Seniors
The Best Diet For Fibromyalgia?

Fibromyalgia (FM) and its cause remains a mystery, but most studies suggest that FM is NOT the result of a single event but rather a combination of many physical, chemical, and emotional stressors.
The question of the month regarding the BEST FM diet is intriguing since one might assume that the many causes should mean that there isn’t one dietary solution. But is that true? Could there be a “best diet” to help ease the symptoms from such a multi-faceted disorder?
Certainly, healthy eating is VERY important for ALL of us regardless of our current ailment(s). Obesity is rampant largely due to the fact that 60% of the calories consumed by the “typical” American center around eating highly inflaming food that include those rich in Sugar, Omega-6 oil, Flour, and Trans fats (“SOFT” foods, if you will!). Obesity has been cited as “an epidemic” largely due to kids and adults becoming too sedentary (watching TV, playing on electronic devices, etc.) and eating poorly.
Perhaps the BEST way to manage the pain associated with FM and to maintain a healthy BMI (Body Mass Index, or ratio between height and weight) is to substitute ANTI-INFLAMING foods for those that inflame (or SOFT foods).
You can simplify your diet by substituting OUT “fast foods” for fruits, vegetables, and lean meats. So there you have it. It’s that simple. The problem is making up your mind to change and then actually doing it. Once these two things take place, most everyone can easily “recalibrate” their caloric intake and easily adapt.
Not only have studies shown that chronic illnesses like heart disease, stroke, and diabetes significantly benefit by following this simple dietary shift, but so does pain arising from the musculoskeletal system! This is because the human body is made up largely of chemicals, and chemical shifts are constantly taking place when it moves. If you reach for an anti-inflammatory drug like ibuprofen or naproxen and it helps, it’s because you ARE inflamed and the drug reduces the pain associated with that inflammation. This is an indication that an anti-inflammatory diet WILL HELP as well (but without the negative side effects)!
The list of chronic conditions that result in muscle pain not only includes FM but also obesity, metabolic syndrome, and type II diabetes. Conditions like tension-type and migraine headaches, neck and back pain, disk herniation, and tendonopathies and MANY more ALL respond WELL to making this SIMPLE change in the diet. For more information on how to “DEFLAME,” visit http://www.deflame.com! It could be a potential “lifesaver!”
I get dizzy when I have a headache. Should I worry?
Dizziness, neck pain, and headaches are very common symptoms that may or may not occur at the same time. Though this interrelationship exists, this month’s article will focus primarily on dizziness, particularly related to dizziness that occurs after standing.
First, it is important to point out that it is VERY common to be light headed or dizzy when standing up too fast, which is typically referred to as orthostatic hypotension (OH). OH is frequently referred to as a benign symptom, but new information may challenge this thought.
Let’s review what happens. When we are lying down, our heart does not have to work as hard as when we are upright; therefore, our blood pressure (BP) is usually lower while we lay in bed. When standing up, blood initially pools in the legs until an increase in blood pressure brings oxygen to the brain. This either resolves or prevents dizziness.
Orthostatic hypotension is defined as a blood pressure drop of >20 mm Hg systolic (the upper number—heart at FULL contraction), 10 mm Hg diastolic (lower number—heart at FULL rest), or both. This typically occurs within seconds to a few minutes after rising to a standing position.
There are two types of OH—delayed OH (DOH) where the onset of symptoms are not immediate but occur within three minutes of standing and “full” OH, which is more serious and occurs immediately upon rising. According to a 2016 study published in the prestigious journal Neurology, researchers reviewed the medical records of 165 people who had undergone autonomic nervous system testing for dizziness. The subjects averaged 59 years of age, and 48 were diagnosed with DOH, 42 with full OH, and 75 subjects didn’t have either condition.
During a ten-year follow-up, 54% of the DOH group progressed to OH, of which 31% developed a degenerative brain condition such as Parkinson’s disease or dementia. Those with initial DOH who also had diabetes were more likely to develop full OH vs. those without diabetes.
