The deltoid is the main muscle that makes up the shoulder. It originates on the clavicle, acromion, and spine of the scapula. It inserts on the deltoid tuberosity of the humerus. The deltoid acts at the shoulder to produce abduction, and assist with flexion and extension. The deltoid is especially prone to developing trigger points. These posterior style will refer pain into the anterior and lateral shoulder. Trigger points in the posterior delt will refer pain into the posterior shoulder with spillover down the lateral arm.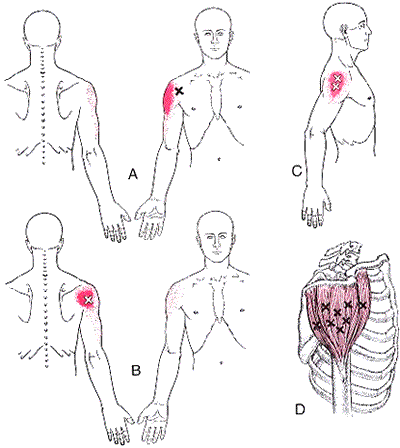
Aging
Lumbar Radiculopathy? That sounds ridiculous!
Your nervous system is basically a big electrical circuit. Your spinal cord transmits all of the electrical nerve impulses between your brain and lower back. From there, individual nerves emerge from your spine then travel to supply sensation and movement to a specific area of your buttock, legs and/or feet. This allows you to move and feel sensations like touch, heat, cold and pain. Anything that

interferes with this transmission can cause problems.
You have been diagnosed with a “Lumbar Radiculopathy”. This means that one or more of the nerves emerging from your lower back has become irritated or possibly pinched. This often results in pain, numbness or tingling in the specific area of your leg that is supplied by the irritated nerve. The term “Sciatica” is often used to describe this condition, because most (but not all) “lumbar radiculopathies” involve the sciatic nerve which supplies the back & outside of your thigh and calf. Symptoms of a lumbar radiculopathy may vary from a dull ache to a constant severe sharp shooting pain. Your symptoms are likely aggravated by certain positions or movements.
To solve this problem, we will treat the source of your nerve irritation. It is important for you to follow your treatment plan closely and be sure to tell us immediately if you experience any progression of your leg pain, numbness or weakness.
Trigger points in the adductor pollicis
The adductor pollicis is a muscle in the hand and acts on the thumb. It originates on the transverse head of the third metacarpal, the oblique head of the base of the second and third metacarpals, and the trapezoid and capitate bones. It inserts on the base of the proximal phalanx and ulnar sesamoid. This muscle acts to adduct and flex the thumb. Trigger points cause pain and aching along the outside of the thumb and hand, spillover pain may reach the thenar eminence.
Lumbar Degenerative Spondylolisthesis
Your lumbar spine (low back) is made up of five individual vertebra stacked on top of a bone called the sacrum. To allow for flexibility and movement, there is a cushion or “disc” in between each level. As we age, our discs and joints can wear and become thinner from a process called arthritis. This leads to additional changes, including loosening of the ligaments that hold your vertebra in place.

The term “degenerative lumbar spondylolisthesis” means that one of your vertebra has shifted forward on top of the one below as a result of arthritis and loosening ligaments. The condition usually comes on after age 50 and affects women six times more frequently than men. Degenerative spondylolisthesis occurs most commonly at your second lowest spinal level. (L4-5)
Sometimes, spondylolisthesis develops silently, but most patients report episodes of back pain that have occurred for many years. Patients often report increased pain when standing or when rising from a sitting position. Pain tends to increase throughout the day. If your nerve openings have become narrowed, the nerves may be pinched, and you may experience pain radiating into your legs. Leg symptoms that shift from side to side are characteristic of degenerative spondylolisthesis. Leg pain and tingling are fairly common, but be sure to tell your doctor if you notice more significant symptoms, like leg numbness, heaviness, weakness, loss of bowel or bladder function, or impotence.
Studies have shown no advantage for surgery over conservative care for most cases of degenerative spondylolisthesis. Approximately one-third of patients will experience progression of symptoms over time, and only 10-15% will ever need surgery to correct the problem. Fortunately, the majority of patients will benefit from treatment and exercises to help stabilize their spine.
You will need to perform your exercises consistently for sustained improvement. You should also try to add some type of aerobic exercise to your daily routine. Stationary cycling is a very good choice, and other options include water walking and swimming. Avoid wearing high heels. You may find some benefit for your arthritic symptoms by taking 1500mg of Glucosamine Sulfate each day. Using a hot pack for 10-15 minutes directly over your lower back may provide some benefit.
