition is more common in certain sports, especially golf, throwing, bowling, football, archery, and weight lifting. Occupations that require heavy gripping or repeated hand movements, like carpentry or typing, can predispose you to this condition. Smokers and people who are obese are more likely to experience this condition.
Medial epicondylitis is the most frequent cause of pain on the “inside” of your elbow but is 3-10 times less likely that its “outside” counterpart- lateral epicondylitis (i.e. “tennis elbow”). Medial epicondylitis is most common between the ages of 40 and 60. The condition strikes the dominant arm in over ¾ of cases. Your symptoms will likely include a dull aching pain over the bump on the inside of your elbow that becomes more intense with use. As the condition progresses, you may notice grip weakness or limitations when shaking hands, grasping objects, and opening jars. Be sure to tell your doctor if you notice numbness or tingling traveling toward your hand.
If left untreated, medial epicondylitis can last indefinitely. Studies show that up to 40% of untreated patients suffer prolonged discomfort, some as long as three years. Fortunately, conservative treatment like the type provided in our office is effective for relieving this condition. Our office may prescribe an elbow “counterforce brace” to help dampen stress to the irritated area. This type of brace should not be used in patients who have numbness or tingling radiating into their fingers. Some patients may benefit from a “wrist splint” that is used at night to allow your tendon to heal in a lengthened position. Using ice or ice massage over your elbow can help limit pain. Your home exercises will play an important role in your recovery.
Initially, you may need to avoid activities that cause an increase in pain, like gripping, lifting, golfing, throwing balls, or swinging a racquet. Be sure to warm up properly and stretch prior to any heavy physical activity. Smokers would benefit from quitting. Overweight patients should consider increasing their aerobic activity to shed excess pounds.
Our Condition of the Month: ITB Syndrome
Iliotibial Band Syndrome
Your iliotibial band is a fibrous band of tissue running from the crest of your hip, down to your knee. A muscle near the crest of your hip called the tensor fascia lata, attaches to this band to help control movements of your leg. Your iliotibial band passes over the point of your hip and over another bony bump on the outside of your knee called the lateral epicondyle. When the band is too tight, it can become painfully inflamed as it repeatedly rubs over the top of either of these bony projections. Irritation at the bony bump near the knee is called iliotibial band friction syndrome.
The condition usually presents as pain on the outside of your knee that becomes worse with repetitive knee flexion or extension. This condition is the leading cause of lateral knee pain in runners, especially slower “joggers.” The pain usually develops 10-15 minutes into the workout. You may sometimes feel or hear a click during movement. Symptoms generally ease at rest. Running on slick “wintry” surfaces may aggravate the condition. Excessively worn running shoes may be a culprit.
This problem is commonly caused by weakness in your gluteal muscles. When these muscles are weak, the muscle that attaches to your iliotibial band must contract harder to stabilize your hip. Having one leg longer than another is a known aggravating factor.
Runners should minimize downhill running and avoid running on a banked surface like the crown of a road or indoor track, as well as wet or icy surfaces. Runners should reverse directions on a circular track at least each mile. Bicyclists may need to adjust seat height and avoid “toe in” pedal positions. Avoid using stair climbers or performing squats and dead lifts. Sports cream and home ice massage may provide some relief of symptoms.
How can I have Tennis Elbow? I’ve never played tennis!
Most of the muscles that extend your wrist are attached to a bony bump on the outside of your elbow called the lateral epicondyle. Sometimes, through injury or overuse, the site where these muscles insert can become irritated or inflamed. This condition is called lateral epicondylitis or “tennis elbow”- although the majority of those affected do not play tennis.
Activities involving repetitive wrist extension are a common cause of this condition, i.e., tennis, carpentry, bricklaying, knitting, playing piano, typing, or lifting objects with your palm facing down. The condition is 3 times more likely to strike your dominant arm.
The pain often begins as an intermittent or gradual discomfort during activity and progresses so that even simple activities, like holding a coffee cup, become painful. Pain may increase when you straighten your arm, grip a doorknob or shake hands. The pain may vary from mild to severe and commonly radiates into the forearm, sometimes to the wrist.
Without treatment, “tennis elbow” usually lingers – 80% of patients still report pain after one year. The first step in a successful treatment plan is to modify or eliminate activities that cause symptoms. Try to avoid lifting heavy objects with your palm facing down. Tennis or racquetball players may need to consider changing to a lighter racket or a smaller handle. We may prescribe a “counter force brace” for your elbow. This brace will act as a temporary new attachment site for your muscles thereby reducing some of the stress to your elbow. Sports creams and home ice massage may provide relief as well. Be patient with your recovery!