The early death rate in this 165 patient group was 29% for those with DOH, 64% with full OH, vs. 9% for those with neither diagnosed condition. The authors point out that those initially diagnosed with DOH who did NOT progress into full OH were given treatment that may have improved their blood pressure.
The authors state that a premature death might be avoided by having DOH and OH diagnosed and properly managed as early as possible. They point out that a prospective study is needed since this study only looked back at medical records of subjects who had nervous system testing performed at a specialized center, and therefore, these findings may not apply to the general population.
The value of this study is that this is the FIRST time a study described OH (or DOH) as a potentially serious condition with recommendations NOT to take OH/DOH lightly or view it as a benign condition. Since doctors see this a lot, a closer evaluation of the patient is in order.
What Exercises Should I Do For Fibro?

Fibromyalgia (FM) is a very common, chronic condition where the patient describes “widespread pain” not limited to one area of the body. Hence, when addressing exercises for FM, one must consider the whole body. Perhaps one of the most important to consider is the squat.
If you think about it, we must squat every time we sit down, stand up, get in/out of our car, and in/out of bed. Even climbing and descending steps results in a squat-lunge type of movement.
The problem with squatting is that we frequently lose (or misuse) the proper way to do this when we’re in pain as the pain forces us to compensate, which can cause us to develop faulty movement patterns that can irritate our ankles, knees, hips, and spine (particularly the low back). In fact, performing a squatting exercise properly will strengthen the hips, which will help protect the spine, and also strengthens the glutel muscles, which can help you perform all the daily activities mentioned above.
The “BEST” type of squat is the free-standing squat. This is done by bending the ankles, knees, and hips while keeping a curve in the low back. The latter is accomplished by “…sticking the butt out” during the squat.
Do NOT allow the knees to drift beyond your toes! If you notice sounds coming from your knees they can be ignored IF they are not accompanied by pain. If you do have pain, try moving the foot of the painful knee about six inches (~15 cm) ahead of the other and don’t squat as far down. Move within “reasonable boundaries of pain” by staying away from positions that reproduce sharp, lancinating pain that lingers upon completion.
What is Whiplash?
Whiplash is an injury to the soft-tissues of the neck often referred to as a sprain or strain. Because there are a unique set of symptoms associated with whiplash, doctors and researchers commonly use the term “whiplash associated disorders” or WAD to describe the condition.
WAD commonly occurs as a result of a car crash, but it can also result from a slip and fall, sports injury, a personal injury (such as an assault), and other traumatic causes. The tissues commonly involved include muscle tendons (“strain”), ligaments and joint capsules (“sprains”), disk injuries (tears, herniation), as well as brain injury or concussion—even without hitting the head!
Symptoms vary widely but often include neck pain, stiffness, tender muscles and connective tissue (myofascial pain), headache, dizziness, sensations such as burning, prickly, tingling, numbness, muscle weakness, and referred pain to the shoulder blade, mid-back, arm, head, or face. If concussion occurs, additional symptoms include cognitive problems, concentration loss, poor memory, anxiety/depression, nervousness/irritability, sleep disturbance, fatigue, and more!
Whiplash associated disorders can be broken down into three categories: WAD I includes symptoms without any significant examination findings; WAD II includes loss of cervical range of motion and evidence of soft-tissue damage; and WAD III includes WAD II elements with neurological loss—altered motor and/or sensory functions. There is a WAD IV which includes fracture, but this is less common and often excluded.
Treatment for WAD includes everything from doing nothing to intensive management from multiple disciplines—chiropractic, primary care, physical therapy, clinical psychology, pain management, and specialty services such as neurology, orthopedics, and more. The goal of treatment is to restore normal function and activity participation, as well as symptom management.
The prognosis of WAD is generally good as many will recover without residual problems within days to weeks, with most people recovering around three months after the injury. Unfortunately, some are not so lucky and have continued neck pain, stiffness, headache, and some develop post-concussive syndrome. The latter can affect cognition, memory, vision, and other brain functions. Generally speaking, the higher the WAD category, the worse the prognosis, although each case MUST be managed by its own unique characteristics. If the injury includes neurological loss (muscle strength and/or sensory dysfunction like numbness, tingling, burning, pressure), the prognosis is often worse.