How do nutritional needs change as we age?
A great piece here from https://www.tallahassee.com/life/
Remember that high school health class? Now imagine a similar class geared toward students 65 and older.
That’s the idea behind nutrition education for older adults provided by the Family Nutrition Program, an Extension program of the University of Florida Institute of Food and Agricultural Sciences, which teaches people how to stay healthy and active on a budget.
“As we get older, our bodies change, and we are at greater risk for developing chronic diseases like high blood pressure and diabetes,” said Dr. Sharon Austin, adult programs specialist for the Family Nutrition Program. “My job is to encourage older adults to make small changes that will help them lead active, independent lives.”
The need for this kind of education is growing, Austin said. Adults over 65 are the fastest growing age group in the United States, and Florida has the highest percentage of adults 65 and older of any state, she said.
Everyone ages differently, and individual needs can be determined with your doctor, Austin said. But in general, as we get older, we may need to pay more attention to certain aspects of our eating and exercise routines to stay healthy, she said.
1. Calorie needs
As we age, our bodies typically need fewer calories because we are moving less and have less muscle mass, Austin said. “When you don’t need as many calories, you want to make sure you get more bang for your buck. That means avoiding ‘empty calories’ and choosing foods that are going to give you the nutrients you need,” she said.
2. Eating from every food group
One way to ensure that you are getting all the nutrients you need is to eat a variety of foods from every food group, Austin said. Take a look at ChooseMyPlate.gov to see how much of each food group to consume.
3. Fiber-rich foods
“Fiber isn’t just good for digestive health. It also helps lower risk for heart disease and diabetes, which are common chronic diseases in older adults,” Austin said.
You can get your daily recommended intake of fiber from whole grains, beans, and fresh fruits and vegetables, she said.
4. Fortified foods
Look for foods fortified with vitamin B12, vitamin D and calcium. “Vitamin B12 helps keep the body’s nerve and blood cells healthy, and calcium and Vitamin D help support bone health,” Austin said.
5. Drinking water
Older adults may have a decreased sense of thirst, and may more easily become dehydrated, Austin said. “One way to avoid dehydration is to sip water throughout the day from a cup or container you keep nearby during your daily routines,” she said
6. Exercises for mobility, balance and weight management
“When we talk about exercise for older adults, the goal is to set yourself up for physical independence. In our classes, we talk about everyday activities, such as cleaning the house or gardening, which can keep us strong and flexible, and burn calories. We also practice ways to increase balance, which can help us avoid falls and injury,” Austin said.
An exercise that many participants enjoy is the ‘couch potato mambo,’ Austin said. “Next time you’re sitting watching TV, get up and dance during the commercial break. It’s a small step toward health, and it’s fun.”
Lumbar Spondylolisthesis


the vertebral arches on its way from your brain to your tailbone. The term “lumbar isthmic spondylolisthesis” describes a condition where your arch has broken free from its anchor on the vertebral body, allowing the vertebral body to slide forward. Lumbar spondylolisthesis typically affects the lowest lumbar vertebra, L5, or occasionally the second lowest, L4.
The condition is sometimes caused by trauma, but more often follows a “stress fracture” involving the arch of the vertebra. This break and slippage is thought to result from repetitive movements, especially hyperextension (arching back) and rotation. The break usually happens during childhood but does not always cause symptoms when it occurs. Many times, the condition will lie dormant until later in life. Lumbar spondylolisthesis is present in six to seven percent of the population and affects males twice as often as females. The problem is more common in those who participate in sports. Some sports predispose children to this “break and slip”. Athletes who participate in gymnastics, rowing, diving, football, wrestling, weight lifting, swimming, tennis, volleyball, and track & field throwing sports (i.e. discus, shot put, etc) are at greatest risk.
The pain usually starts in your back but may radiate into your buttock or thigh. Your pain usually intensifies with standing upright for prolonged periods of time or leaning backwards, especially during heavy activity. Some women report increased symptoms during the later stages of pregnancy. Be sure to tell your doctor if you notice pain, numbness or tingling in your groin, a loss of bowel or bladder function, fever, night sweats, pain extending beyond your knee, or weakness in your legs.
