Physio
Condition Of The Month: Thoracic Joint Restriction

Your spine is made up of 24 bones stacked on top of each other with a soft “disc” between each segment to allow for flexibility. Normally, each joint in your spine should move freely and independently. When one or more of your spinal vertebra is slightly misaligned and restricted, we call this condition a “spinal segmental joint restriction”. A “thoracic joint restriction” means that this misalignment or restriction is located in your upper or mid-back region.
To help visualize this, imagine a normal spine functioning like a big spring moving freely in every direction. A spine with a joint restriction is like having a section of that spring welded together. The spring may still move as a whole, but a portion of it is no longer functioning.
Joint restrictions can develop in many ways. Sometimes they are brought on by an accident or an injury. Other times, they develop from repetitive strains or poor posture. Being overweight, smoking, strenuous work, and emotional stress can make you more susceptible to problems.
Restricted joints give rise to a self-perpetuating cycle of discomfort. Joint restriction causes swelling and inflammation, which triggers muscular guarding leading to more restriction. Since your spine functions as a unit, rather than as isolated pieces, a joint restriction in one area of your spine often causes “compensatory” problems in another. Think of this as a rowboat with multiple oarsmen on each side. When one rower quits, the others are placed under additional stress and can become overworked.
Joint restrictions most commonly cause local tenderness and discomfort. You may notice that your range of motion is limited. Movement may increase your discomfort. Pain from a restricted joint often trickles around your rib cage or up & down your spine. Be sure to tell your chiropractor if your symptoms include any chest pain, shortness of breath, unusual cough, indigestion or flu- like complaints.
Long-standing restrictions are thought to result in arthritis – much like the way a slightly misaligned wheel on your car causes premature wearing of your tire.
You should recognize that your problem is common and generally treatable. Chiropractic care has been shown to be the safest and most effective treatment for joint restrictions. Our office offers several tools to help ease your pain. To speed your recovery, you should avoid activities that increase your pain. Be sure to take frequent breaks from sedentary activity. Yoga has been shown to help back pain sufferers so consider joining a class or picking up a DVD.
Diet & Fibromyalgia
Fibromyalgia (FM) is a common condition that affects about five million Americans, often between ages 20 and 45 years old. FM is very difficult to diagnose primarily because there is no definitive test like there is for heart, liver, or kidney disease. Equally challenging is the ability to effectively treat FM as there are frequently other conditions that co-exist with FM that require special treatment considerations. Typically, each FM case is unique with a different group of symptoms and therefore, each person requires individualized care.
Fibromyalgia symptoms can include generalized pain throughout the body that can vary from mild to severely disabling, extreme fatigue, nausea/flu-like symptoms, brain “fog” (“fibro-fog”), depression and/or anxiety, sleeping problems and feeling un-refreshed in the mornings, headaches, irritable bowel syndrome, morning stiffness, painful menstrual cramps, numbness or tingling (arms/hands, legs/feet), tender points, urinary pain or burning, and more!
So, let’s talk about ways to improve your FM-related symptoms through dietary approaches. When the FM symptom group includes gut trouble (bad/painful gas, bloating, and/or constipation), it’s not uncommon to have an imbalance between the “good” vs. the “bad” bacteria, yeast, and problems with digestion or absorption. Think of management as a “Four Step” process for the digestive system:
1. REMOVE SENSITIVITIES: Consider food allergy testing to determine any foods the FM patient has a sensitivity for. Frequently, removing gluten, dairy, eggs, bananas, potatoes, corn, and red meat can benefit the FM patient. The use of anti-fungal and / or anti-bacterial botanicals (as opposed to drug approaches such as antibiotics) can be highly effective. A low allergy-potential diet consisting of fish, poultry, certain vegetables, legumes, fruits, rice, and olive and coconut oil is usually a good choice.
2. IMPROVE DIGESTIVE FUNCTION: The presence of bloating and gas is usually indicative of poor digestion, and the use of a digestive enzyme with every meal can be highly effective!
3. RESTORE THE “GOOD” BACTERIA: Probiotics (with at least 20-30 billion live organisms) at each meal are often necessary to improve the “good” gut bacteria population, which will likely also improve immune function.
4. REPAIR THE GUT: If the gut wall is damaged, nutrients like l-glutamine, fish oils, and n-acetyl-d-glucosamine may help repair it.
This process will take several months, and some of these approaches may have to be continued over the long term. Doctors of chiropractic are trained in nutritional counseling and can help you in this process. As an added benefit, many FM sufferers find the inclusion of chiropractic adjustments to be both symptomatically relieving and energy producing.