Chiropractic care for the WAD patient can include manipulation, mobilization, and home-based exercises, as well as the use of anti-inflammatory herbs (ginger, turmeric, proteolysis enzymes (bromelain, papain), devil’s claw, boswellia extract, rutin, bioflavonoid, vitamin D, coenzyme Q10, etc.) and dietary modifications aimed at reducing inflammation and promoting healing.
* 83% of those patients involved in an MVA will suffer whiplash injury and 50% will be symptomatic at 1 year.
* 90% of patients with neurologic signs at onset may be symptomatic at 1 year.
* 25- 80% of patients who suffer a whiplash injury will experience late-onset dizziness
* Clinicians should be observant for radiographic signs of instability, including interspinous widening, vertebral subluxation, vertebral compression fracture, and loss of cervical lordosis.
* Horizontal displacement of greater than 3.5 mm or angular displacement of more than 11 degrees on flexion/extension views suggests instability
What to do about FM #pain?
Fibromyalgia (FM) is a very common condition affecting approximately ten million Americans (2-4% of the population)—with a ratio of about four women to each man with the disease. Part of the diagnosis and treatment challenge is that many of the complaints associated with FM occur in ALL of us at some point, such as fatigue, generalized whole body aches/pains, non-restorative sleep, depression, anxiety, etc. So what is the difference between the FM sufferer and those without it? Let’s take a look!
The primary distinction between patients with FM and the “rest of us” has to do with the word “chronic.” This term means “…persisting for a long time or constantly recurring; long-standing, long-term.” In fact, the term “fibromyalgia” is described as a complex chronic pain disorder that causes widespread pain and tenderness that may present body wide or migrate around the body. It is also known to “wax and wane over time,” meaning it flares up and down, off and on.
The diagnosis of FM is typically made by eliminating every other possible cause. Hence, after blood tests and x-ray or other imaging, the ABSENCE of other problems helps nail down the diagnosis of “primary fibromyalgia.” Then there is “secondary fibromyalgia,” which is DUE TO a known disorder or condition such as after trauma (like a car accident), rheumatoid arthritis, migraine headache, irritable bowel syndrome, “GERD” (which is heart burn due to reflux), pelvic pain, overactive bladder, tempromandibular joint dysfunction (jaw pain, with or without ringing in the ears), or stress. It’s also often accompanied by anxiety, depression, and/or some other mental health condition.
It should be clearly understood that there is no “cure” for FM. It has also been widely reported in many studies that the BEST management approach for FM is through a TEAM of healthcare providers. This team is frequently made up of primary care doctors, doctors of chiropractic, massage therapists, mental / behavioral specialists, physical therapists, and perhaps others (acupuncturist, nutritionist, stress management specialists, and more).
The “general” treatment approach is typically done with medications, cognitive behavioral therapies (CBT), gentle exercise, and manual therapies. Additionally, patients are encouraged to participate in the healing process via self-management strategies that focus on reducing stress and fatigue, optimizing diet, and developing a consistent sleep habit.
Think of the role of the chiropractor as a strong member of the team. A doctor of chiropractic can offer many of the known methods of managing FM described above, as their training includes diet and nutrition, stress management, exercise training, and ability to provide “whole person care.” Treatments delivered in the chiropractic setting like spinal manipulation, mobilization, and massage offer GREAT relief to FM patients! Again, coordinating care between various providers is the best approach, but you need someone willing and able to do that. A doctor of chiropractic is a great choice!
It is very difficult to manage FM on your own. Let a doctor of chiropractic tailor a treatment plan that is appealing to you and your specific interests. Managing FM is definitely NOT a “…one size fits all” approach like an inhaler is for asthma. Each individual’s situation is too highly unique!
Can Chiro Help My Headache?
