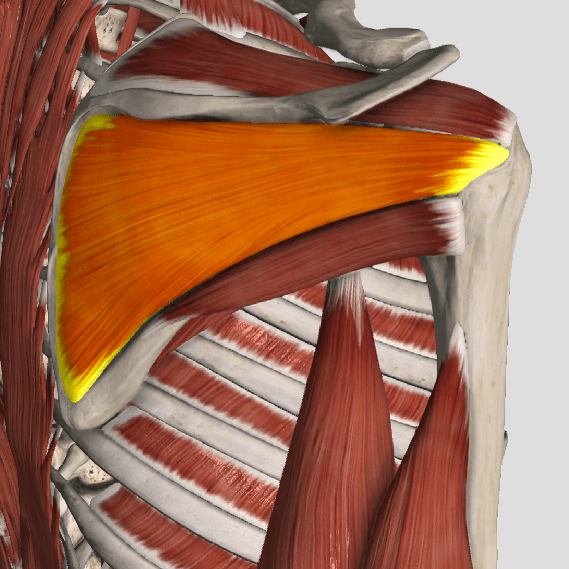
One of the most common causes of shoulder pain is a rotator cuff (RC) tear. To determine just how common this is, one study looked at a population of 683 people regardless of whether or not they had shoulder complaints. There were 229 males and 454 females for a total of 1,366 shoulders. (The participants’ average age was 58 years, ranging from 22 to 87 years old.)
The research team found 20.7% had full thickness rotator cuff tears. Of those with shoulder pain, only 36% had tears found on ultrasound. Of those without shoulder pain, 17% also had tears! Risk factors for an increased for tearing of the rotator cuff include a history of trauma, the dominant arm (ie your right arm if you’re right handed), and increasing age.
In a review of radiologic studies of 2,553 shoulders, researchers found full-thickness rotator cuff tears in 11.75% and partial thickness tears in 18.49% of the subjects for a total of 30.24% having some degree of tearing. In this group, about 40% of tears were found in pain-free shoulders. The researchers concluded that rotator cuff tears are common and frequently asymptomatic.
Both of these studies support the necessity to FIRST consider the patient’s clinical presentation and then correlate that with the imaging results. In other words, the presence of a RC tear on an image (usually MRI or ultrasound) does NOT necessarily mean there is pain (and vise versa)!
So what other things could be causing the shoulder pain? There are many: impingement, tendonitis, bursitis, muscle strain, capsular (and other ligament) sprain, frozen shoulder, and osteoarthritis (the “wearing out” type). Also, rheumatoid arthritis, lupus, polymyalgia rheumatica and other autoimmune types of “arthropathies,” fibromyalgia, a herniated cervical disk, shoulder dislocations, whiplash injuries, and more!
Most importantly, we must NOT forget to include referred pain to the shoulder from an impaired heart (such as coronary heart disease or heart attack), lung, liver, or gall bladder as these problems commonly refer pain to the shoulder and may represent a MEDICAL EMERGENCY!