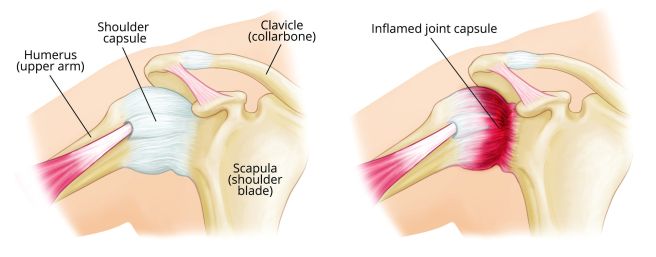
Shoulder capsulitis
Shoulder capsulitis happens when the strong connective tissue surrounding the shoulder becomes thick, stiff and inflamed, causing pain and loss of motion in the shoulder in all directions. It is sometimes called adhesive capsulitis or frozen shoulder.
The exact cause of this condition is unknown, but the risk of suffering from it increases following prolonged shoulder immobilization, a stroke or other shoulder conditions.
People over 40 are more prone to developing this condition and women are more commonly affected than men. Diseases such as diabetes, thyroid dysfunction and cardiovascular diseases can increase the risk of suffering from shoulder capsulitis.
▬▬▬▬▬
Structures involved
The glenohumeral joint capsule is involved in this condition. When it thickens, the capsule limits movements of the shoulder. The presence of a natural joint lubricant called synovial fluid also tends to diminish during a capsulitis.
1
▬▬▬▬▬
Signs & Symptoms that you may experience with Shoulder Capsulitis
Everyone will react differently in the event of capsulitis and recovery will depend on its intensity. Shoulder capsulitis generally causes pain and loss of range of motion in the shoulder. This condition typically develops slowly and can last from a few months to a few years. Symptoms of shoulder capsulitis can generally be categorized into three progressive stages.
In the first one, called the freezing stage, the shoulder becomes progressively stiffer and painful. Pain can be worse at night, especially if you sleep on your affected side.
In the second one, called the frozen stage, stiffness in the shoulder joint is important. Pain may begin to diminish during this stage but the range of motion in the shoulder is very limited and muscles start to lose their strength.
The last stage, called the thawing stage, is the beginning of recovery. There is a reduction in pain and a gradual increase in movement.
▬▬▬▬▬
Recovery
Prognosis is favorable for the majority of people affected but recovery can take a long time, ranging from one to two years. Your rehabilitation plan, health, fitness & nutritional status will affect recovery speed. Although you can expect to recover from this condition, some mobility restrictions may persist, particularly in regard to range of motion at the shoulder.
▬▬▬▬▬▬▬▬▬▬▬▬▬▬▬▬▬▬▬▬▬▬▬▬▬▬▬▬▬▬▬▬▬▬▬▬▬▬▬▬▬▬▬▬▬▬▬▬
▶ WHAT TO DO
Early Stage
Relative rest is a good way to protect your shoulder and prevent further damage during the first stage, but it’s important to avoid overprotecting your shoulder. It might be necessary to reduce pain-inducing movement and activities. Progressive return to your activities of daily living, range of motion exercises and light cardiovascular exercise will allow better recovery.
Rehabilitation for Shoulder Capsulitis
Follow your practitioner’s advice. It will help you manage the different stages of a capsulitis and will increase the likelihood of successful rehabilitation. Your practitioner will assist you during your rehabilitation program in order to regain your normal range of motion, strength and endurance and functional status.
As per the principles of rehabilitation for shoulder capsulitis, range of motion exercises are an important element of functional recovery. A progressive exercise program is pretty standard.
▶ WHAT TO AVOID
Don’t rely on passive treatment only. Each phase of the rehabilitation process is important. Patients that are actively involved in their treatment plan tend to recover faster. Keep in mind that pain is not always a good indicator of tissue damage. As soon as you feel better and the pain is well managed in collaboration with your therapist, you should reintroduce light range of motion and strengthening exercises as tolerated.