If you, a friend or family member requires care for Fibromyalgia, we sincerely appreciate the trust and confidence shown by choosing our services!
Carpel Tunnel in a nutshell
Here it is: carpal tunnel syndrome (CTS) in a nutshell!
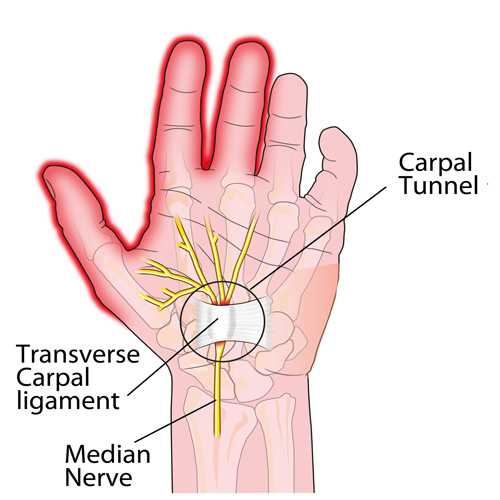
Chiropractic as THE alternative to Opioids.
In 2015, two million Americans had a substance abuse disorder involving prescription pain relievers; with more than 20,000 overdose deaths related to these drugs. In the past decade, death rates and substance use rates quadrupled in parallel to sales of prescription pain relievers.
Chronic LBP is a primary generator for opioid prescriptions. This year, both JAMA and Annals of Internal Medicine have published and supported new clinical practice guidelines that recommend prescribing spinal manipulation over medication for LBP patients.
“For acute, subacute, or chronic low back pain, physicians and patients initially utilize spinal manipulation and delay pharmacologic management.”
Research shows that low back pain patients who undergo chiropractic care have improved outcomes with lower rates of opioid use, surgery, and overall healthcare costs.
Not surprisingly, various governing bodies, including the FDA, CDC, and 37 State Attorney General’s, have concurred that physicians and healthcare decision makers should consider non- pharmacologic therapy for LBP patients. In fact, the 2018 Joint Commission guidelines mandate that hospitals include conservative options for chronic musculoskeletal pain management, specifically naming chiropractic as a potential option.
Chiropractic care is not a replacement for traditional medical treatment of LBP, rather a complementary tool to integrate within your current management paradigm. We hope that you will continue to consider our office for those cases that may be favorably served by conservative manual therapy. We are grateful for your confidence and will work hard to maintain your trust.
Do I Need an MRI?
Exercise Helps LBP!

Moving is good for your back and muscles, especially if you have back pain. Check out this link for more info!
http://www.theitem.com/stories/exercise-to-help-relieve- your-lower-back-pain,296073
Chiro & Concussions

Whiplash Associated Disorders (WAD) is the appropriate terminology to use when addressing the myriad of symptoms that can occur as a result of a motor vehicle collision (MVC). In a recent publication in The Physician and Sports Medicine (Volume 43, Issue 3, 2015; 7/3/15 online:1-11), the article “The role of the cervical spine in post-concussive syndrome” takes a look at the neck when it’s injured in a car accident and how this relates to concussion.
It’s estimated about 3.8 million concussion injuries, also referred to as “mild traumatic brain injury” (mTBI), occur each year in the United States. Ironically, it’s one of the least understood injuries in the sports medicine and neuroscience communities. The GOOD NEWS is that concussion symptoms resolve within 7-10 days in the majority of cases; unfortunately, this isn’t the case with 10-15% of patients. Symptoms can last weeks, months, or even years in this group for which the term “post-concussive syndrome” (PCS) is used (defined as three or more symptoms lasting for four weeks as defined by the ICD-10) or three months following a minor head injury (as defined by the Diagnostic and Statistical Manual of Mental Disorders).
There have been significant advances in understanding what takes place in the acute phase of mTBI, but unfortunately, there is no clear physiological explanation for the chronic phase. Studies show the range of force to the head needed to cause concussion is between 60-160g (“g” = gravity) with 96.1g representing the highest predictive value in a football injury, whereas as little as 4.5g of neck acceleration can cause mild strain injury to the neck. In spite of this difference, the signs and symptoms reported by those injured in low-speed MVCs vs. football collisions are strikingly similar!
Research shows if an individual sustains an injury where the head is accelerated between 60-160g, it is HIGHLY likely that the tissues of the cervical spine (neck) have also reached their injury threshold of 4.5g. In a study that looked at hockey players, those who sustained a concussion also had WAD / neck injuries indicating that these injuries occur concurrently. Injuries to the neck in WAD include the same symptoms that occur in concussion including headache, dizziness/balance loss, nausea, visual and auditory problems, and cognitive dysfunction, just to name a few.