Your doctor will “grade” your spondylolisthesis based on the percent of the vertebral body that has slipped forward. Your doctor will try to determine if your spondylolisthesis is “active”, meaning a recent break or “inactive”, referring to a long-standing problem. If your doctor has determined that your spondylolisthesis is new and has a chance of worsening, you may need to stop certain activities or sports for a period of time until your fracture heals. Sometimes a lumbar brace is used to help you recover more quickly. Patients with a long-standing “inactive” spondylolisthesis may benefit from a combination of treatments including stretching and strengthening. You should limit leaning backwards or sleeping on your stomach. Females should avoid wearing high heels.
Lumbar Spondylo-what?
Your spine is made up of 24 individual vertebrae, all stacked on top of each other. The lowest five vertebrae are referred to as your lumbar spine. Each vertebra has two basic components- the “body” and the “arch.” You can envision this as a coffee mug lying on its side. The cup would represent the vertebral body, and the handle would represent the arch. The spinal cord travels through each of the vertebral arches on its way from your brain to your tailbone.

The term lumbar spondylysis describes a condition where a part of the arch breaks free from its anchor site on the vertebral body. This condition most commonly occurs during adolescence while bones are hardening. When we are young our bones have taken shape but they have not yet become hardened. Think of this as a clay coffee mug that has not yet been fired in the kiln. During adolescence, our bones transform from this softer clay to a more brittle bone.
The condition is sometimes caused by trauma but more often is a “stress fracture” to the arch of the vertebra. This defect is thought to result from repetitive movements, especially hyperextension and rotation. The condition is more common in people who were born with a small or weak arch- think of a coffee mug handle with a very thin brittle attachment.
Lumbar spondylolysis usually affects the lowest lumbar vertebra- L5, or occasionally L4. Most patients are 10-15 years of age when they are diagnosed with the condition, although sometimes symptoms do not present until adulthood. It is more common in those who participate in sports. Some sports predispose children to this problem. Athletes who participate in diving, wrestling, weight lifting, track, football and gymnastics have the highest incidence of spondylolysis.
The pain usually starts in your back but may radiate into your buttock or thigh. Your pain usually intensifies with standing upright for prolonged periods of time or leaning backwards. You should limit movements that involve hyperextension, like leaning backwards. Females should avoid wearing high heels.
Your doctor likely performed x-rays or an MRI to make the diagnosis of spondylolysis. If your doctor has determined that your spondylolysis is new and has a chance of worsening, you may need to stop certain activities or sports for a period of time until your fracture heals. Sometimes a lumbar brace is used to help you recover more quickly.
What is Lumbar Stenosis?

The term stenosis means “narrowing” of a tube or opening. Spinal stenosis means that the tube surrounding your spinal cord and nerve roots has become too small, and your nerves are being compressed. Stenosis can arise in different ways. Sometimes, people are born with a spinal canal that is too small. Other times, the canal may have been narrowed by surgery or conditions like disc bulges. Most commonly, spinal stenosis arises from chronic arthritic changes that narrow the canal. This type of stenosis usually develops slowly over a long period of time, and symptoms show up later in life.
Patients with stenosis often report pain, tingling, numbness or weakness in their legs. Lower back pain may or may not be present, but leg symptoms are usually more bothersome. You may notice increasing symptoms from standing or walking and relief while sitting because the available space in your spinal canal decreases when you stand, walk or lean back and increases when you sit or flex forward. Walking down hill is usually more uncomfortable than walking up hill. You may notice that when you walk with a shopping cart or lawn mower, you are more comfortable, as this promotes slight flexion. Sleeping on your side in a fetal position with a pillow between your knees may be most comfortable.
The natural course of spinal stenosis is variable. Most patients notice their symptoms stay about the same over time, while others are divided into fairly equal groups who either improve or worsen. Be sure to tell your doctor if you notice that your legs become cold, swollen or change color. Likewise, tell us if you notice a fever, unexplained weight loss, flu-like symptoms, excessive thirst or urination, numbness in your groin or loss of bladder control.
While there is no non-surgical cure for stenosis, we offer potent treatments to help ease your symptoms. Treatment is focused on helping improve your mobility so that you can walk and function better. You will be given exercises to help with conditioning. You should avoid activities that increase your pain, including heavy lifting or those that cause you to extend your back, like prolonged standing or overhead activity. When you are forced to stand, you may find relief by slightly elevating one foot on a stool or bar rail. You may find relief while washing dishes if you open your cabinet door and alternately rest one foot on the inside of the cabinet to provide a little bit of flexion. Recumbent cycling is often a more tolerable alternative to walking or running. Some patients report relief by using an inversion table.
