Whiplash is a nonmedical term used to describe neck pain following an injury to the soft tissues of the neck (specifically ligaments, tendons, and muscles).It is caused by an abnormal motion or force applied to the neck that causes movement beyond the neck’s normal range of motion. It is usually caused by a flexion-extension motion of the neck that pulls and strains the neck muscles and ligaments.



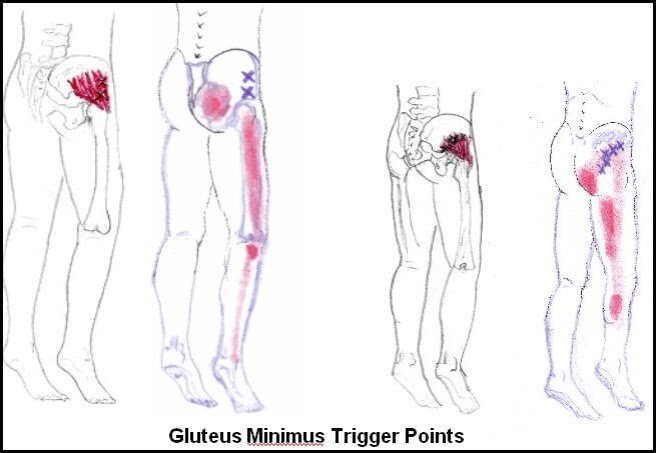
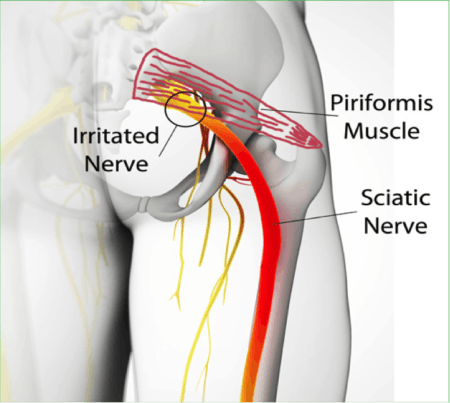
 The Rectus Femoris muscle is a large muscle that makes up part of the quadriceps group. It functions to extend the knee and flex the hip. It originates on the anterior inferior iliac spine and part of the acetabulum. It’s insertion is the patella via the quadriceps tendon and tibial tuberosity via the patellar ligament. Trigger points in this muscle refer deep into the knee. This muscle is an often overlooked source of knee pain.
The Rectus Femoris muscle is a large muscle that makes up part of the quadriceps group. It functions to extend the knee and flex the hip. It originates on the anterior inferior iliac spine and part of the acetabulum. It’s insertion is the patella via the quadriceps tendon and tibial tuberosity via the patellar ligament. Trigger points in this muscle refer deep into the knee. This muscle is an often overlooked source of knee pain.