The paper concludes with five cases of PCS that responded well to a combination of active exercise/rehabilitation AND passive manual therapy (cervical spine manipulation). The favourable outcome supports the concept that the neck injury portion of WAD is a very important aspect to consider when treating patients with PCS!
This “link” between neck injury and concussion explains why chiropractic care is essential in the treatment of the concussion patient! This is especially true when the symptoms of concussion persist longer than one month!
We realize you have a choice in whom you consider for your health care provision and we sincerely appreciate your trust in choosing our service for those needs. If you, a friend, or family member requires care for Whiplash, we would be honoured to render our services.
Do you have CTS?
PFPS Cont. You want details?
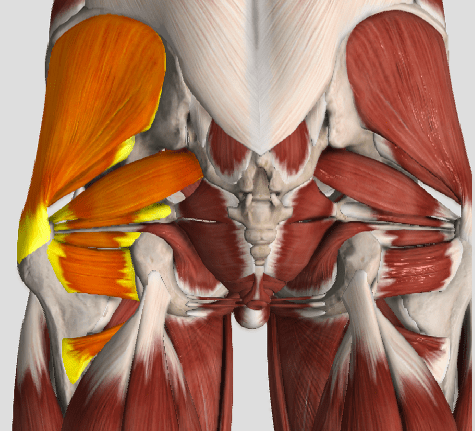
The muscles of the hip provide not only local stability, but also play an important role in spinal and lower extremity functional alignment. (1-4) While weakness in some hip muscles (hip extensors and knee extensors) is well tolerated, weakness or imbalance in others can have a profound effect on gait and biomechanical function throughout the lower half of the body. (5) Weakness of the hip abductors, particularly those that assist with external rotation, has the most significant impact on hip and lower extremity stability. (5,6)