Everyone, well at least almost everyone, has had headaches from time to time, and we all know how miserable they can make us feel. In fact, at some point in time, 9 out of 10 Americans suffer from headaches that range between mild and dull to throbbing, intense, and debilitating, sometimes to the point of requiring bed rest in a dark, quiet room.
The common reflex is to reach for that bottle of pills and pray the headache subsides so you don’t have to call in sick and lose another day of productivity when you have so much to do. Unfortunately, between the side effects of many medications designed to help headaches and the pain associated with the headache, this approach is frequently NOT the answer. So what is?
The good news is that many studies have identified spinal manipulation therapy (SMT), the main type of care utilized by chiropractors, as being very effective for popular types of headaches—in particular tension-type headaches that arise in the neck. An important 2001 study reported that SMT provided almost immediate relief for headaches that arose in the neck with SIGNIFICANTLY fewer side effects and longer-lasting results compared with commonly prescribed medications.
Another interesting study that found similar results included tracking the prevalence/frequency of headaches after treatment stopped. The authors of the study reported the patients receiving SMT had continued to experience sustained benefits throughout the following weeks, and even months, in contrast to those in a medication treatment group where headaches came back almost immediately after they discontinued treatment.
The most commonly prescribed medication for tension-type headaches are non-steroidal anti-inflammatory drugs (NSAIDs). Common over-the-counter options include ibuprofen (Advil, Nuprin, etc.) and Aleve (Naproxen). For those who can’t take NSAIDs because of blood thinning and/or stomach-liver-kidney problems, doctors commonly prescribe acetaminophen (Tylenol), but it can be hard on the liver and kidneys, especially when taken over time.
So, what can you expect from a visit to a chiropractor for your headaches? The typical approach begins with a thorough history and examination with an emphasis of evaluating the neck and its associated function. Your doctor of chiropractic may also perform tests designed to reduce pain and some that provoke a pain response to identify the “pain generator” or cause!
Because each patient is unique, the type of care provided will be individually determined based on the findings, the patient’s age, comfort, and preference of both the provider and patient.
So, the next time you find yourself reaching for pills because of headaches, remember that there are better options! Give chiropractic a try. You’ll be GLAD you did!!!
What is Cervical Spondylosis?
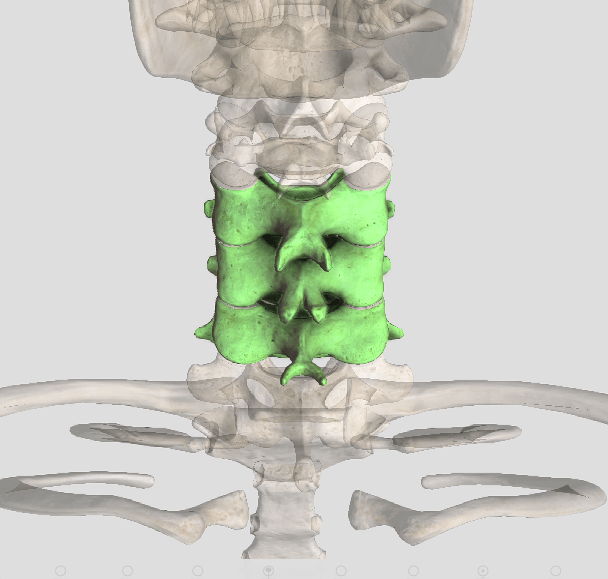
Cervical spondylosis (CS) is another term for osteoarthritis (OA) of the neck. It is a common, age-related condition that you will probably develop if you live long enough. Or, if you suffered a neck injury as a youth, it can develop within five to ten years of the injury, depending on the severity. According to the Mayo Clinic, CS or OA affects more than 85% of people over 60 years old, and that is probably a conservative estimate!
Common symptoms associated with CS/OA vary widely from no symptoms whatsoever to debilitating pain and stiffness. For example, when CS crowds the holes through which the nerves and/or spinal cord travel, it creates a condition called spinal stenosis that can result in numbness, tingling, and/or weakness. In severe cases, this can even affect bowel or bladder control (which is an EMERGENCY)!
