Chiropractic Care is a Safe and Effective Option
SATURDAY, May 19, 2018 — Chiropractic care can help ease low back pain when added to a comprehensive treatment plan, a new clinical trial has found.
Active-duty military personnel reported having fewer back problems when they visited a chiropractor along with receiving usual medical care, the researchers said.
“This study provides the strongest evidence to date that chiropractic is safe, that it’s effective and that it can be integrated into a multidisciplinary health care setting,” said lead researcher Christine Goertz. She is CEO of the nonprofit Spine Institute for Quality in Davenport, Iowa.
Still, at least one pain specialist said more research may be needed to confirm chiropractic’s value for lower back pain.
The study comes in the context of the ongoing U.S. opioid crisis. This epidemic of addiction has created an urgent need for research into pain management that doesn’t involve medications, such as chiropractic care, Goertz said.
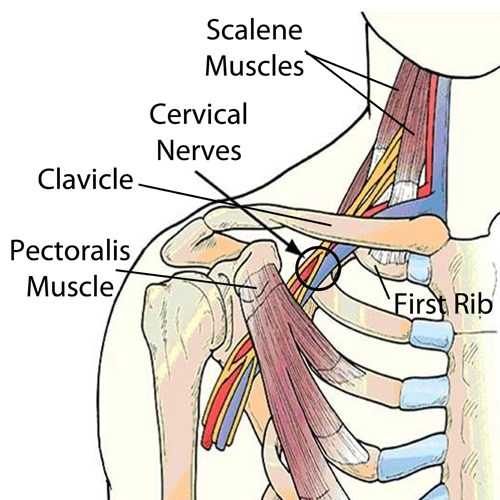
Chiropractic care focuses on the musculoskeletal system and the nervous system, mainly as they relate to the spine, according to the American Chiropractic Association.
Chiropractors aim to reduce low back pain by restoring joint mobility and proper alignment in the spine, through a process called spinal manipulation. Controlled force is applied hands-on to individual joints of the spine, to loosen them up and to stretch or break tight muscle tissue surrounding them.
Between 8 percent and 14 percent of U.S. adults seek chiropractic care, but there has been little research into its safety and effectiveness, Goertz said.
“Chiropractic has been controversial in the past, partially because chiropractic grew up outside the conventional medical care system,” she said. “For a long time, we really didn’t have a lot of evidence supporting the outcomes that both patients and doctors of chiropractic were reporting.”
To conduct a real-world test of chiropractic’s usefulness, Goertz and her colleagues enrolled 750 back pain patients at three military hospitals across the nation.
Low back pain is one of the most common reasons military personnel seek medical care, and a condition most likely to interrupt combat duty, according to the researchers.
Study participants were randomly assigned to receive either usual medical care, or that same care along with chiropractic.
Usual medical care involved seeing a doctor, taking pain medications, undergoing physical therapy and performing exercises, the study authors noted. Patients were treated for six weeks, then tracked for another six weeks.
“We found that at every time point, those patients that received chiropractic care had better outcomes in terms of their level of pain intensity and pain-related disability,” Goertz said.
“In addition, we also found that patients who saw the chiropractor tended to be much more satisfied with the care they received, and more likely to have perceived benefit from the care they received,” she added.
However, more adverse events were associated with chiropractic care.
The group receiving usual medical care reported 19 adverse effects, mostly muscle or joint stiffness attributed to physical therapy or exercise.
But 43 adverse events were reported by those also receiving chiropractic care, with 38 of them described as muscle or joint stiffness related to chiropractic procedures.
Dr. Karan Johar, medical director of NYC Pain Specialists and an attending physician at Lenox Hill Hospital in New York City, downplayed the study.
Johar noted that the investigators did not make sure each patient received the exact same type of chiropractic or traditional medical care, making it tough to pinpoint what worked for each patient.
The diagnosis of low back pain also is very broad, adding to the lack of clarity regarding how much chiropractic care contributed to patients’ well-being, he said.
“It’s very hard to assess if that study proves that chiropractic care helps,” Johar explained.
Insurance coverage for chiropractic care varies widely, Goertz noted. For example, Medicare covers chiropractic for spinal manipulation only, and will not reimburse chiropractors for examining patients.
“The majority of payers cover chiropractic in some way or another,” she said, “but the copay can be larger than the amount of the office visit.”
Goertz hopes more studies will find medical benefit in chiropractic care and that insurance companies will “follow the evidence” and improve coverage of these services.
The trial results were published online Friday in JAMA Network Open.
More information The U.S. National Institutes of Health has more about spinal manipulation for low back pain.
Copyright © 2018 HealthDay. All rights reserved.