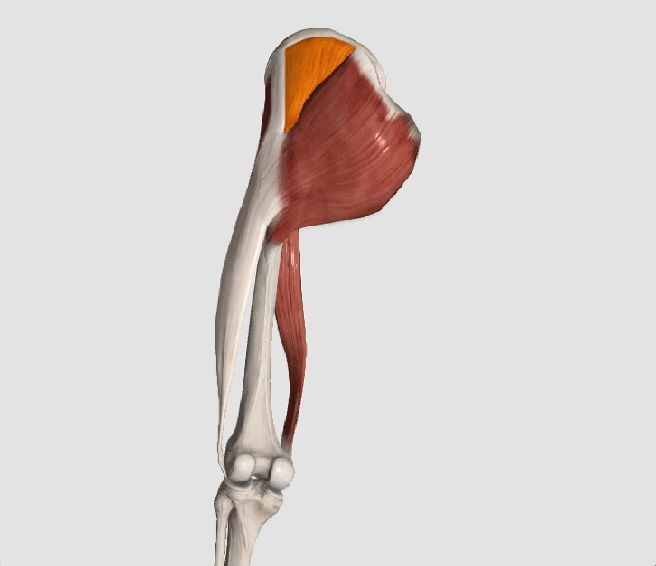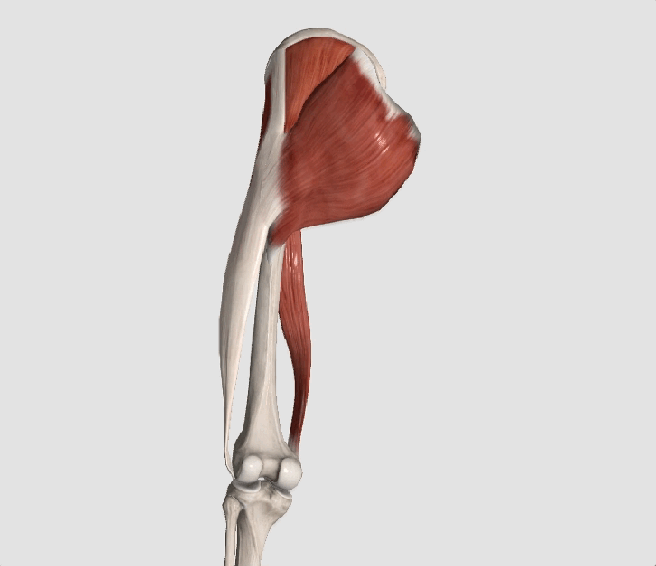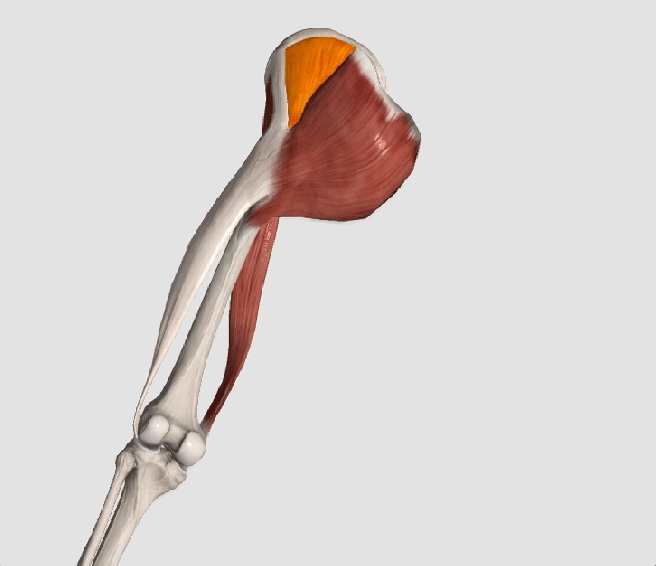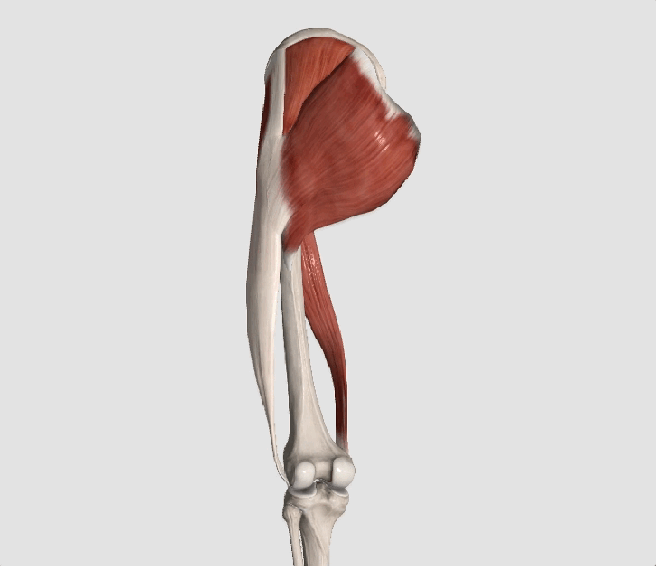
The gluteus medius is the principal hip abductor. When the hip is flexed, the muscle also assists the six deep hip external rotators (piriformis, gemelli, obturators, and quadratus femoris). The gluteus medius originates on the ilium just inferior to the iliac crest and inserts on the lateral and superior aspects of the greater trochanter. While the principal declared action of the gluteus medius is hip abduction, clinicians will appreciate its more valuable contribution as a dynamic stabilizer of the hip and pelvis- particularly during single leg stance activities like walking, running, and squatting. The gluteus medius contributes approximately 70% of the abduction force required to maintain pelvic leveling during single leg stance. The remainder comes predominantly from 2 muscles that insert onto the iliotibial band: the tensor fascia lata and upper gluteus maximus. Hip abductor strength is the single greatest contributor to lower extremity frontal plain alignment during activity. (6)
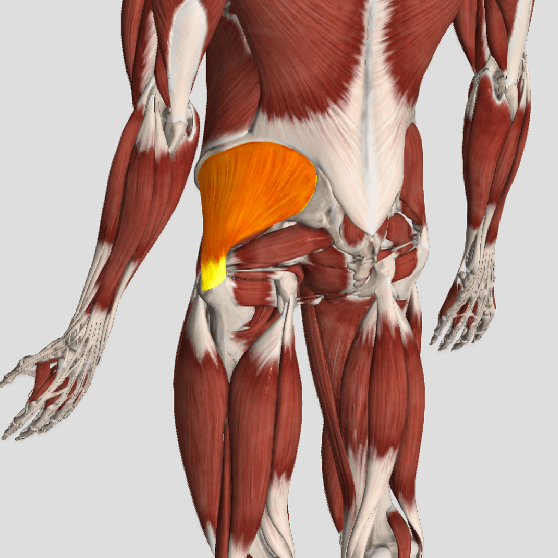
Incompetent hip abductors and/or external rotators allows for excessive adduction and internal rotation of the thigh during single leg stance activities. This leads to a cascade of biomechanical problems, including pelvic drop, excessive hip adduction, excessive femoral internal rotation, valgus knee stress, and internal tibial rotation. (1,7-12)