CS occurs when the normal slippery, shiny cartilage surfaces of the joint(s) gradually thin and eventually wear away. Bone spurs often form, which results from the body trying to stabilize an unstable joint. In some cases, the spurs can actually fuse a joint, which often helps reduce pain. (Bone spurs can also form if the intervertebral disks or shock-absorbing pads between the vertebrae are injured or become dehydrated due to arthritic conditions.)
Risk factors associated with CS include: aging, injury, years of heavy lift/carry job demands, and jobs and/or hobbies that require the neck to be outside of a neutral position (like years of pinching a phone between the ear and shoulder). Genetics and bad habits (like smoking) also play a role in CS. Obesity and inactivity also worsens the severity of CS symptoms.
The good news is that even though most of us will have CS, it is usually NOT a disabling condition. However, CS may interfere with our normal activities. Depending on its location, pain may feel worse in certain positions, like when sneezing or coughing or with movements like rotation or looking upwards.
Stiffness is a common symptom, which can vary with weather changes. Too little as well as too much activity can be a problem, but the BEST way to self-manage CS is to keep active! Range of motion exercises, strength training, and walking all help reduce the symptoms of CS.
Chiropractic & Headaches

According to the World Health Organization, headaches are among the most common disorders of the nervous system affecting an estimated 47% of adults during the past year. Headaches place a significant burden on both quality of life (personal, social, and occupational) and financial health. They are usually misdiagnosed by healthcare practitioners, and in general, are underestimated, under-recognized, and under-treated around the world. So, what about chiropractic and headaches… Does it help?
Suffice it to say, there are MANY studies showing chiropractic care helps headache sufferers. For instance, in a review of past research studies using an “evidence-based” approach, chiropractic treatment of adults with different types of headaches revealed very positive findings! Researchers note that chiropractic care helps those with episodic or chronic migraine headaches, cervicogenic headache (that is, headaches caused by neck problems), and tension-type headaches (chronic more than episodic). There appears to be additional benefit when chiropractic adjustments are combined with massage, mobilization, and/or adding certain types of exercises, although this was not consistently studied. In the studies that discussed adverse or negative effects of treatment, the researchers noted no serious adverse effects.
In patients suffering from athletic injuries, particularly post-concussion headache (PC-HA), chiropractic care can play a very important role in the patient’s recovery. With an estimated 1.6 to 3.8 million sports-related brain injuries occurring each year, approximately 136,000 involve young high school athletes (although some argue this is “grossly underestimated”).
Several published case studies report significant benefits for post-concussion patients after receiving chiropractic care, some of which included PC-HA from motor vehicle collisions, as well as from slips and falls. For example, one described an improvement in symptoms that included deficits in short-term memory as well as attention problems. In this particular study, a six-year-old boy fell from a slide in the playground, and after 18 months of continuous problems, underwent a course of chiropractic care. After just three weeks of care, his spelling test scores improved from 20% to 80% with even more benefits observed by the eighth week of care!
Another case study looked at a 16-year-old male teenager with a five-week-old football injury who had daily headaches and “a sense of fogginess” (concentration difficulties). He reported significant improvement after the second visit, with near-complete symptom resolution after the fifth visit (within two weeks of care). After seven weeks of care, he successfully returned to normal activities, including playing football.
Dizziness and vertigo are also common residuals from concussion and were present in a 30-year-old woman just three days following a motor vehicle accident. She also complained of headache, neck pain, back pain, and numbness in both arms. The case study noted significant improvement after nine visits within an 18-day time frame.
What is CTS?
If tingling/numbness primarily affects your thumb, index, third, and ring fingers, it very well could be carpal tunnel syndrome, or CTS. Chances are you’ve probably had this condition for months or even longer but it’s been more of a nuisance than a “major problem” and therefore, you probably haven’t “bothered” having it checked out. Let’s take a look at some “facts” about CTS!