Thumb/Wrist pain from De Quervain’s Disease…..
Tendons are strong, fibrous bands of tissue connecting muscles to bones. Some tendons are covered by a protective, lubricated insulation called a “synovial sheath.” The two tendons on the thumb-side of your wrist that extend and abduct your thumb into a “hitchhiker” position are covered by a sheath. Normally, these tendons move freely within this covering, much like a sword sliding through a sheath.

If these tendons and sheaths are forced to repetitively rub against the bones of your wrist, they can become painfully swollen. This condition is called De Quervain’s tenosynovitis.
The pain of De Quervain’s tenosynovitis may begin abruptly, but more commonly starts gradually and increases over time. The pain is provoked by movements of your thumb or wrist. In more severe cases, you may notice swelling on the outside of your wrist. Some patients complain of “catching” or a slight “squeaking” sound while moving their wrist.
Activities like gardening, knitting, cooking, playing a musical instrument, carpentry, walking a pet on a leash, texting, video gaming and sports like golf, volleyball, fly fishing and racquet sports are known triggers. The condition was once known as “Washer woman’s sprain,” since wringing out wet clothes can trigger the problem. Lifting infants or children by placing your outstretched finger and thumb beneath their armpit has led to the nicknames of “Mommy thumb” or “Baby wrist.”
The condition strikes women much more frequently than men. It typically affects middle-age adults and is more slightly common in African-Americans, patients with diabetes or rheumatoid arthritis may be at higher risk for this problem.
Many patients will experience resolution of their symptoms through conservative care, like the type provided in our office. You should avoid lifting, grasping and pinching movements, especially when your wrist is bent toward either side. You may need to find alternate ways to lift children and perform work, sport and leisure activities. Video game players and those who text should take frequent breaks and try to hold their wrists straighter. Avoid wearing tight wristbands. Applying ice to your wrist for 10 minutes every hour or performing an “ice massage” (freeze a paper cup filled with water, tear off the bottom to expose the ice, massage over the tendons in a figure-eight pattern for 6-10 minutes, taking breaks as needed) can provide relief.
Patients who have severe pain or swelling are less likely to respond to conservative care. These patients may require a cortisone injection to relieve their pain, however, surgery is rarely necessary.
I’m getting old Doc… Getting old….
Your lumbar spine (low back) is made up of 5 individual vertebrae stacked on top of a bone called the “sacrum”. To allow for flexibility and movement, there is a cushion or “disc” in between each level. As we age, these discs can wear and become thinner over time. This leads to additional changes, including bone spurs and narrowing of the opening where your nerves exit your spine.
 This process is called “lumbar spondylosis”, or simply, “arthritis”. This problem most commonly involves the vertebra at the very base of your spine, which bear the highest loads.
This process is called “lumbar spondylosis”, or simply, “arthritis”. This problem most commonly involves the vertebra at the very base of your spine, which bear the highest loads.
Lumbar arthritis is exceptionally common, affecting people as young as 20 and becoming extremely likely by age 70. How quickly you develop low back arthritis is largely a trait you inherited from your parents. Other factors may play a role, including a history of trauma, smoking, operating motorized vehicles, being overweight and/ or performing repetitive movements (i.e. lifting, twisting, bending or sitting). Men seem to be affected slightly more often than women.
Symptoms often begin as back and buttock pain that gradually worsens over time. Stiffness may be present upon arising in the morning. Pain is relieved by rest or light activity and aggravated by strenuous work. Sometimes your nerves can become “pinched” in narrowed openings where they exit your spine. This can cause “sciatica” which results in pain, numbness, or tingling radiating into your leg along the path of the irritated nerve. Be sure to tell your doctor if you notice any weakness or if you have fever, abdominal pain, change in bowel or bladder function, or pain in your groin crease.
Arthritic changes can be seen on x-rays, but interestingly, the amount of wearing does not seem to correlate directly with the severity of your symptoms. People with the same degree of arthritis may have symptoms ranging from none to severe. Most researchers believe that the symptoms of osteoarthritis are not the direct result of the disease, but rather, from the conditions that preceded the disease and those that develop subsequent to it, like joint restrictions and muscle tightness. Fortunately, those conditions are treatable and our office has a variety of tools to help relieve your pain.
In general, you should avoid repeated lifting and twisting and take frequent breaks from prolonged sitting, especially in motorized vehicles. Avoid any position that causes an increase in radiating pain. Low-impact activities, like walking, stationary cycling, water aerobics, and yoga may be helpful.

